There doesn’t seem to be a word to describe what it feels like for a parent to first hear the name of their child’s diagnosis. I tried to name the feeling – catastrophic, devastating, scary.
None of these terms fully encapsulates the experience; the way the name of the disorder stuns and disorients. What word describes what it feels like to live inside a snow globe that is suddenly and violently lifted and shaken relentlessly?
My blonde-haired, round-faced, full-smiled, running-never-walking, 3-year-old Anni couldn’t possibly be the bearer of such a complicated term like “mucopolysaccharidosis.” She could easily navigate a playground, a dinner plate, and a preschool classroom. How was she going to navigate a disease that would relentlessly steal her skills, leaving seizures and a feeding tube as a consolation prize?
I didn’t know on that diagnosis day – the day I sat on my living room floor hearing the words, “Don’t Google it” – how much would be asked of our family. I only knew enough to be terrified and heartbroken, stuck on a repeating loop: How? How? How? How would I ever be okay again? How would I make a life for her that wasn’t a downward spiral of hopelessness? That day, it felt like someone pressed the diagnosis into my hand, and I knew that I would never put it down.
When I learned about my daughter’s diagnosis, I also discovered how much I had quietly and automatically assumed on the day I found out I was pregnant about what her life would be like. I expected sleepovers. I expected school plays. I expected late nights introducing her to movies that I grew up with. I expected teenage years of eye rolling and slammed doors. I expected broken curfews and negotiations about borrowing the car. I expected a normal amount of heartbreak. I expected to live longer than her. I didn’t expect to hear “mom” a limited number of times. I didn’t expect to have to thicken water in her sippy cup, so it wouldn’t leak into her lungs. I didn’t expect to have to carry her when she was a teenager. I didn’t expect I would change her diaper beyond 3 years old.
What do I wish I had known in those early days after her diagnosis? What did I need that I couldn’t find on Google? I already Googled what the disease meant for her. What I didn’t know – what I wanted to look up – was whether I would be able to handle it all. If I were sitting on the other side of that question, answering my 28-year-old self, staring at a brand-new diagnosis, here’s the most honest answer I could give to this question:
Am I going to be okay?
Answer: No. Then yes. Then no, no, no. Then yes again.
A huge part of grieving Anni’s diagnosis and the life I thought we would have together was acknowledging that this type of thing happens, and happens often. Terminal diagnoses are not rare. Even rare diseases are not rare in the grand scheme of human suffering. A mother losing a child is not actually that unusual. I had to grieve that an uninterrupted cosmic “yes” is not something any of us are promised.
I remember sitting with Anni after she had lost most of her speech. We snuggled and stared into each other’s eyes, without words, for what felt like forever. And in that moment, nothing needed to be different – not her diagnosis, not what was coming. The grief was there, and the love was there, and they were the same thing. We were just two people looking at each other.
I didn’t expect this life to be so full of love. I didn’t expect that caring for her body would be more than changing diapers. I didn’t expect the people I would meet who would work very hard to make her life full of good experiences and meaningful inclusion. I didn’t expect to become part of a community that intentionally turns their heartbreak into positive action. I didn’t expect such an expansion of joy.
My perspective on joy isn’t about putting a positive spin on things or hunting down a silver lining. It’s not “just focus on the positive” messaging because doctor appointments, IEPs, and a DNR can be relentless, exhausting, and sorrowful – they are always there. If we focus only on the positive, it would be like looking at our life through a pinhole. I don’t want a pinhole, I want a wide-eyed, courageous panoramic view of it all.
In the 14 years since her diagnosis, I’ve learned that moments of joy are not few and far between. They’re not moments that are meant to sustain you until the next heartbreak. They’re not moments of reprieve in a long line of disappointments and frustrations. What I slowly learned is that living a full life means viewing all moments with equanimity. The dark and luminous alike are necessary for the full human experience. None of us gets through life unscathed, but the gift of living goes to those who learn to invite in both the prickly and effervescent – to sit with them, to listen, to let them stay for a while.
Remember the word I was looking for to describe receiving a diagnosis? Maybe it’s tricky to find that word because the experience itself is so complex. Maybe it’s a word that can only be written with hindsight.
So I invented one:
Excruliance
excruliance (ek-skroo-lee-əns) noun, excruciating + radiance
The simultaneous experience of devastation and illumination; the overwhelming, clarifying, heartbreaking, and ecstatic feeling that arrives when a moment is too vast for any single emotion to contain. Often felt when love and loss become indistinguishable from one another.
“The diagnosis did not destroy her — it arrived with an excruliance she would spend years learning to name.”
As I write this, Sasha is screaming. Not the kind of vocalizations you might hear at a restaurant or department store and realize someone with a complex disability is in the vicinity. This screaming is a pupils-dilated, faced-flushed, blood-curdling kind of shriek. If you were to zoom in further, you’d see her uvula swinging violently in the back of her throat – something right out of a horror movie. My husband employs noise cancelling headphones during these episodes, while Sasha’s four-year-old sister calmly states, “Sasha, it’s too much.”
These episodes have long been a part of parenting Sasha and living alongside her. In her early years, they tended to be nocturnal. As the sun set, an internal switch would flip on and Sasha would start pacing and screaming. We would hear yells anytime she got cold, whether from a window being down while driving along a highway or from missing a blanket when watching television. Nowadays, a screech may occur when she wakes from a brief catnap and feels disoriented. We always hear one when she is uncomfortable from wetness in her incontinence brief. But mostly – and like clockwork – this behavior occurs during menses. Period Power is the term my husband has dubbed it, referencing the surge of energy, mania, appetite and sleepless nights we often see during “that time of the month”. Each cycle has brought challenges for us as caregivers, and also unexpected, miraculous strength to Sasha’s body.
Sanfilippo Syndrome carries with it a myriad of complexities. Sasha was six when her seizures began. With them came a loss of skills, which was shocking and particularly devastating because we did not yet know her diagnosis. Witnessing such a small, young individual go into convulsions brought a helplessness no parent should ever know. As time moved on, the seizures worsened, and our pediatric neurologist shared that seizures beget more seizures. Eventually, Lennox-Gestaut, a typically intractable seizure disorder, was diagnosed. Ativan was prescribed to halt the cluster events; and a new protocol was in place as we cautiously moved forward.
This intervention mostly worked for a few years to come. Every six weeks, Sasha would have a grand mal seizure for about thirty seconds; we’d administer a tiny tablet of Ativan between her back teeth and cheek, and she would fall into a deep sleep for about sixteen hours. A worrisome occurrence to witness, such deep sleep without stirring, but the potential for a seizure wave and crest was mitigated. Sasha would gradually resume her baseline state of awareness and functioning and life went on. That is, until adolescence.
The teenage years arrived, and with them, hormones. Hormones meant more seizures. Six weeks apart became four, then four weeks apart became two, until they eventually hit a worrisome new frequency where Sasha was having seizures every five days. I’ll never forget the day I told her neurologist that I feared a seizure would be the medical event to take her life. If this shrinking timeline continued, the five day interval would become a two, and then every two days would eventually become one. The daily strain of seizures – those were such harrowing years.
In an urgent conversation, he finally mirrored my worries, and he started combining meds in an attempt to reset Sasha’s neurological hardwiring. We had amazing results with a two medication “cocktail” and suddenly watched our wall calendar transform. Once riddled with red circles marking epileptic events, the calendar began to reveal white spaces. The circles grew further apart. More and more white spaces appeared. Calendar pages turned as days turned into weeks and weeks became months. We had struck gold.
While her menses no longer triggers seizure events, it does still have its challenges. Sanitary care was initially quite difficult, as her fully able body was paired with the developmental understanding of a toddler. But as with any medical decision in this rare disease world, deciding whether or not to medically intervene with her hormone cycle was not simple. If I could count the number of times someone said to me, “Life will get so much easier when….,” I would be a very wealthy individual.
For the past fourteen post-puberty years, I have chosen to not (yet) intervene with Sasha’s menses. Behaviors of sleepless nights, screeching vocalizations, frantic pacing and voracious eating are par for the course each and every month. We opt not to travel via airplane, or stay in hotels or rentals with shared walls due to the potential for unexpected screeching episodes. They are incredibly alarming to hear, and I often find myself waiting for police to be called by well intended strangers. While Sasha’s monthly cycles are fairly predictable, they do have a tendency to slightly shift, making travel planning challenging. Sasha experiences urinary retention every month as her cycle approaches, as well withholding the ability to void for upwards 16 hours. Are there medications that can address all of this? Absolutely. Injectable, oral, non surgical and minimally surgical offerings are all at the ready should we wish to pursue them. How effective they will be for a rare disease individual can vary greatly. If they will be a game changer for the better, or conversely, the card that makes the house of cards tumble – we do not know. I live every day, Sasha lives every day, in a house of cards. Her foundation is not built on sand, but her roof can be made wide open to the elements ever so easily.
