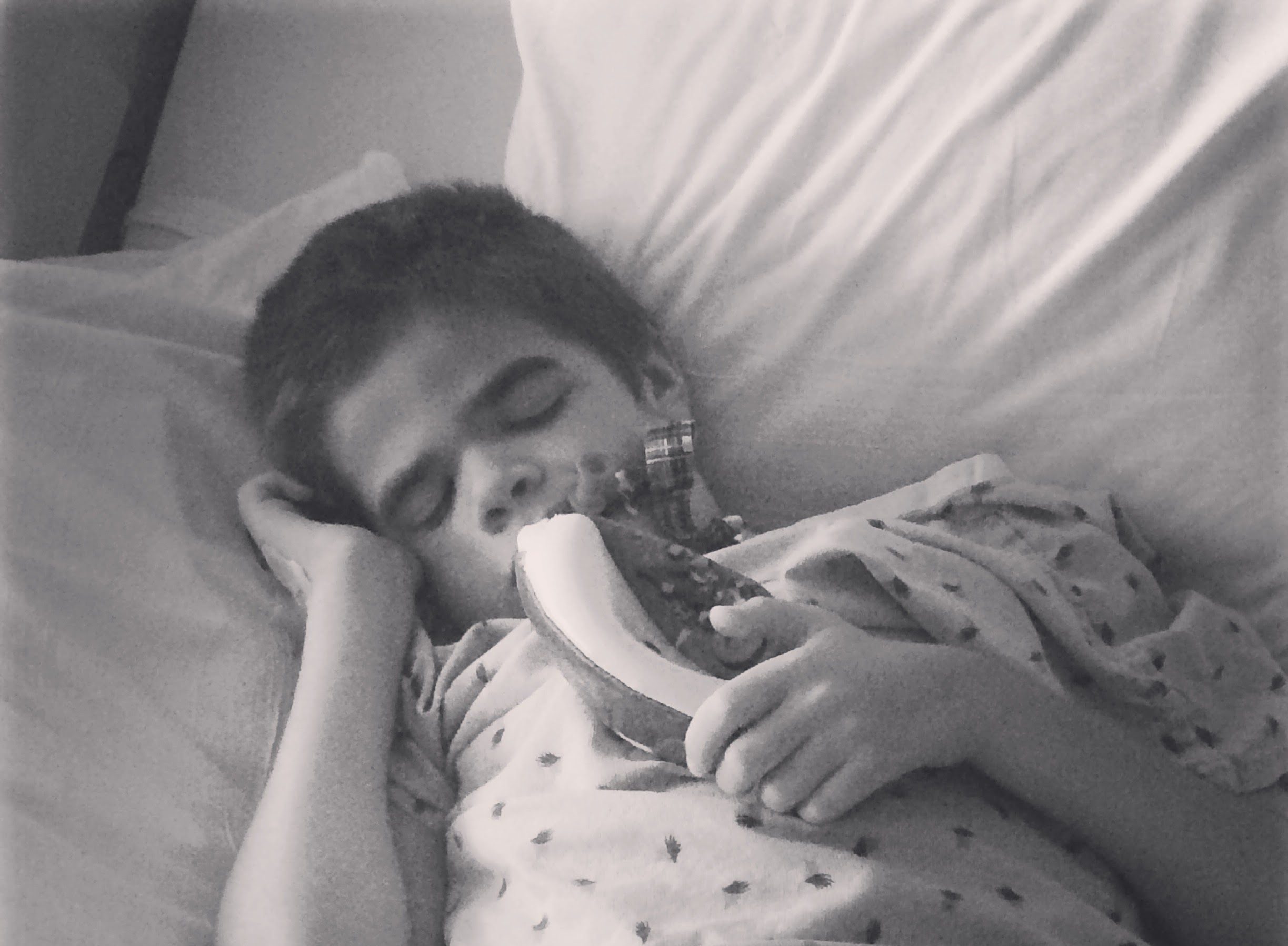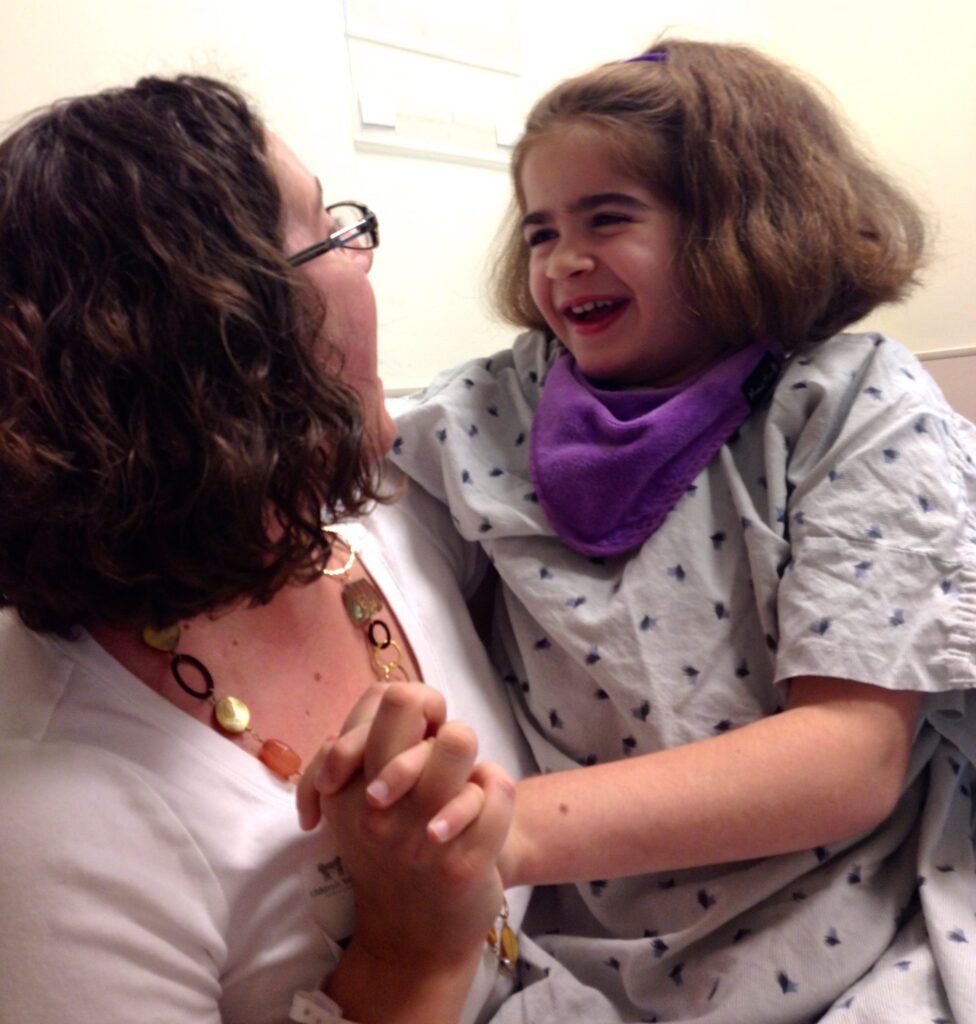
Eighteen years ago, my world was turned upside down when my daughter, Waverly, was diagnosed with Sanfilippo Syndrome. One month later, my son, Oliver, was given the same diagnosis. My family was living in London, embarking on a new career adventure when everything we had planned was no more.
My husband and I felt an extreme need to be back stateside to settle down, make a home, and build structure for the chaos we found ourselves now living. We were in a position where I could forgo my career to become the primary caregiver, devoting my time to the daily tasks of mothering two children with complex medical care needs. My husband worked to provide our family with insurance and financial stability. Most therapy appointments, doctor and equipment clinic visits, Medicaid applications, insurance appeals, and school forms were my responsibility.
In all the literature we read and conversations we had with other families, we were naïve about the impact severe neurological impairment would have on the children’s body systems as they neared the end of their lives. My husband and I made countless difficult decisions about their care. However, the most painful and gut-wrenching decisions revolved around feeding.
We opted for a G-tube when Waverly was 8 years old. She had been having trouble swallowing for several years. We thickened and puréed, but after some choking episodes, we had a g-tube placed. I took photos of her perfect belly and wept knowing our decisions were causing her to undergo surgery and pain. As parents, we weigh the options and make the best decision we can with the information we have at the moment. We constantly ask ourselves, “What is the ‘right’ decision?”
