It was a Friday afternoon, and it was Halloween. I was beginning my weekend on-call for the pediatric palliative care team, when my pager beeped. Recognizing the phone number, I returned Allison’s call. It was about Beckett - his feeding tube had come out of place. I knew what this meant: he’d have to come to the hospital to have the feeding tube replaced by the interventional radiologists immediately. Because of his metabolic condition, Beckett could fall critically ill if he went too long without receiving fluids or nutrition. Time was also an issue because it was Friday afternoon, and the radiologists don’t put feeding tubes in overnight. Beckett lived an hour away from the hospital, and if he didn’t make it in soon, he’d have to spend the night in the hospital and get the tube replaced over the weekend.
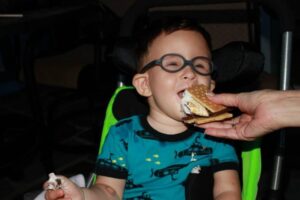 This was not a good option for Beckett, Allison or their family. Beckett, and his sister Clementine, who share the same metabolic condition, had recently been discharged home with hospice care. Allison and her husband Ben felt that Beckett and Clementine’s frequent hospitalizations, which required intensive interventions, were hindering their children’s quality of life. Instead, they chose to continue Beckett and Clementine’s complex regimen of medications and feeds, but in the comfort of their own home. They knew that as a result of their metabolic condition, Beckett and Clementine would get acutely ill, and would die – but would do so in their own home, surrounded by their loving family.
This was not a good option for Beckett, Allison or their family. Beckett, and his sister Clementine, who share the same metabolic condition, had recently been discharged home with hospice care. Allison and her husband Ben felt that Beckett and Clementine’s frequent hospitalizations, which required intensive interventions, were hindering their children’s quality of life. Instead, they chose to continue Beckett and Clementine’s complex regimen of medications and feeds, but in the comfort of their own home. They knew that as a result of their metabolic condition, Beckett and Clementine would get acutely ill, and would die – but would do so in their own home, surrounded by their loving family.
But Allison, Ben, Beckett, Clementine, Julia and Wilbur were not thinking about that now. Allison exclaimed, “But it’s Halloween!” and informed me that all four kids were already dressed in costumes and ready for trick-or-treating. I called in a favor to the on-call radiologist, who I (luckily) happened to know personally. He agreed to put the new tube in, but only if Beckett was there within the hour. When I relayed the time constraint to Allison, she informed me that they might go trick-or-treating for a short time, and then travel in to have Beckett’s tube replaced. “I didn’t hear you say that,” I retorted, in a blatant attempt to preserve plausible deniability, and assured the radiologists that Beckett would in fact, be there within the hour.
 I had seen Allison and Ben’s pictures from Halloween the year prior. Beckett’s wheelchair served as the base of the Wizard of Oz’s balloon, with Beckett (of course) as the Wizard. Clementine, Julia and Wilbur rounded out the Oz characters, all dressed for their walk down the yellow brick road. I had first met Beckett and Clementine in the ICU, but it wasn’t until I saw those pictures and heard their family’s stories that I began to understand who they really were. One of my favorite parts of working in palliative care is seeing the pictures, hearing the stories, and getting to know children with serious illness for who they really are: children.
I had seen Allison and Ben’s pictures from Halloween the year prior. Beckett’s wheelchair served as the base of the Wizard of Oz’s balloon, with Beckett (of course) as the Wizard. Clementine, Julia and Wilbur rounded out the Oz characters, all dressed for their walk down the yellow brick road. I had first met Beckett and Clementine in the ICU, but it wasn’t until I saw those pictures and heard their family’s stories that I began to understand who they really were. One of my favorite parts of working in palliative care is seeing the pictures, hearing the stories, and getting to know children with serious illness for who they really are: children.
We listen to stories and build relationships not just because it’s fun. Most parents of children with serious illnesses have to make difficult decisions for their children. And while the medical details matter, more often than not, it’s the other details about these children: what their lives are like, what makes them happy, and how they fit into their family, that carry more weight during the decision-making process. Beckett and Clementine didn’t go home to die on hospice. They went home to live. They went apple picking, got haircuts, and went to school. They took family photos and family vacations. As Allison notes in her story for Courageous Parents Network , “We made it a priority to do the really good stuff.”
When I discuss my work in pediatric palliative care, the conversation often ends quickly, or makes people noticeably uncomfortable having to talk about death, especially that of a child. It’s unfortunate that most people equate palliative care with death. I find myself explaining that while palliative care includes care of the dying, more often the focus is on living. We work to maximize and preserve quality of life, including the management of distressing symptoms (like pain, nausea or difficulty breathing), and help ensure that plans of care match children and their family’s goals. Caring for children like Beckett and Clementine, and parents like Allison and Ben, has taught me that children with serious illness and their families are living, and usually thriving, in the face of serious illness, and in the face of harsh medical realities. What Allison says in one of the Courageous Parents Network videos - “Not everyone is meant to grow old,” -- is an uncomfortable actuality that some children and their families have to face. My role, or rather my privilege, as a palliative care provider is to support children and their families in living as well as they can, in the face of unfortunate circumstances.
I often think of Clementine and Beckett and their family, the lives they led, and the lives they still lead. I also can’t help but think of the interventional radiologists, waiting, on a Halloween Friday afternoon, to replace Beckett’s feeding tube. I later found out that everyone did go trick-or-treating, and Beckett (in full lion costume) arrived an hour late. Perhaps, at some point, it crossed the radiologists’ minds that something had happened to this “hospice patient” they were waiting for, even that he had died. But no, not Beckett, he was too busy living.