There’s a host of reasons why I wait – that for all of these years of screeching, I keep pausing. For one, Sasha cannot tell me if she is experiencing a side effect, and more importantly what that side effect is. Women typically follow their mother’s gynecological history; and for me, I had severe mood swings any time I took hormones, and as a monthly migraine sufferer myself, this would also be a concern for Sasha. Second, there is the chance for weight gain. With Sasha being nearly immobile now, it is important for her health (and for our backs!) that she remains at a relatively consistent weight. Neurologically speaking, estrogen tends to increase neuronal excitability, lowering Sasha’s seizure threshold. We are therefore limited in medication options and would need to use progesterone-only compounds so as not to risk the return of seizures. And there is one oddly unique reason holding me back: Sasha’s stamina.
Every month as Sasha’s period approaches, along with the negative behaviors come unexpected positives – increased strength and a return of mobility. During the week leading up to Sasha’s period, she stands on her own volition, with me only holding her hands for balance, and takes self-initiated steps. For one week, every month, I can get Sasha to walk through multiple rooms in our home. In warmer months, my husband follows behind us with her wheelchair as we walk portions of our neighborhood. It is fleeting but amazing. As the period comes, stamina wanes, energy levels dip, and we are back to a two-person assist at her best, and the hoyer lift at her worst. I am so fearful to risk the loss of this sacred week of strength should we alter her hormone cycle. I simply cannot consider it.
I relay my reasoning to Sasha’s providers every six months. I do not disavow the negatives. I treat Sasha with over-the-counter medications for suspected cramping and headaches, monitor her hydration closely and gently apply warm compresses to her abdomen. And in our cupboard sits a month-long prescription of norethindrone, waiting for me to give it a try. But nothing is simple in this rare disease world. What might look like an obvious medical solution from the outside is, for us, a calculation of risk, memory, and hope — and for now, I choose to wait. Some decisions are not about making life easier; they are about preserving what is miraculous.
 Joanne Huff comes to Courageous Parents Network as a long time follower and parent enthusiast of the organization. As the Mother of two girls, the oldest of whom has the rare disease MPS IIIA/Sanfilippo Syndrome, Joanne has benefited tremendously from the intimate parent interviews and candid, vulnerable story sharing throughout numerous thought provoking blog posts. As her daughter’s activities and lifestyle started to slow down with disease progression, CPN became a larger anchor in times of uncertainty and unrest. It is through this lens that Joanne hopes to share experiences and insights via the CPN blog.
Joanne Huff comes to Courageous Parents Network as a long time follower and parent enthusiast of the organization. As the Mother of two girls, the oldest of whom has the rare disease MPS IIIA/Sanfilippo Syndrome, Joanne has benefited tremendously from the intimate parent interviews and candid, vulnerable story sharing throughout numerous thought provoking blog posts. As her daughter’s activities and lifestyle started to slow down with disease progression, CPN became a larger anchor in times of uncertainty and unrest. It is through this lens that Joanne hopes to share experiences and insights via the CPN blog.
Joanne completed nursing school after her daughter’s diagnosis, receiving her Bachelors of Science in Nursing from Plymouth State University, Plymouth NH. She enjoyed community liaison work with home care providers of adults with special needs up until her own daughter’s care became increasingly more involved. In addition to serving on the Boards of New England Regional Genetics Group (NERGG) and Adaptive Sports Partners through 2024, she has found great purpose in volunteer work advocating for policy improvements and change in Washington DC with the National MPS Society. In her free time, Joanne seeks balance and refuge with yoga, hiking and performing as an ensemble Soprano vocalist with the Pemigewasset Choral Society. When not blogging for CPN, Joanne enjoys sharing offerings on her personal Blog Folding Origami for God. She resides in Bow New Hampshire with her two daughters, Sasha and Nika, her husband Mike and her yellow lab Suki.
I consider myself an advocate through and through; not only for my daughter, who struggles with a rare disease, but for the causes I feel are in her best interest. To that end, I want to remind all parents of children with rare diseases and complex medical conditions that you know your child best. This is true for two obvious reasons. First, we typically spend the most time with that child providing clinical care and parental oversight. Second, by definition, a rare disease is just that – rare. This suggests not a tremendous amount is known about the given condition we find ourselves navigating. For those two reasons alone (there are more!) it is so important to listen to our inner voice, our gut and our past experiences.
There have been many times over the years where I’ve needed to find my voice and politely request more. More support, more budget, more space or more time. Whether it meant pausing on the idea of overnight summer camp and choosing day camp instead, questioning the timeline of a medication titration, electing to place a G-tube, or seeking out the most supportive seating for Sasha’s evolving postural needs, these were moments that required careful consideration. There were times when I stood back during meetings—while touring a camp at an open house, attending an appointment with a neurologist or surgeon, or meeting with a DME representative—when I needed to gather my thoughts, analyze the information in front of me, and advocate for what was important and what was right.
At other times, my advocacy is hindered by unrealistic expectations. This happens when I enter an appointment expecting complete alignment between provider, patient, and parent. I want to feel fully seen and understood. I want the clinician’s knowledge to be vast, their understanding of her syndrome complete, their answers certain. From that place, I imagine a dialogue unfolding effortlessly, clarity expanding without limits.
Of course, this is an unrealistic expectation at best, and at its worst, deeply irrational – especially when caring for a child with a rare disease. It’s as though I am searching for someone omnipresent, omnipotent, omniscient.
with a rare disease. It’s as though I am searching for someone omnipresent, omnipotent, omniscient.
When such overly hopeful expectations are not met, I recognize the moments when I dig in my heels under the banner of advocacy. In my disappointment at the absence of concrete answers, I cling to the belief that I know more, that I know best, that I alone am the expert. And in doing so, collaboration stalls. I hear only superficially what the provider is trying to convey.
It’s while standing at that forked road that collaboration breaks down. This is when I overlook a provider’s deep experience, especially when it is not specific to my daughter’s disease. Advocacy needs to be rooted in realistic expectations; when mine blur, everyone loses, potentially most of all, Sasha.
These are the times when I’ve had to let go of my attachment to an idea, perhaps to even an ideal. Yes, I care for a child who is rare. Yes, there is a good chance when a specialist new to her care team approaches, they have perhaps never met a child with Sanfilippo Syndrome. I am often asked if medical residents can be present in an exam room when Sasha is receiving routine care at our state’s teaching hospital; and I am pleased each time I am asked this and gladly agree. Each interaction means one more future medical provider who can say, “I have seen Sanfilippo Syndrome before”.
Sometimes I pause when a remarkable medical provider shares that they have never treated a child with Sanfilippo Syndrome. I must remind myself that this neurologist has seen hundreds of children with epilepsy, that the speech language pathologist in front of us has conducted countless swallow studies, that our PCP has faced challenging confounding variables, that virtually all geneticists have treated numerous other rare diseases. It makes me ask, “What if both concepts can be true – that I know my daughter best and the provider might also be right?” As we both gain knowledge through managing my daughter’s care, we all might expand and grow together.
Recently, I pushed back against a recommendation from Sasha’s neurologist to titrate down one of her anti-seizure medications. For many reasons, I found his recommendation to be particularly bold. Sasha has a form of epilepsy known as Lennox-Gestaut, which tends to be very resistive to medications. There was a point in time just over a decade ago when her seizures became so severe it looked like the seizures, and not so much Sanfilippo Syndrome, would be the medical event to take her. We were tremendously fortunate to find something that’s worked these past 12 years. Why rock the apple cart now? I was able to offer this perspective and history to the neurologist, and we’ve been able to more cautiously approach dosing changes while maintaining her seizure control. What a pivotal moment that was. Through collaboration, a sense of harmony was forged within her care plan.
At another appointment this past year, when meeting a new geneticist, I was excited to glean some insight into some of the more challenging symptoms to recently arise for Sasha. She had never treated a child with Sanfilippo Syndrome before, but she had treated a patient with a very different rare syndrome, an individual who was also an outlier in the life expectancy for her given condition. Much like Sasha, this child also suffered the same challenging symptom Sasha was experiencing. Again, like Sasha, this symptom was uncommonly found in the comparable rare disease. Parallels were drawn by our new provider in real time, and data gathering was soon underway. This could one day enhance understanding of both syndromes. I am grateful for this provider for thinking outside the box and sharing her insights.
