 The morning after we learned that my NICU graduate and newborn daughter’s 6 week MRI had indicated that her hypoxic injury left large areas of fluid where the majority of her brain tissue used to be, I resumed my in-hospital training on how to administer her peritoneal dialysis. Once she had gained enough weight to no longer need the manual peritoneal dialysis administered by her NICU nurses, my 4- week old daughter moved to the Renal Unit where for the last 2 weeks I was learning how to run her continuous cyclic dialysis machine. I was also learning how to change her bags of dialysate, the cleansing solution which helps remove the toxic wastes her kidneys cannot manage to filter out on their own. Finally, I was being trained to use syringes, sometimes with needles, to take cultures of dialysate fluid to test for infection, to inject antibiotics, and to administer subcutaneous injections to combat anemia.
The morning after we learned that my NICU graduate and newborn daughter’s 6 week MRI had indicated that her hypoxic injury left large areas of fluid where the majority of her brain tissue used to be, I resumed my in-hospital training on how to administer her peritoneal dialysis. Once she had gained enough weight to no longer need the manual peritoneal dialysis administered by her NICU nurses, my 4- week old daughter moved to the Renal Unit where for the last 2 weeks I was learning how to run her continuous cyclic dialysis machine. I was also learning how to change her bags of dialysate, the cleansing solution which helps remove the toxic wastes her kidneys cannot manage to filter out on their own. Finally, I was being trained to use syringes, sometimes with needles, to take cultures of dialysate fluid to test for infection, to inject antibiotics, and to administer subcutaneous injections to combat anemia.
I was taking on the terrifying task of learning the nursing skills associated with my newborn’s complicated peritoneal dialysis procedure in part because I was given no other choice. Her injured kidneys were taking unexpectedly long to recover so she needed to stay on dialysis until she weighed enough to handle a kidney transplant. Keeping her in the hospital until she was around 15 months old was not a viable option; therefore, we were informed we could coordinate her peritoneal dialysis procedure at our own home with a satellite medical team. This was surprising to us because neither my husband nor I had any previous medical training. In addition, although both my husband and I had played sports in high school this was not the kind of team we ever imagined participating in as a family.
Prior to the birth of our second child, my husband had been working full time while I was completing my dissertation in clinical child psychology and caring for our 2 year old daughter. My relatively greater availability made me the best candidate for running our home medical operations. The cost of the expensive home machinery would be covered by Medicaid; however, home nursing was not likely to be covered by our medical insurance. For this reason, the plan included my training.
It quickly became clear during my in-hospital training that as a bona fide clutz who tripped over her own feet while playing sports, I had made a wise decision not to pursue a medical degree. My nursing skills were so limited that the renal nurses laughed with me during my initial mishaps. Whenever my butterfingers fumbled ever so slightly while connecting her catheter to her bag of dialysate chemicals, I let out a comical little shriek–similar to the little shriek I made whenever I tripped while playing lacrosse.
I was incredibly nervous administering the sterile procedures. I was constantly afraid that my not-so-steady hands would inadvertently create a non-sterile environment and guarantee an abdominal infection called peritonitis. With the nurses’ understanding, patience and support, I slowly and surprisingly made my way through the complicated training. I grew to trust their assurances that I was learning the tools needed to avoid or appropriately deal with any mishaps I might have at home. My confidence was also boosted knowing that I would have the nurses available for consultation by phone. I put my fears behind me during the training, knowing that this complicated peritoneal dialysis procedure was the key to both our liberation from the hospital and the unification of our family under one roof.
