Reprinted with permission from the author from the AAP’s Section on BioEthics. The perspectives within the articles reflect the opinion of the authors, and do not necessarily reflect the perspective of the Section or the AAP.
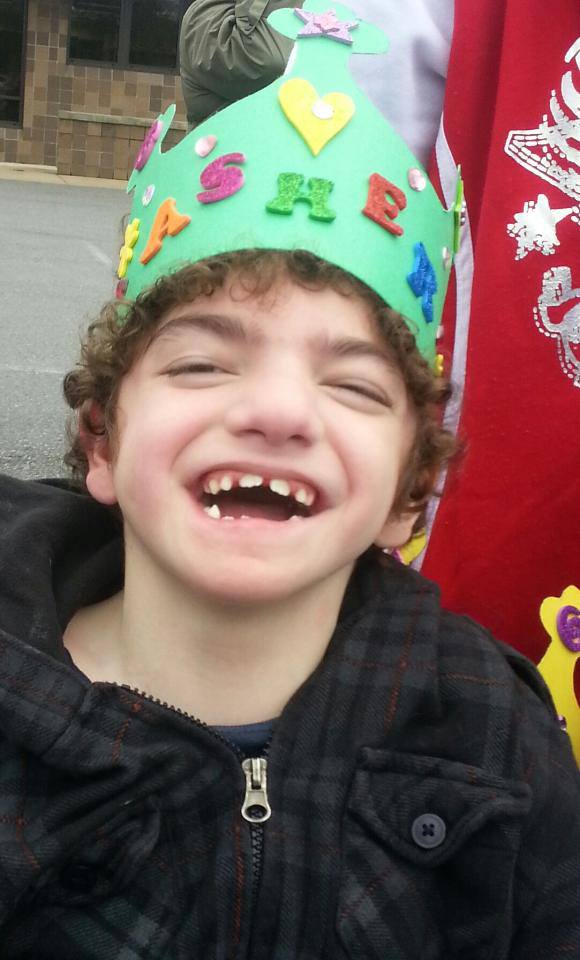
My son, Asher, died on August 18, 2013. He was medically complex and spent his entire life in and out of hospitals, most of the time in the PICU. Our family never had access to a dedicated palliative care program, however, we were fortunate that the director of the PICU had a passion for palliative care and had done some work/studying on his own.
When Asher was born, near full‐term at 39 weeks, weighing 8 pounds 6 ounces, the youngest of four children, we thought we were seasoned pros. When he had his first seizure 24 hours later and was transferred to the NICU, we realized this was going to be a different set of coupons.
We stumbled through the first two years of his life learning new terminology and new technology, integrating apnea monitors, medication regimens, an entire Day Planner dedicated to Asher’s doctor appointments and therapy sessions. At no time along the way did any of his providers talk to us about palliative care, or the idea that our child had a life‐limiting condition. He had Dandy‐Walker (and depending on who we talked to) malformation, variant, syndrome, cerebral palsy, seizures, and a wide array of musculoskeletal and other congenital anomalies that didn’t necessarily go hand‐in‐hand with DW.
We moved to be closer to family when Asher was 2 years old and got settled in with our new providers in the PICU. In and out as one of the Unit’s “frequent flyers” celebrating birthdays and most other holidays over the years, the first time we had a conversation with anyone about Asher’s fragile life was when he was ten years old. TEN YEARS OLD. Ten. And it was when we had to make the decision whether we were going to transfer him from the PICU he grew up in in Pensacola to one in Gainesville, 6 hours away, to have him undergo a laryngectomy so he could spend the rest of his life on a ventilator or simply allow him to die. We had twenty‐four hours to make the decision.
After “living” with amazing doctors and nurses who loved Asher like we did, none of them had thought to have that conversation with us until it was crunch time. In fact, they apologized to us – perhaps because all of us, deep down, believed Asher WASN’T fragile even though we were on a first‐name basis with the cleaning crew and the cafeteria folks.