At Sasha’s annual physical in 2024, as her PCP brought the appointment to a close, she stated, “with Sasha doing so well right now, would she be interested in attending summer camp next year?” I was floored, with an initial (internal) reaction of “are you crazy?!” I now stand back in this new year underway. As I assess the alignment of many of my responses over the years, I recognize that my baseline is often to resist. The camp experience ended up being an unforgettable one for Sasha and our entire family, with tremendous meaning imparted to the entire household. To this day, new habits remain in place for Sasha’s betterment stemming from a single week at camp. Her little sister Nika picking out Sasha’s daily outfit, me checking the forecast each morning to see if we can safely be outdoors, my husband shopping for a land yacht of a handicap vehicle to ensure travel and adventure in all seasons. All of us are mirroring our roles from that sole week of summer camp.
All of this is to say, when I walk into a medical provider’s exam room, they have no idea the depth of the well that holds Sasha’s entire story, her traits, her personality, her medical history. But maybe, I don’t always appreciate the depth of their well either. As caregivers, we are the leader in our child’s care. We truly do know them best. But our care team members, if we are lucky enough – and I deeply hope we all are – they know an awful lot too.
 Joanne Huff comes to Courageous Parents Network as a long time follower and parent enthusiast of the organization. As the Mother of two girls, the oldest of whom has the rare disease MPS IIIA/Sanfilippo Syndrome, Joanne has benefited tremendously from the intimate parent interviews and candid, vulnerable story sharing throughout numerous thought provoking blog posts. As her daughter’s activities and lifestyle started to slow down with disease progression, CPN became a larger anchor in times of uncertainty and unrest. It is through this lens that Joanne hopes to share experiences and insights via the CPN blog.
Joanne Huff comes to Courageous Parents Network as a long time follower and parent enthusiast of the organization. As the Mother of two girls, the oldest of whom has the rare disease MPS IIIA/Sanfilippo Syndrome, Joanne has benefited tremendously from the intimate parent interviews and candid, vulnerable story sharing throughout numerous thought provoking blog posts. As her daughter’s activities and lifestyle started to slow down with disease progression, CPN became a larger anchor in times of uncertainty and unrest. It is through this lens that Joanne hopes to share experiences and insights via the CPN blog.
Joanne completed nursing school after her daughter’s diagnosis, receiving her Bachelors of Science in Nursing from Plymouth State University, Plymouth NH. She enjoyed community liaison work with home care providers of adults with special needs up until her own daughter’s care became increasingly more involved. In addition to serving on the Boards of New England Regional Genetics Group (NERGG) and Adaptive Sports Partners through 2024, she has found great purpose in volunteer work advocating for policy improvements and change in Washington DC with the National MPS Society. In her free time, Joanne seeks balance and refuge with yoga, hiking and performing as an ensemble Soprano vocalist with the Pemigewasset Choral Society. When not blogging for CPN, Joanne enjoys sharing offerings on her personal Blog Folding Origami for God. She resides in Bow New Hampshire with her two daughters, Sasha and Nika, her husband Mike and her yellow lab Suki.
It’s sometimes hard to discern when a cascade has its onset. When a fleeting thought tying a current situation to a similar one suddenly opens a vast abyss and down the rabbit hole we go. Recently, as I turned my daughter Sasha in bed preparing for the shower that awaited, I was transported back 18 years to a resident’s room in the long-term care facility where I worked as a nursing assistant. My mind recounted the position of the patient’s bed, their off white johnny with pale blue and green abstract designs, its material slightly scratchy from frequent laundering and the question I was asked during every bedding change – “When am I going home?”
A cascade of memories followed – the quirky personalities of my coworkers, the late night, harried winter commutes, the excitement felt when a resident would eat a truly good quantity of their dinner.
 And suddenly and for seemingly random reasons unclear, this catapulted me into reflections on all the specialists who follow Sasha. My head hummed with questions – was the newly developing guidance from our neurologist to decrease a medication overly ambitious? Should I make more time for the range of motion exercises recommended by an occupational therapist over two years ago? Was the quantity of g-tube formula shipped really going to carry us the entire month…do the prescribed 5 ¼ cartons per day really average out to 4.8 over the course of 30 days? Where are my math skills when I need them! Will her new wheelchair fit through her bedroom door? How funny would that be, after some 15 years with the old one, if we can’t use the new wheelchair in our new home(NOT)! Should I finally give up on the topical ointment we’ve employed for 10 months to treat her rosacea and move on to long term antibiotics? Should Sasha’s little sister Nika really be hanging out in a ski lodge each week, crammed indoors with the risk of flu so high?
And suddenly and for seemingly random reasons unclear, this catapulted me into reflections on all the specialists who follow Sasha. My head hummed with questions – was the newly developing guidance from our neurologist to decrease a medication overly ambitious? Should I make more time for the range of motion exercises recommended by an occupational therapist over two years ago? Was the quantity of g-tube formula shipped really going to carry us the entire month…do the prescribed 5 ¼ cartons per day really average out to 4.8 over the course of 30 days? Where are my math skills when I need them! Will her new wheelchair fit through her bedroom door? How funny would that be, after some 15 years with the old one, if we can’t use the new wheelchair in our new home(NOT)! Should I finally give up on the topical ointment we’ve employed for 10 months to treat her rosacea and move on to long term antibiotics? Should Sasha’s little sister Nika really be hanging out in a ski lodge each week, crammed indoors with the risk of flu so high?
I could feel the angst rising inside me as the cascade built.
As all these thoughts rattled through my head, it occurred to me that I have become the specialist’s extension – the vehicle through which so many tasks are performed. I embody the occupational therapist as I conduct range of motion exercises or the speech pathologist as I watch for swallowing patterns and listen for worrisome sounds. I roleplay a DME representative as I measure the bedroom doorway one last obsessive time. I imitate a case manager keeping tight oversight on Sasha’s needed medical supplies while juggling insurance approvals and prior authorizations like a seasoned healthcare agent. The registered nurse in me, while no longer in practice, closely monitors medication administrations, nutrition and hydration needs via Sasha’s g-tube.
As the cascade came to an apex, I wondered amidst the myriad roles, when do I become Sasha’s Mom again?
With that question at the forefront of my thoughts, I rolled Sasha over to remove her soiled diaper. As I did, I told her that this holiday season, we would sit on the couch together and watch Christmas movies. Not with her across the room from me in her sit to stand recliner while I’m on the couch (which in fairness affords a quick exit to tend to her four-year-old sister) but side by side, shoulder to shoulder, holding hands. I envisioned us, feet elevated on a shared pouf, cuddling with the same blanket on our laps. The image of our Christmas movie watching warmed me and instantly calmed the pending mental overload.
Complex medical parenting requires so many balls to levitate in the air simultaneously EACH and EVERY day. When our child is in maintenance mode (i.e. a steady baseline) the balls tend to be predictable – refills of medications, routine appointments, supply oversight, dietary planning and staffing coverage. It’s when things start to “go sideways” as my husband likes to call it, that life gets particularly challenging and loud. In an instant, we can be asked to maintain pre-existing roles while adding on foreign ones; the insurmountable cost of a wheelchair van as mobility starts slipping away; referrals for new specialists when mystery symptoms appear; consultations and surgical g-tube placement when swallowing capabilities decline; hospital admissions in the unfortunate event of a hard-hitting illness. It is during these times when our role as parent can feel as if it has completely receded – when the hopes of the simple act of watching holiday movies on the couch with my daughter seems elusive.
I often chuckle at New Year’s resolutions despite generating at least one or two each year. Those resolutions used to be quantitative in nature with satisfying measurable goals. But in recent years, they have become less constructed, softer and more idyllic in nature. I simply seek enhanced engagement and moments of true meaning with Sasha; not just making sure her medication refills are aligned or that she has enough incontinence supplies to stretch us to our next order, but qualitative pillars of joy and peace.
This holiday season, I watched exactly one Christmas movie sitting side by side with Sasha, our feet rested upon the new pouf my brother had gifted her. Shoulder to shoulder, I provided foolish Mom commentary at the hard to fathom scenes while wrapped in our shared blanket, holding hands. While I realize that some of the recommendations for making a successful resolution found in the SMART acronym (Specific, Measurable, Achievable, Relevant and Time Bound) were left out of my holiday pledge to Sasha, I got one of those five recommendations right. Relevance. Remembering that you are a parent first, creating moments of meaning, carving out experiences for connection, not just conducting the actions that keep our children physically functioning and safe, are paramount. I’ll take that sole movie viewing and moment of returning to Sasha’s Mother as a win.
 Joanne Huff comes to Courageous Parents Network as a long time follower and parent enthusiast of the organization. As the Mother of two girls, the oldest of whom has the rare disease MPS IIIA/Sanfilippo Syndrome, Joanne has benefited tremendously from the intimate parent interviews and candid, vulnerable story sharing throughout numerous thought provoking blog posts. As her daughter’s activities and lifestyle started to slow down with disease progression, CPN became a larger anchor in times of uncertainty and unrest. It is through this lens that Joanne hopes to share experiences and insights via the CPN blog.