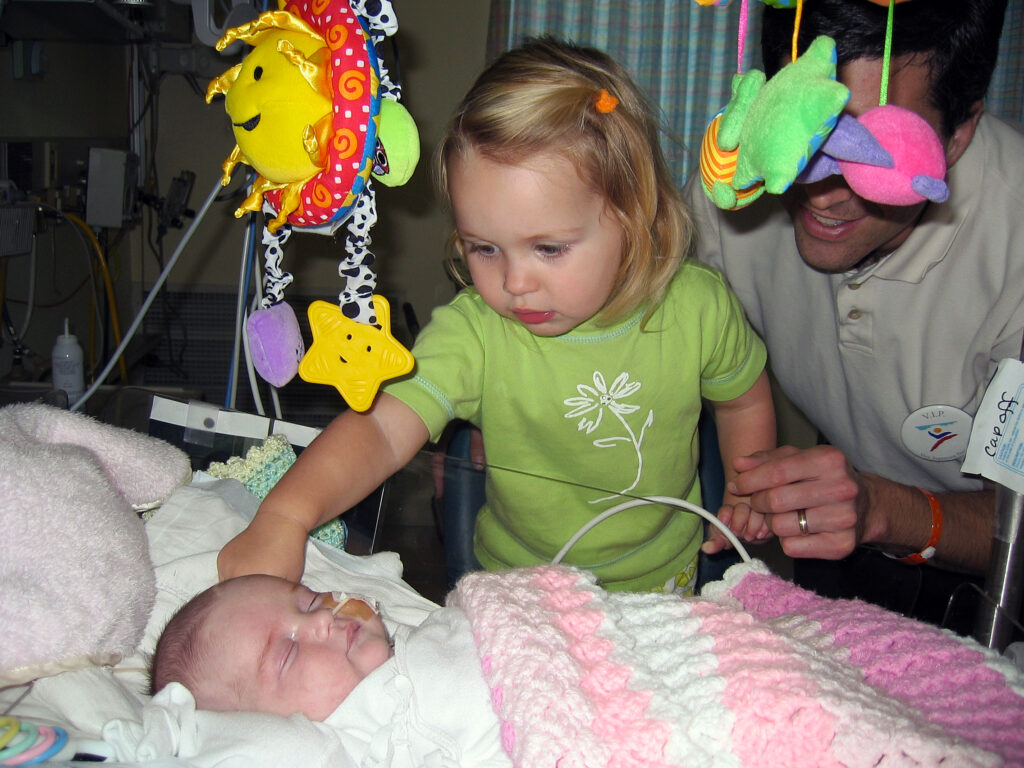 I truly hated having our family constantly split between two locations. My 2-year-old was the ultimate big sister and cheerleader who could not wait to visit her “baby sister” in the hospital. After work, my husband would come to relieve me at the hospital so I could spend time at home with my 2-year-old. I felt so torn as a mother every time I left her at home to go back to the hospital. The guilt I felt was also compounded whenever I had to leave my newborn’s bedside to spend a brief visit with my older daughter. There was no way to avoid splitting my time because I was also not comfortable potentially leaving my newborn alone in the hospital overnight.
I truly hated having our family constantly split between two locations. My 2-year-old was the ultimate big sister and cheerleader who could not wait to visit her “baby sister” in the hospital. After work, my husband would come to relieve me at the hospital so I could spend time at home with my 2-year-old. I felt so torn as a mother every time I left her at home to go back to the hospital. The guilt I felt was also compounded whenever I had to leave my newborn’s bedside to spend a brief visit with my older daughter. There was no way to avoid splitting my time because I was also not comfortable potentially leaving my newborn alone in the hospital overnight.
My husband and I were both together in her hospital room the day after we met with the neurologist to discuss her devastating MRI and severe neurological diagnosis. Two nephrologists casually entered my daughter’s room, bringing two chairs with them. After informally greeting my husband and me at her bedside, they positioned the chairs next to each other on the side of the room closest to the door and sat down. I should have known instinctively that this was not a good sign based just on the fact that they never sat down during bedside rounds. Another clue that we were about to face an additional unexpected curve ball was that our daughter’s attending Nephrologist was joined by the Chief of the Nephrology Division, who was also the Medical Director of the Dialysis and Kidney Transplantation Service. We were still reeling from last night’s heartbreaking news that she was at risk for seizures, cerebral palsy, and intellectual disability, so I naively assumed that they had seen the MRI and were both here to comfort us.
The Chief started speaking while the attending nephrologist remained silent. In a calm, warm manner he confirmed that my daughter’s renal team had reviewed her MRI and then told us that because of her severe brain injury, her potential poor quality of life, and the transplant surgery risks to her and her donor (me), she was no longer a kidney transplant candidate.
My husband and I were blindsided. We froze with confusion and shock as we digested that she was now being denied a transplant. Her team had told us decisively that home dialysis was a bridge to her transplant. The doctor paused for questions, which normally would have been helpful because it can be hard to quickly process any new medical information but our shock prevented us both from saying anything really.
Thankfully, our daughter was asleep during this meeting because I was in no condition to care for her. My chest tightened and my throat closed while my focus intensely narrowed in on just the four adults, making the room uncomfortably smaller. My confusion and fear started to overwhelm me once again even though we had already faced so many uncertainties since her birth. It did not help that we had been lulled into complacency, knowing that her dialysis was successfully doing the work of her failed kidneys by removing all the toxic waste products from her body. We had not been preparing for her death but preparing instead to bring her home to wait for a life-saving transplant. Furthermore, she had inherited my blood type and I was already intent on donating my kidney. In that speechless moment, my weeks of training reminded me that without a kidney transplant, we would ultimately lose my daughter.