It was also the first time we had to think about Asher’s care from a truly selfless perspective. This kid who could not speak had the most infectious smile and laugh; a laryngectomy would rob the world of that. He was wheelchair bound and did not use his hands effectively but when he wasn’t in the hospital he was “surfing” in the Gulf of Mexico, riding his enormous horse, Doc, or “playing” video games with his brothers and sister (he was a mean drummer on Band Hero!). And he loved Marvel movies. And riding roller coasters. How could we rob Asher of all the things he loved and the things that brought joy to his life just so we could spend more days with him? Gratefully, this team who loved Asher walked with us as we made the decision to let Asher decide when he was ready and said “No” to the surgery. That was April 1, 2011.
From that point forward, we began to have conversations in terms of, as one of the intensivists put it, “What can we do FOR Asher, not to him?” That was so eye‐opening, so freeing. As a parent, it feels wrong not to fix the boo‐boo. But when fixing the boo‐boo will cause more pain, more distress, diminish joy in your child, you have to step back. It hurts so badly, but knowing that your hurt means your child isn’t hurting (or hurting as much)…well, that’s parenthood.
We lived two more amazing years with Asher Man. That’s not a typo – I mean it: WE LIVED. More beach time, horseback riding, roller coasters, it was AWESOME! Not saying he wasn’t still bopping in and out of the PICU, because he was, and the “tune ups” got closer together and the stays got longer (oh, we didn’t see that writing on the wall either!).
When July 2013 rolled around and Asher got too tired, we knew it was about that time. I mean, we had all been here before (2011) but this was different for sure. At least we had already had the hard core “DNR” conversation in 2011 when he was discharged and again many times in the two years after.
The first one, I recall, was very awkward:
Us: “Well, what does that mean, really?”
MD: “Well, it can mean anything you want, really.”
Us: “Like what?”
MD: (lists the entire gamut of possible interventions that we could pick and choose from, like a
death menu)
Each time we had the conversation, and we had it as many times as Asher was admitted and discharged in the two years before his death, the “menu items” we chose became less and less aggressive. Again, looking at his life from a “do for, not to” perspective. When he entered the hospital for what would be his final admission in late July 2013, and the rubber really hit the road, though, we sort of had a back‐pedal moment. That’s when we really needed the guidance of our care team but they had a moment of back pedal, too, I think. Like parents, they’re fixers. They’re PICU docs and nurses. They’re in the business of saving lives, so to counsel a family that it’s time to stop must be absolutely crushing.
Finally, we did come to a consensus but we really had to press – hard. We had to insist, crying, begging, “Please, tell us what to do. You’ve been with us on this journey for 8 years. Now is the time we really need your honest guidance.” Trust me, I know it wasn’t easy for them either.
Even after the decision was made to allow Asher to hold God’s hand and find his own path, we still had moments of doubt (remember, I said it’s HARD), so we would ask for reassurance. “We support whatever decision you make.” That was probably the worst thing anyone could say to us. Tell us we’re making the right decision for our suffering baby. Tell us you know how devastated we are because you’re crying for him and for us, too, but you’re willing to let him go because you see how much he’s hurting and how tired he is. It’s okay. It really is okay to say that.
Telling me you support any decision I make just places doubt in my mind: “What do they know that they’re not telling me? Is there something we could try that wouldn’t hurt him but could save him? Are we doing the right thing? Is it US that’s tired and not him and are we being selfish?” (Yes, that last thought really does cross your mind and it’s ugly.)
Asher died with dignity and respect in the hospital surrounded by his family and second family. He’s not tired anymore.
Even though we had some bumps, we know Asher was so loved and that our family is loved. We still maintain contact with his core nurses and doctors, many of whom have gone on to advocate for a comprehensive pediatric palliative care program within our children’s hospital. I like to think Asher had something to do with that.