Joanne Huff comes to Courageous Parents Network as a long time follower and parent enthusiast of the organization. As the Mother of two girls, the oldest of whom has the rare disease MPS IIIA/Sanfilippo Syndrome, Joanne has benefited tremendously from the intimate parent interviews and candid, vulnerable story sharing throughout numerous thought provoking blog posts. As her daughter’s activities and lifestyle started to slow down with disease progression, CPN became a larger anchor in times of uncertainty and unrest. It is through this lens that Joanne hopes to share experiences and insights via the CPN blog.
Joanne completed nursing school after her daughter’s diagnosis, receiving her Bachelors of Science in Nursing from Plymouth State University, Plymouth NH. She enjoyed community liaison work with home care providers of adults with special needs up until her own daughter’s care became increasingly more involved. In addition to serving on the Boards of New England Regional Genetics Group (NERGG) and Adaptive Sports Partners through 2024, she has found great purpose in volunteer work advocating for policy improvements and change in Washington DC with the National MPS Society. In her free time, Joanne seeks balance and refuge with yoga, hiking and performing as an ensemble Soprano vocalist with the Pemigewasset Choral Society. When not blogging for CPN, Joanne enjoys sharing offerings on her personal Blog Folding Origami for God. She resides in Bow New Hampshire with her two daughters, Sasha and Nika, her husband Mike and her yellow lab Suki.
Data suggest that 19% of the parenting population is caring for a medically complex child. While small, the number has me considering our common conundrums. For example, we often grapple with finding a comfortable baseline only to chronically wait for it to change. We have an acute awareness of the need to recognize better days for our child and family. And when a downward trend presents, hopes of returning to better days are clung to. A statement shared by triathlete Bruce Campbell, a fellow rare disease advocate diagnosed with Pompe Syndrome summarizes this well, “There’s a constant tension that comes with living with a body that doesn’t always cooperate with your spirit.” As a caregiver, a feeling of helplessness compounds constant tension. It also heightens my grief. I want my daughter to physically be able to do the things she used to. Not only because I miss those experiences with her, but because that loss of ability signifies that we’re getting closer to the finish line.
As the regression that is expected from a neurologically degenerative syndrome takes deeper hold in my daughter’s body and in our home, I recognize a phenomenon unfolding like nesting. Often seen in expecting mothers as the weeks of maternity wane, an urge to clean, organize and “nest” settles into the household. Alongside Sasha’s physical body starting to recoil into fetal posturing, her mouth forming sucking gestures when attempting to drink from a straw, and her ability to fall asleep amidst bustling public places, my muscle memory casts me back to her infant years. Pushing a bundled adult Sasha in a wheelchair mirrors infant Sasha going for walks in her stroller decades past. Recently, I am content to find myself painting rooms, rearranging décor, menu planning and keeping up with laundry, reminiscent of preparations for the arrival of a brand-new baby girl. Back when Sasha was born, it was a month before I ventured out into the world. Today, a big outing is a shopping run to gather provisions, then a swift return to the nest where I feel most at ease. A lifestyle such as this is a highly unusual state to find myself content in again. An era of flourishing for me is typically one filled with change, new experiences, new residences, new professional endeavors and frequent travel.
 Acceptance of any significant life shift that is not initiated by choice seldom comes easily. Early on clinical trials and research studies into supplements distracted me from acceptance of the realities of Sasha’s diagnosis. Then durable medical equipment to prolong safe eating and standing provided the next ray of hope. Manageable tasks like physical therapy alongside sweeping gestures such as the consideration of relocating to a warmer climate to meet Sasha’s evolving baseline helped me cling to the hope of a return to better days. I didn’t recognize that these actions were, in part, attempts to deny a reality until a dear fellow rare disease mom finally called it out, “Joanne! YOU CAN’T FIX THIS!” I was stunned but not hurt. Those were words I needed to hear. She was so right. I could not fix this. But I wondered, “How could that possibly be?”
Acceptance of any significant life shift that is not initiated by choice seldom comes easily. Early on clinical trials and research studies into supplements distracted me from acceptance of the realities of Sasha’s diagnosis. Then durable medical equipment to prolong safe eating and standing provided the next ray of hope. Manageable tasks like physical therapy alongside sweeping gestures such as the consideration of relocating to a warmer climate to meet Sasha’s evolving baseline helped me cling to the hope of a return to better days. I didn’t recognize that these actions were, in part, attempts to deny a reality until a dear fellow rare disease mom finally called it out, “Joanne! YOU CAN’T FIX THIS!” I was stunned but not hurt. Those were words I needed to hear. She was so right. I could not fix this. But I wondered, “How could that possibly be?”
Adjustment and adaptation are said to be nuanced responses to any life event that brings forth significant change. Adjustment is a more concrete approach incorporating actions employed to heighten functionality within a new landscape. A new equilibrium is the defined endpoint of adjustment. Adaptation on the other hand, is said to be a more psychological and emotional phenomenon. Here is where capabilities, circumstances and needs are assessed and reframed. Bruce Campbell’s words continue to resurface, “There’s a constant tension that comes with living with a body that doesn’t always cooperate with your spirit.” I live within a state of constant tension. Some of these tensions feel incredibly superficial – like not being able to have a pretty area rug in the living room due to wheelchair maneuverability. Other tensions run deeper and are much darker – like wondering if this could be Sasha’s last Christmas.
When Sasha was approaching sixteen, her neurologist sat me down to delicately segue the discussion to my quality of life alongside Sasha’s. He asked if I considered the longevity of Sasha’s care as she approached chronological adulthood. At the time, there was no apparent decline to Sasha’s physical presentation on the horizon, and he felt we had a long road ahead. He thought that residential care might be something worth considering. I was taken aback. I would never sleep a restful night knowing that Sasha was in a bed outside of our shared home. It is only now that I realize he was hoping to get me to simply make adjustments. Many years later, I now recognize why research is delving into a phenomenon identified so often by study participants: the continual attempts to reconstruct lives to accommodate an illness. The emotional component of a decision like considering residential placement for Sasha is something nearly impossible to convey and I am not sure if any amount of adjustment or adaptation would ease the tension. Because in truth, something even larger looms. Acceptance it turns out, has been my true Achilles.
Acceptance is defined as the action of consenting to receive or undertake something offered. In medically complex parenting scenarios, an additional parenting responsibility has been bequeathed. It’s as though a medical, emotional, physical and spiritual reality has been bestowed upon us and there is no longer, or maybe never was, contact with the originator who passed it down to us. I have long accepted that I will likely never find a satisfactory answer to the “why” question. Why should an innocent child suffer and endure symptoms that combine ALS and Alzheimer’s all in one? How frightening must it be for Sasha to be so impacted by developmental delays that she cannot express her experiences and hardships? Why was I entrusted to walk this path and care for someone that special? Am I honoring Sasha’s spirit as I care for a body that doesn’t always cooperate with it? When I look back on conversations with hundreds of rare disease families over the past 20 years, I often recognize that acceptance is hard to find. I will forever miss walking with Sasha through the halls of her vast medical center to admire the colorful mobiles in the sweeping halls. I will always be aware that my body is pushing her in a wheelchair as opposed to walking shoulder to shoulder, hand in hand. With each delivery of g-tube formula and feeding bags, I will always mourn shopping for her favorite foods – avocados, bananas, sweet potatoes. Just yesterday I put the blender away for good. Stored it in a forgotten cupboard with no plans to ever see it again. How does one accept any of this?
“There’s a constant tension that comes with living with a body that doesn’t always cooperate with your spirit.” We can adjust, adapt, reframe and retool. But to accept should perhaps never be an expectation, only something to strive for. As I continue to nest, I suspect there will be more to explore.
Citation:
https://psychology.town/psychosocial-issues-in-disability/stages-adaptation-adjustment-disability/
https://pmc.ncbi.nlm.nih.gov/articles/PMC11506064/
 Joanne Huff comes to Courageous Parents Network as a long time follower and parent enthusiast of the organization. As the Mother of two girls, the oldest of whom has the rare disease MPS IIIA/Sanfilippo Syndrome, Joanne has benefited tremendously from the intimate parent interviews and candid, vulnerable story sharing throughout numerous thought provoking blog posts. As her daughter’s activities and lifestyle started to slow down with disease progression, CPN became a larger anchor in times of uncertainty and unrest. It is through this lens that Joanne hopes to share experiences and insights via the CPN blog.