I did not understand why they had suddenly turned on their heels and unilaterally made this decision. This abrupt change in plan robbed our family of a future that was already filled with atypical hopes because of her severe brain injury. I looked at my husband who was stoic and focused on the doctors. Recognizing that we were still processing what he told us and not yet ready to ask questions, the Chief continued with an explanation that he likely suspected we were craving. I forced myself to focus and listen carefully while he clarified. He told us that had they originally known the full extent of our daughter’s brain injury they would not have initiated her dialysis because it is an incredibly heroic medical procedure for a newborn. Indeed, they first suggested peritoneal dialysis for her kidney failure just days after pediatricians had aggressively resuscitated her at birth. They had told us her condition was so fragile that there was a chance we might lose her from catheter placement surgery itself. However, they thought it was the right thing to do at the time to give her the best chance of survival.
We had signed a form that indicated our acceptance of the 20 percent chance we might lose my newborn to try and save her life (for the second time). Now, without warning they had altered the plan. When I had begun to process the original reasoning the Chief had shared, I grasped at my fleeting hopes, sandwiching them in a bunch of dreaded “what ifs” in my head: If I was a match, if I was healthy enough …. and if I was willing to take on the risks of surgery to give my daughter my kidney …. why were they unwilling to do the family-based surgery and just remove her from the national transplant list? I believed that because it was my body, it was my choice to take on and sign away the risks of a transplant for both of us as my daughter’s likely donor and her parent.
The Chief seemed to know what I was thinking and added firmly that we could ask other doctors at other local children’s hospitals if they would do the transplant, but that we would most likely discover they followed the same protocols and would reach the same conclusion. Now my throat was closing again, squeezing my vocal chords so tightly I could feel the lump developing and barring any speech. However, my husband managed to ask what would happen next.
The doctor explained that we could choose to keep her on dialysis or stop it and bring her home. Her need for a transplant would remain, so keeping her on dialysis would not sustain her life indefinitely. He paused for what seemed like an eternity to let this sink in. He told us that we could take as long as we wanted to decide and ask as many questions as we needed and that the team would support any decision we made. Then they left us alone to make one of the most difficult decisions parents could ever have to make for their child. Over the next week, we watched our daughter closely and spoke to her team members at length about the true consequences of each option.
Initially, I resented her doctors for forcing that difficult choice upon us by deciding that they would not conduct her kidney transplant surgery. They had defaulted on their original plans for her at the last minute, suddenly pulling the rug out from under us. In this confused and angry state, I wondered if their offer to allow her to stay on dialysis indefinitely was designed only to placate any distress caused by their sudden refusal to do the life-saving transplant.
The next day I again helped hook her up to the large machine that took over her kidneys’ job of removing the toxins from her body. The moments she was hooked up suddenly took on an even more powerful meaning than my self-righteous anger. I watched her wince in pain with every drain and tried my best to comfort her, often unsuccessfully. The powerful machine was pulling at her insides to drain excess fluid and failing to sense that her abdominal space was already free of fluid. Similarly, my heart was being pulled in two directions thinking of the decision we had to make. I could not bear to see my baby in so much pain from the tugging, which medications could not reduce. I also could not bear the thought of losing her so soon without this life-saving medical procedure. As her mother, I was still struggling with unnecessary guilt that I may have somehow missed signs of her compromising birth conditions in the hours before I had started bleeding at home. I also had a hard time managing thoughts that equated stopping her dialysis with giving up on her.
I acknowledged my personal struggle related to concerns of abandonment to one of my daughter’s nurses. She candidly shared her opinion that I had done absolutely everything in my power thus far to give her the best chance to survive and that it was her doctors who had abandoned her by refusing the transplant. She also shared that she thought my daughter’s developmental issues and medical complications could mean she would eventually need to be institutionalized. While this was a bit much for me to process at the time, her honest perspective released me from my guilt, allowing me to finally start to explore the kind of life I truly wanted for my newborn and our family.
I knew that as her parents, my husband and I would do whatever we could to manage the uncertain prognosis associated with either option. There was no doubt because we had already done this on our daily rollercoaster ride in the weeks since our daughter was born. However, her extremely fragile condition made the mother in me become immediately concerned about her older sister’s well-being. Unfazed by all the extra equipment, she adored her baby sister and had been asking for weeks when she was going to come home. I did not know how we were going to tell her that with either option her sister might not live the life she expected. We also imagined that the constant focus on and worry about our newborn would frighten or alienate her. We needed powerful words to communicate her precarious condition and poor prognosis to her sister, who was too young to even comprehend why her sister faced the challenges she did.