We continued with pleasure feeds, allowing Waverly to taste her favorite foods. We watched for signs of distress around eating, like squirming and crying. We noted signs of pain as we started a feed and then relief when we stopped. We would decrease rates and reduce volumes to maintain comfort. She began having more diarrhea and vomiting, spitting up formula during feeds. Waverly was experiencing edema throughout her body. We consulted with her team and made recommended changes, but her system continued to decline.
We had difficult conversations with providers we trusted. We weighed their guidance with our philosophy and ethics. I relied on my mother's intuition, but Waverly was our guide. We followed her lead. Waverly was signaling to us that her body was tired.

It took time to see that feeding her was causing her pain. We charted every feed, how many milliliters and over what period. We noted any movement or grimace that we recognized as pain. We stopped and started, gave breaks, and switched to Pedialyte. We dripped tiny amounts of food into her belly only to stop as her body showed signs of distress. My husband and I both needed to agree that it was time to stop feeding.
We transitioned into a hospice approach focused on comfort. We had time to invite loved ones into our home to spend time with her, continue to make memories and build her legacy. She died in our bed days after she turned 12 years old.
I spent a significant amount of time perseverating on our decision to stop feeding her. I would be rendered inconsolable, and overwhelmed with guilt. My husband would walk me through the events, logically laying out the cause and effects, and why we came to our decision. Repeatedly organizing the facts allowed my emotional responses to quell. I needed that framework to assuage any guilt and confirm the decisions were made to alleviate the suffering of our daughter.
And we knew we had to do it all over again with Oliver.
We were practiced. Waverly once again smoothed the path for her little brother. We noticed the signs earlier and knew what adjustments to make. Our medical team was also more versed having navigated Waverly’s decline with us just three years prior. The decisions came quicker and with a tinge less doubt. Oliver died a few weeks before his twelfth birthday.
My guilt was lessened with Oliver’s death. I felt more confident in our decisions. I also felt more supported by all of those around me. My expertise was validated by Oliver’s care team.

As parents of children with rare diseases, we are often the experts in the room, explaining the nuances of our children to those more credentialed than we are. We bring binders and share literature to inform those caring for our children. We were fortunate to have a medical team who invited us to have a seat at the table for all decisions. And if they weren’t open to that, we found another provider who was willing to say, “I don’t know” and “let me consult with others”.
Having abandoned a career and spent fifteen years as a full-time caregiver, I wanted to build upon my children’s legacy. I wanted to work in a field supporting children like mine. I returned to graduate school and became a pediatric social worker and grief counselor. I work for a community-based hospice and palliative care agency in Washington, DC.
As a pediatric hospice and palliative care social worker, I support families as they navigate complex decisions. I see my role as ensuring full parental participation and advocating for the parents’ goals of care. I am in their homes, supporting the entire family system, building trust and rapport, ideally early on so a relationship is established as decisions become more complex.
I have utilized the Courageous Parents Network both as a parent and as a professional. The educational videos were especially helpful in normalizing my experience as a mother. And I found it validating to hear others vocalize my thoughts and feelings. As a social worker, I return to the same videos with the families I support, hoping for a similar outcome.
The new NeuroJourney tool is invaluable. I wish I had access to this when I was parenting my children. However, I am thrilled to have this instrument available to my patients and their caregivers. I have introduced several families to the website, exploring the impact severe neurological impairment has on their child’s body systems. The website provides information and tools to parents and providers.
I have found the GI section especially helpful as it addresses a caregiver’s innate need to nourish their child. It provides a guidebook for one of the most challenging decision points. By using this tool, I have watched families recognize the signs of feeding intolerance and decline in their children. It opened the door to an honest conversation about prioritizing comfort and adjusting goals of care.
My hope, as both a bereaved parent who held onto guilt and as a therapist who supports caregivers experiencing guilt, is that this tool can aid in adjusting to changes and navigating decisions. This information has the potential to improve caregivers’ confidence in their choices by providing clinical data and reducing the potential for a more complicated grief process.