Joanne Huff comes to Courageous Parents Network as a long time follower and parent enthusiast of the organization. As the Mother of two girls, the oldest of whom has the rare disease MPS IIIA/Sanfilippo Syndrome, Joanne has benefited tremendously from the intimate parent interviews and candid, vulnerable story sharing throughout numerous thought provoking blog posts. As her daughter’s activities and lifestyle started to slow down with disease progression, CPN became a larger anchor in times of uncertainty and unrest. It is through this lens that Joanne hopes to share experiences and insights via the CPN blog.
Joanne completed nursing school after her daughter’s diagnosis, receiving her Bachelors of Science in Nursing from Plymouth State University, Plymouth NH. She enjoyed community liaison work with home care providers of adults with special needs up until her own daughter’s care became increasingly more involved. In addition to serving on the Boards of New England Regional Genetics Group (NERGG) and Adaptive Sports Partners through 2024, she has found great purpose in volunteer work advocating for policy improvements and change in Washington DC with the National MPS Society. In her free time, Joanne seeks balance and refuge with yoga, hiking and performing as an ensemble Soprano vocalist with the Pemigewasset Choral Society. When not blogging for CPN, Joanne enjoys sharing offerings on her personal Blog Folding Origami for God. She resides in Bow New Hampshire with her two daughters, Sasha and Nika, her husband Mike and her yellow lab Suki.
“I’m so glad I have a sister. Otherwise, it would just be me, you, Daddy and Suki (our dog).” Those were the words spoken to me recently by my four-year-old daughter, Nika as I rounded the corner from Sasha’s sit to stand recliner and headed towards the hall. I was stunned but tried not to show it. It had been a hard week in the household. I returned from a remarkable caregiver’s workshop in Washington DC to find that Sasha took a swift downturn during my ever so brief absence. We had already taken her to her primary care provider. It was a lengthy visit. As I sat there, the most surreal wave washed over me – a knowledge crest that everything was about to change.
My husband Mike came to the appointment to help get Sasha in and out of our vehicle. We had Nika in tow as the appointment fell on a non-school day. Fortunately, there is a cute park on the clinic’s campus, and the weather cooperated for Nika to play for nearly 2 hours while Sasha and I investigated the next steps in her care plan. I appreciated the levity of Mike sending me time trials as Nika ran laps, “11.77, 12.08, 11.76, 13.31.” Random figures illuminated my phone with no explanation – a pleasant mystery that provided a helpful distraction. The day was a brighter gray than some during a particularly windy October.
appointment fell on a non-school day. Fortunately, there is a cute park on the clinic’s campus, and the weather cooperated for Nika to play for nearly 2 hours while Sasha and I investigated the next steps in her care plan. I appreciated the levity of Mike sending me time trials as Nika ran laps, “11.77, 12.08, 11.76, 13.31.” Random figures illuminated my phone with no explanation – a pleasant mystery that provided a helpful distraction. The day was a brighter gray than some during a particularly windy October.
Daylight savings was coming soon. I sat there silently bemoaning as I waited for Sasha’s PCP to enter the exam room. I’ve always resented the changing of clocks. In my college years, my first taste of adulthood, the time change always took me aback as it collided with an irresponsible modus operandi. Seemingly always in a public establishment, I’d look up only to realize I was an hour off on my given day. Years later, upon having my first child—a daughter with special needs—I would marvel, with frustration, at how deeply her days were affected by adding or taking away even one hour from her already tenuous schedule. Now, in middle age, I resent the changing of clocks for an entirely different reason: who are we to collectively manipulate time? What gives us the societal audacity to control clocks? Do we think we are God? Little did I know—especially in those college years—that time would become such a burden during most of my child-rearing years. I would either wish for it to speed up amid the angst of “When will this ever end?” or to slow down indefinitely so I could cherish the good years.
For nearly two decades, that balancing act came alongside a family unit of 2-3 individuals. While a single Mom to Sasha, there was never a reality of adding a sibling to her chaos. And when I met my second husband as Sasha was approaching age five, I was still a steadfast NO! My hands felt full with an extremely hyperactive child with significant special needs. Being in the throes of destructive sleepless nights, a nocturnal manic state that is common for children with Sanfilippo Syndrome, I knew that adding another child would be the rush of air that pushed down the line of dominos. As Sasha approached nine and we learned of her diagnosis of Sanfilippo Syndrome, we were faced with an unthinkable reality – Sasha’s body carried something fatal. With that realization came the heavy understanding that adding another child would mean they, too, might one day experience a traumatic loss. I doubled down on my steadfast “no” but was that ever the right way to view things? In truth, we could all lose anyone in an instant. Who was I to play God…to try and control any outcome?
My phone continued flashing Nica’s times as I chatted with our PCP’s counterpart, a new nurse practitioner on Sasha’s medical team who was visibly committed to addressing the clinical concerns unfolding. We discussed the preceding week and the cascade of events – Sasha’s sudden struggles with swallowing, her significant weight loss and increased tremors while eating. A swallow study was ordered. I left with numerous instructions, including recommendations for utilizing Sasha’s g-tube for nutrition within a specified framework.
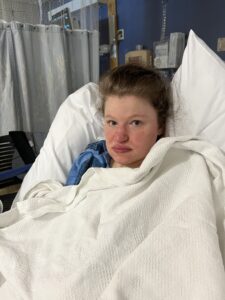 The g-tube. A gut-wrenching decision that I fought so hard against that preceding year. Nine months of meeting with numerous specialties – Palliative, Genetics, Neurology, Complex Care. Messaging friends and acquaintances in the Sanfilippo community. Reaching out to fellow nurse friends to discuss the clinical implications. Listening to interviews of families before me who navigated the same decision. Middle-of-the-night brainstorming sessions filled with self-reflective thoughts. Looking back on the early days post diagnosis. I remembered sitting in Sasha’s cozy bed, holding her close, telling her I would never initiate any invasive procedure. We would let nature guide us and she could tell me when she was ready to be done with the fight. I told her to never hold on for me or anyone else. When she was tired, she could let us know and we would support her decision to let go. I would never play God.
The g-tube. A gut-wrenching decision that I fought so hard against that preceding year. Nine months of meeting with numerous specialties – Palliative, Genetics, Neurology, Complex Care. Messaging friends and acquaintances in the Sanfilippo community. Reaching out to fellow nurse friends to discuss the clinical implications. Listening to interviews of families before me who navigated the same decision. Middle-of-the-night brainstorming sessions filled with self-reflective thoughts. Looking back on the early days post diagnosis. I remembered sitting in Sasha’s cozy bed, holding her close, telling her I would never initiate any invasive procedure. We would let nature guide us and she could tell me when she was ready to be done with the fight. I told her to never hold on for me or anyone else. When she was tired, she could let us know and we would support her decision to let go. I would never play God.
That time now felt so out of reach, so long ago, like she and I were completely different people. I couldn’t believe the day I found myself sitting in a surgeon’s clinic, waiting for a g-tube consultation. He thought Sasha and I were there to schedule the surgery. In reality, I was there to ask the question, “who are we to think we can change course in an agreed upon pact?”
A highly rushed individual, as trauma surgeons will be, he bound through the exam room door and asked even before making eye contact or sitting down, “What questions do you have for me?” I stared as I waited for him to find his seat and scoot over via his three-wheeled black vinyl stool. A lanky fellow with wisps of black hair along a mostly bald scalp, his shoulders too broad for the wash-faded indigo scrubs, I quietly wondered if he was a long-distance runner. He looked at Sasha and saw my reservations. Knowing we were both rushing to get out of there, I spoke rapidly to squeeze it all in. Eventually, he softened and shared a personal story of his own father temporarily needing a g-tube. He could not impress upon me enough, he stated, the importance of nutrition and hydration in all phases of the lifespan. In that moment, he became more than a surgeon. He became human.
I told him I’d think it over and he shared the process for scheduling. It would not be an immediate phone call, I told him. He encouraged me to call and make an appointment, pointing out that as the day approached, I could always cancel if I was still feeling unsure. He left. I felt a bolstering confidence, ever so briefly. I was not reneging on an agreement made to Sasha so many years ago. And I certainly was not playing God. Was I?
“12.65” Nika’s time trials at the clinic’s park were ending alongside our appointment. Mercifully, Nika did not ask what transpired, an unusual occurrence for her inquisitive nature and foreman mindset overseeing all of Sasha’s care needs. She was consumed in exhilaration by her newfound mastery of time. She had learned through her dad’s coaching that she was slowing down ever so slightly each time she approached the finish line. He had explained that if she made a final push as the imaginary line approached, her time would improve.
There will be times in virtually all our lives, where we will be asked to make a decision standing at the crossroads of faith and uncertainty – at the intersection of medicine and personal philosophy. We may be called to decide for ourselves or for a loved one in a way that directly impacts a clinical outcome.