 We spoke to our daughter’s team who predicted that off-dialysis we could expect only days, weeks, or months at the most with her. Hearing this, I cried unapologetically. Looking back, this was the first time her doctors had seen me cry, because I had previously only been focused on overcoming day-by-day health challenges without any hint of such a bleakly restricted future. When I expressed concerns about her older sister’s ability to cope, a psychologist from the palliative care team who specialized in working with siblings of children with terminal illness came to our daughter’s room. She encouraged us to tell our 2-year-old in concrete terms that her sister’s kidneys were broken and that her doctors cannot fix them so she will die soon. She also told us we would not be alone because we would have hospice support and therapists available to guide our family through the next steps at home if we chose to stop her dialysis. With my fear of the unknown eased a bit, I was able to focus more on my own personal concerns as her mother.
We spoke to our daughter’s team who predicted that off-dialysis we could expect only days, weeks, or months at the most with her. Hearing this, I cried unapologetically. Looking back, this was the first time her doctors had seen me cry, because I had previously only been focused on overcoming day-by-day health challenges without any hint of such a bleakly restricted future. When I expressed concerns about her older sister’s ability to cope, a psychologist from the palliative care team who specialized in working with siblings of children with terminal illness came to our daughter’s room. She encouraged us to tell our 2-year-old in concrete terms that her sister’s kidneys were broken and that her doctors cannot fix them so she will die soon. She also told us we would not be alone because we would have hospice support and therapists available to guide our family through the next steps at home if we chose to stop her dialysis. With my fear of the unknown eased a bit, I was able to focus more on my own personal concerns as her mother.
It was exceedingly painful for me to even think about losing my daughter. I wanted more than anything to help my newborn daughter survive for as long as possible by running her life-saving dialysis every night at home. However, with every painful drain for her the powerful dialysis machine created, my aching heart made me see that I was not being the advocate my voiceless daughter desperately needed. I was being a coward, so afraid of facing her eventual death that I was forcing her to experience tremendous pain just so she could remain with us. Repeatedly witnessing her inconsolable moments on dialysis made me realize I did not want her to be in pain because of me. I came to understand that I needed to protect her quality of life even if it meant limiting the quantity of her life.
My husband agreed with this philosophy. He knew this was the path he wanted to take before I did. Still, he gave me the space I needed to make up my own mind. He shared his concern that the longer our daughter lived, the harder it would be to lose her. Fear of getting attached, however, was not the issue for me. During moments of uncertainty and instability, such as when doctors initially could not find my baby’s heartbeat after I arrived at the hospital bleeding and leaking amniotic fluid at 38 weeks pregnant, I briefly tried to shelter myself from the pain of losing her; however, every time her health shifted toward stabilization my bond continued to deepen and strengthen my attachment.
 With a new comfort care philosophy leading the way, my husband and I decided to bring our daughter home pain-free off-dialysis and on home-based hospice so she could enjoy the love of her family liberated from everything else, including our own fears of her dying. Putting her needs first was not only evidence of our intense love for our daughter but also how I felt the true power of that love for her for the first time. Indeed, her big sister responded to our well-crafted statement about her sister’s broken kidneys with a resolute “Well, I’ll fix them!” Her sister’s unwavering determination reminded us that our family was strong and tenacious enough to give our newborn the love-filled life she deserved. Once stabilized off-dialysis, she was discharged home at almost 2 months old.
With a new comfort care philosophy leading the way, my husband and I decided to bring our daughter home pain-free off-dialysis and on home-based hospice so she could enjoy the love of her family liberated from everything else, including our own fears of her dying. Putting her needs first was not only evidence of our intense love for our daughter but also how I felt the true power of that love for her for the first time. Indeed, her big sister responded to our well-crafted statement about her sister’s broken kidneys with a resolute “Well, I’ll fix them!” Her sister’s unwavering determination reminded us that our family was strong and tenacious enough to give our newborn the love-filled life she deserved. Once stabilized off-dialysis, she was discharged home at almost 2 months old.
Surrounded by her adoring family members and much to everyone’s surprise, her kidneys rallied. We were given the gift of not just days, weeks, or months, but an incredible ( still medically challenging) 12 years with our sweet daughter.
Erin is a Licensed Clinical Psychologist and the author of Adapted World, a blog filled with ideas to adapt equipment and everyday items for children who have multiple severe disabilities. Her blog also documents the life experiences of her medically complex daughter, including family adventures and interactions with her older sister and younger brother.