I have been fortunate to have a care team that welcomes these discussions, even discourse when necessary and who recognizes that philosophy is sometimes malleable and that certainty is never a guarantee. In a world that feels unquantifiable, when making decisions that feel impossible, I came to realize that an 80/20 ratio may be the best that I can do. If 80% confidence in a decision can be obtained, then that is where I will hang my hat. Those decisions may evolve with the revelation of new information or the presentation that is in front of you – our minds can change, and that is alright.
I didn’t know what to say in response that day when Nika proclaimed how happy she was to have a sister. I fought back tears and simply offered, “I’m so glad you have a sister too.”
 Joanne Huff comes to Courageous Parents Network as a long time follower and parent enthusiast of the organization. As the Mother of two girls, the oldest of whom has the rare disease MPS IIIA/Sanfilippo Syndrome, Joanne has benefited tremendously from the intimate parent interviews and candid, vulnerable story sharing throughout numerous thought provoking blog posts. As her daughter’s activities and lifestyle started to slow down with disease progression, CPN became a larger anchor in times of uncertainty and unrest. It is through this lens that Joanne hopes to share experiences and insights via the CPN blog.
Joanne Huff comes to Courageous Parents Network as a long time follower and parent enthusiast of the organization. As the Mother of two girls, the oldest of whom has the rare disease MPS IIIA/Sanfilippo Syndrome, Joanne has benefited tremendously from the intimate parent interviews and candid, vulnerable story sharing throughout numerous thought provoking blog posts. As her daughter’s activities and lifestyle started to slow down with disease progression, CPN became a larger anchor in times of uncertainty and unrest. It is through this lens that Joanne hopes to share experiences and insights via the CPN blog.
Joanne completed nursing school after her daughter’s diagnosis, receiving her Bachelors of Science in Nursing from Plymouth State University, Plymouth NH. She enjoyed community liaison work with home care providers of adults with special needs up until her own daughter’s care became increasingly more involved. In addition to serving on the Boards of New England Regional Genetics Group (NERGG) and Adaptive Sports Partners through 2024, she has found great purpose in volunteer work advocating for policy improvements and change in Washington DC with the National MPS Society. In her free time, Joanne seeks balance and refuge with yoga, hiking and performing as an ensemble Soprano vocalist with the Pemigewasset Choral Society. When not blogging for CPN, Joanne enjoys sharing offerings on her personal Blog Folding Origami for God. She resides in Bow New Hampshire with her two daughters, Sasha and Nika, her husband Mike and her yellow lab Suki.
It had been many years, 23 to be exact, since the last time I navigated life with a toddler. While friends of mine have started celebrating their entrance into grandparenthood, I had a remarkable occurrence of a surprise pregnancy instead. At age 45, while already the mother to a 22-year-old daughter with medical complexity and developmental needs, I was told the shocking news that I would be the parent to a daughter once again. Advanced maternal age hurdles were cleared, some more tenuous than others, but lo and behold, in the winter of 2021, a newborn arrived. Those first two years with our daughter Nika were filled with daily pinch me moments. We marveled at the mere existence of this new person developing before us. Highchairs, car seats, onesies and child rearing technological offerings, unheard of in the late 1990s, all took hold within our home. Milestones were easily met. We were on absolute cloud nine.
Then, toddlerhood entered. The temper tantrums, safety concerns and juggling of a very mobile little one coupled with the noticeable decline of her older sister became a heavier weight to carry. In this newest journey with toddlerhood, I started to wonder if my age (now 50) or perhaps the cumulative effects of decades of diaper changes, now for two individuals instead of just one, had created mental exhaustion.
I started to rescind from social interactions due to overwhelm. Most notable was my inability to clearly answer the question; how can I help? when offered by supportive friends. I understood their generosity and genuine desire to be of assistance, but I could not identify my own needs. My internal dialogue went something like this – Do I need someone to tend to the house or tend to my older daughter with special needs? Would it help my mental state if I found purpose by going back to work? Should my toddler attend preschool full-time while I remain home to catch my breath? Maybe I could simply “do better” at streamlining life and its collective tasks. In this past year, the most common thought I find myself thinking in response to outside offers of help is, “stop making my life harder”.
Small minor things like my husband asking if I know where his shoes are, my toddler insisting on Mommy doing something over anyone else, administrative bottle necks when trying to get a mere prescription refilled, are all examples of times when mental overwhelm takes hold. This wasn’t always the case. It’s only during this past year I’ve noticed this shift within my normal state of homeostasis.
This phenomenon self-propelled; it is now the case that when well-meaning friends suggest the planning of a girls’ outing, when I place unrealistic expectations on myself to see extended family members, or even just grabbing a quick dinner out with my husband ALL compound daily stressors. Each time one of these opportunities arises, I feel the quiet constraint of a belt being cinched, hoping to reach that next hole – wanting to please others, wanting to find balance, wanting to lead a normal adult life. Meanwhile, I feel a house of cards crashing down from all the tasks waiting in the wings.
Recently, I decided to investigate what research exists on the tolls taxed upon caregivers of adult children with special needs. I postulate that these consecutive 27 years, totaling more than half of my own lifespan, are the root cause of my mental decline. It’s not so much that the individual tasks of caring for Sasha, who suffers from the neurologically degenerative Sanfilippo Syndrome, are my undoing, but rather the collective and ongoing nature of those tasks.
needs. I postulate that these consecutive 27 years, totaling more than half of my own lifespan, are the root cause of my mental decline. It’s not so much that the individual tasks of caring for Sasha, who suffers from the neurologically degenerative Sanfilippo Syndrome, are my undoing, but rather the collective and ongoing nature of those tasks.
Indeed, a useful study conducted by the Polibienestar Research Institute, Universitat de Valencia and Biomedical Data Science Lab – ITACA Institute, Universitat Politecnica de Valencia, found that “the aging of family caregivers has been correlated with decreasing caregiving efficiency”. Perhaps my initial read was accurate. While my commitment to caregiving itself has never waned, my engagement with all things peripheral from it certainly has.
A little more digging had me also reading a National Institute of Health study illuminating Carol Ryff’s 6 domains for consideration towards psychological wellbeing: (1) Self-Acceptance, (2) Positive Relations with Others, (3) Autonomy, (4) Environmental Mastery, (5) Purpose in Life, and (6) Personal Growth. Immediately, many of these categories lit up my brain like a PET scan and caused me to reflect on the evolution of my life.
Sasha, who for so many years ran wild, laughed with mischief, fed herself and loved riding in the car, windows open, music blaring, is now so deeply changed. Today, Sasha is wheelchair bound, trembling while eating, crying out in the night longing for assistance to be repositioned. She needs diapering at the most inconvenient times, which is every instance that we’re headed out our front door on time, or in a public setting with a precarious wheelchair bathroom. As her eating and drinking rates have significantly slowed and require more of my time, the list of administrative and household to-do’s sits idly waiting. Her care has taxed my autonomy, my environmental mastery, my self-acceptance and my purpose in life. She has changed my trajectory. This reality is undeniable.
Sasha’s changes serve as a reminder that what was once helpful to me – like offers from others to help – may no longer be as useful. I live in a suspended state knowing that what would be most useful to me now is something that will never return: a mobile Sasha – a robust, strong, speed eating, agile Sasha. Setting that aside, even when I can identify resources to bolster control over my new environmental landscape – those which might provide greater autonomy or tap into my purpose and aid with self-acceptance – I find myself unable to act. My continual state of overwhelm has made it difficult to determine a beneficial resource.
At one point in time finding someone to help with housework or securing a care provider with a flexible schedule were the most meaningful forms of assistance. Blogging and journaling aided in reflection and self-acceptance and rippled into enhanced positive relations with others. Working outside the home provided purpose in life and personal growth. But in this current iteration of life, those tasks simply mean more oversight, which means more areas for me to manage.
In recent years, I have also identified that a quiet house provides the biggest boost in bandwidth. When Sasha’s school years came to an end, so did a quiet home. While we are very fortunate to have nursing staff come into the home to care for Sasha, Sasha and her sister (along with an additional individual) are now almost always home and a quiet house nowhere to be seen. This suggests to me that a certain bandwidth must be present to even pursue supportive tools or resources.
How can I help? is a well-meaning inquiry. But this inquiry can often stunt a response from the caregiver who is so often in that state of overwhelm. It asks us to think of a solution when we are already drowning. Thinking about Carol Ryftt’s 6 domains, it occurred to me that those offering support should consider them as well. For example, when asking a friend who is caring for an individual with special needs to go on a girl’s weekend, it might be helpful to first ask yourself – does that friend HAVE the mastery over their environment, or the autonomy to make such a plan? Or upon deeper reflection, you might see that the caregiver is consumed with domains 5 and 6 and understand that simply going out to dinner may feel like a pulling away from precious time needed to pursue their own self-care or purpose creating activities.
Caregivers often struggle with how their lives feel dictated by their circumstances. In my case, travel, working outside of the home and the pursuit of additional higher education, all intrinsically meaningful to me, also have all been put on an indefinite hold. I greatly miss engaging in a community aligned with my outside interests and meeting a greater sense of purpose. Self-acceptance ebbs and flows most days, which naturally impacts the final domain, positive relations with others. If an individual does not feel like they are flourishing, a rippling effect into other relationships can be expected.
All this is to say, caregivers feel tremendous strain. There are many days when the provision of basic life necessities are the only realistic activities to complete. I would like to offer this suggestion to those wanting to support parents like me. Offer a tangible, finite gesture of assistance. Rather than making a broad offer – Can I bring you dinner? Clarify it – “I can bring dinner over either on Tuesday, Thursday or Sunday this week” or “I can take the girls for a Sunday drive this month so that you can quietly tackle things around the house”. These more directive offers remove the pressure felt by the caregiver to make yet another decision.
Supporting a friend or family member like me is truly a subjective task for both parties involved, the supporter and the supported. It’s important to know that the caregiver role is an ever-changing landscape. Supporting loved ones navigating this life requires some reflection and finesse by both parties. In the end, and I say this delicately, trying not to “make that person’s life harder” may be a helpful mantra to start with when you are considering how to support caregivers.
References:
Namkung, E. H., Greenberg, J. S., Mailick, M. R., & Floyd, F. J. (2018). Lifelong parenting of adults with developmental disabilities: Growth trends over 20 years in midlife and later life. American Journal on Intellectual and Developmental Disabilities, 123(3), 228–240. https://doi.org/10.1352/1944-7558-123.3.228
https://www.sciencedirect.com/science/article/abs/pii/S0277953624011031
 Joanne Huff comes to Courageous Parents Network as a long time follower and parent enthusiast of the organization. As the Mother of two girls, the oldest of whom has the rare disease MPS IIIA/Sanfilippo Syndrome, Joanne has benefited tremendously from the intimate parent interviews and candid, vulnerable story sharing throughout numerous thought provoking blog posts. As her daughter’s activities and lifestyle started to slow down with disease progression, CPN became a larger anchor in times of uncertainty and unrest. It is through this lens that Joanne hopes to share experiences and insights via the CPN blog.
Joanne Huff comes to Courageous Parents Network as a long time follower and parent enthusiast of the organization. As the Mother of two girls, the oldest of whom has the rare disease MPS IIIA/Sanfilippo Syndrome, Joanne has benefited tremendously from the intimate parent interviews and candid, vulnerable story sharing throughout numerous thought provoking blog posts. As her daughter’s activities and lifestyle started to slow down with disease progression, CPN became a larger anchor in times of uncertainty and unrest. It is through this lens that Joanne hopes to share experiences and insights via the CPN blog.
Joanne completed nursing school after her daughter’s diagnosis, receiving her Bachelors of Science in Nursing from Plymouth State University, Plymouth NH. She enjoyed community liaison work with home care providers of adults with special needs up until her own daughter’s care became increasingly more involved. In addition to serving on the Boards of New England Regional Genetics Group (NERGG) and Adaptive Sports Partners through 2024, she has found great purpose in volunteer work advocating for policy improvements and change in Washington DC with the National MPS Society. In her free time, Joanne seeks balance and refuge with yoga, hiking and performing as an ensemble Soprano vocalist with the Pemigewasset Choral Society. When not blogging for CPN, Joanne enjoys sharing offerings on her personal Blog Folding Origami for God. She resides in Bow New Hampshire with her two daughters, Sasha and Nika, her husband Mike and her yellow lab Suki.
Six years ago, my daughter Sasha aged out of the public school system. I was forewarned by our area agency, her medical team and school staff that this transition would not be easy. Yet as much as they prepared me for the challenges that lay ahead, I was still taken aback by the freefall that occurred immediately after “age-out” day.
On Sasha’s last day of school, her therapists, aides, classmates and classroom staff hosted a big party. We laughed as we sat with paper plates on our laps, reminiscing about so many incredible elementary, middle and high school years. After an hour or so, Sasha’s physical therapist asked if they could walk the halls together one last time. I held back tears as we loaded our van with Sasha’s favorite school supplies – a dinosaur stenciled pillowcase, a plush musical octopus, special blankets and chewies, clothing and hair supplies.
In preparation for the coming years and after careful consideration, we decided on the Parent Directed Management System (PDMS) for Sasha’s day program. Unlike the Traditional Day Program where an area agency provides staff and locations, the PDMS model would give us the autonomy to utilize Sasha’s annual Medicaid and State budget in varying ways. We would be responsible for hiring and overseeing our own staff and building goals around a program we created. This model would have its benefits and challenges, but our desire for a customized day program that emulated what Sasha loved most about school drove the decision.
In the early months, we struggled to find staff in our rural community, a challenge we anticipated. Then, a pandemic hit. Life halted for most, and the medical vulnerabilities within the special needs community temporarily froze all programs. Next came a surprise pregnancy. I was 45 years old, making me now at increased risk for COVID too, in addition to an unborn child. All systems were necessarily on hold.
Somehow, six years passed. Six years of Sasha remaining at home. Little structure was present in her days other than meal and medication schedules and instilling purpose and meaning was like watching a balloon float just out of reach. And so, It was with disbelief during Sasha’s 2024 annual physical that the topic of summer camp arose. Her PCP, the Medical Director at a camp serving individuals with special needs in southern New Hampshire, broached the topic, “With Sasha doing so well,” she began “do you think she’d be interested in attending camp next summer?” Doing so well? I recall thinking. Attend camp? “With you living a good distance away” she continued, “overnight would make the most sense of course. We offer 5, 7 or 10-day sessions”. Overnight would make the most sense? I thought. I sat there…stunned. But I knew this was a must-do for Sasha. She had barely left my side for six whole years. She was 26 years old.
When registration opened, despite the commute, I changed my application status from overnight to day camp. I wasn’t sure If I was ready to displace Sasha, however temporary. I envisioned her looking up at the ceiling of a camp cabin, wondering if she would ever return home. I didn’t think either of us were ready for something so big. Soon thereafter, we attended the open house, touring the facilities and grounds. We met camp counselors from all over the world and got a wonderful feel for the activities and programs provided each day. On the car ride home Sasha’s sister Nika, age 4, asked why she couldn’t attend too.
The excitement in our home was palpable as the first day of camp approached. Checklists and shopping trips, preparations and medical clearances were all complete. The night before camp started, we retired a bit early and told Sasha what lay ahead. Tomorrow, she had a place to be.
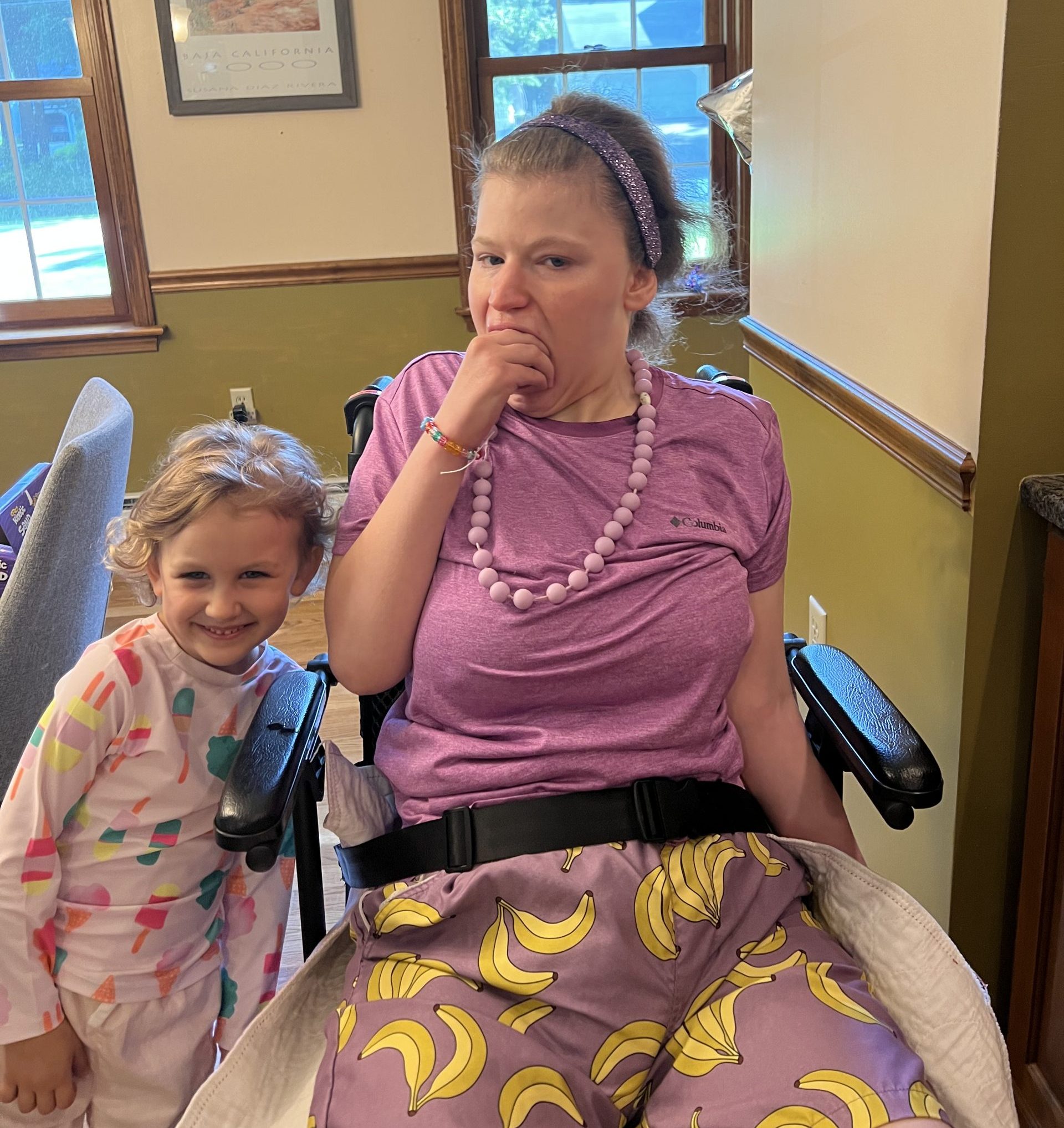 That first morning was surreal, reminiscent of routines from years ago when Sasha attended school. I felt a familiar pang as I prepared myself to allow someone else to care for Sasha. Her sister was stoic, asking if she could make Sasha’s lunch and silently loaded her bag. I tried not to let my mind wander. A haunting notion that a much deeper loss awaited us all one day kept rising. One day we will be packing hospital bags instead of lunches. One day Sasha will leave the house and not return home. But there was no time to dwell. Drop off time was near.
That first morning was surreal, reminiscent of routines from years ago when Sasha attended school. I felt a familiar pang as I prepared myself to allow someone else to care for Sasha. Her sister was stoic, asking if she could make Sasha’s lunch and silently loaded her bag. I tried not to let my mind wander. A haunting notion that a much deeper loss awaited us all one day kept rising. One day we will be packing hospital bags instead of lunches. One day Sasha will leave the house and not return home. But there was no time to dwell. Drop off time was near.
As we got out of the car there was one counselor left on the gravel road, waiting for their camper. I am self-aware enough to know that I spoke forever while introducing us all to Joyce. I shared Sasha’s likes and dislikes, which noises indicate discomfort and which noises express joy. I conveyed the importance of hydration and discussed her g-tube along with how to best feed her purees. Nika listened attentively but spoke little. As we drove down the dirt road leaving Sasha behind Nika cried out “I miss her already!” I understood. I did too.
For the next five days we learned and grew as we honed our routines. Nika would excitedly march ahead of me into Sasha’s room each morning, flip on the light and call out “Sashaaaaa…. it’s camp tiiiiime!”. Then she would meticulously discuss outfit options, all the way up to the headband. Lunch would get packed as I fed Sasha her breakfast and then Nika would hold the front screen door for me to help the wheelchair fit through the threshold. She was so proud that her sister had somewhere to be.
 During daily pick-up we’d marvel at the joy Sasha’s arts and crafts brought us. Painted rocks for Mom and Dad, sunrise paintings for Sasha’s room, namesake beaded jewelry for her sister. But more than all those things, camp gave us a must-do schedule with Sasha as opposed to an optional one. Sasha was given structure, autonomy, identity and purpose. It also gave us one more thing, equity.
During daily pick-up we’d marvel at the joy Sasha’s arts and crafts brought us. Painted rocks for Mom and Dad, sunrise paintings for Sasha’s room, namesake beaded jewelry for her sister. But more than all those things, camp gave us a must-do schedule with Sasha as opposed to an optional one. Sasha was given structure, autonomy, identity and purpose. It also gave us one more thing, equity.
That word kept ringing in my ears as the end of camp neared. While reflecting on the people, the tone, the joy and the humanity that surrounded Sasha during her time at camp, movie reels of life throughout the years played in my mind. The reels mostly included Mike, Nika and I running to and fro while Sasha often stayed behind. We went out in the world to socialize or get things done and then report back. Meanwhile, Sasha’s day was unchanged.
During camp week, however, things felt…. equitable. Fair and impartial. Sasha would go out in the world for a day of socializing and productivity while we did the same. Both parties would report back with experiences to tell one another. What a gift camp gave us all.
________________________________________________________________________________________________________________
Joanne Huff comes to Courageous Parents Network as a long time follower and parent enthusiast of the organization. As the Mother of two girls, the oldest of whom has the rare disease MPS IIIA/Sanfilippo Syndrome, Joanne has benefited tremendously from the intimate parent interviews and candid, vulnerable story sharing throughout numerous thought provoking blog posts. As her daughter’s activities and lifestyle started to slow down with disease progression, CPN became a larger anchor in times of uncertainty and unrest. It is through this lens that Joanne hopes to share experiences and insights via the CPN blog.
Joanne completed nursing school after her daughter’s diagnosis, receiving her Bachelors of Science in Nursing from Plymouth State University, Plymouth NH. She enjoyed community liaison work with home care providers of adults with special needs up until her own daughter’s care became increasingly more involved. In addition to serving on the Boards of New England Regional Genetics Group (NERGG) and Adaptive Sports Partners through 2024, she has found great purpose in volunteer work advocating for policy improvements and change in Washington DC with the National MPS Society. In her free time, Joanne seeks balance and refuge with yoga, hiking and performing as an ensemble Soprano vocalist with the Pemigewasset Choral Society. When not blogging for CPN, Joanne enjoys sharing offerings on her personal Blog Folding Origami for God. She resides in Bow New Hampshire with her two daughters, Sasha and Nika, her husband Mike and her yellow lab Suki.
Every two years in the month of July the deadline for redetermination of Medicaid coverage looms. My daughter, approaching age 27, has received subsidized health insurance for well over two decades. Her diagnosis, the rare genetic syndrome MPS IIIA (Sanfilippo Syndrome), requires extensive medical surveillance. We are fortunate that its severe impacts, surrounded by developmental delays, seizures and a degeneration of the central nervous system, are greatly but not entirely supported by Medicaid. The trifecta of her syndrome results in not only an all-hands-on-deck approach within the household but, if I’m being forthcoming, also a tremendous financial burden to both the family unit and the taxpayer at large.
 I have long recognized and spoken of the financial burden that my daughter Sasha imposes upon the healthcare system. What I don’t often speak of is the financial impact her condition has on our household. The reality of both parents maintaining employment presents a logistical nightmare, as care management of a medically complex child is a full time job. Authorizations to obtain services are complex, and coordinating referrals, reauthorizations and appointments are commonplace in day to day life making parents both caregiver and case manager.
I have long recognized and spoken of the financial burden that my daughter Sasha imposes upon the healthcare system. What I don’t often speak of is the financial impact her condition has on our household. The reality of both parents maintaining employment presents a logistical nightmare, as care management of a medically complex child is a full time job. Authorizations to obtain services are complex, and coordinating referrals, reauthorizations and appointments are commonplace in day to day life making parents both caregiver and case manager.
In Sasha’s early years, 1:1 supervision was required; she had the physical strength of a child her age but the cognitive awareness of an 18 month old. This made for numerous safety concerns and a need for her to always have eyes on her. Now in her older years the 1:1 supervision has been paramount for hygiene needs, feedings and positioning as she approaches a state nearing paralysis. Training in-home staff in a high turnover field eats up extended time periods and often parents need to fill the gaps in care, making a professional career nearly impossible. I know the continuous financial strain that Sasha’s care has placed on our family all these years, but I am also acutely aware that I am one of the lucky ones. There is sufficient financial stability in our home to provide for the option for me to not work full-time. But I worry – what are other, less fortunate families to do, especially in a political climate of intense governmental financial scrutiny, often by individuals far removed from the real life experiences of families like mine?
 We have also been fortunate with our healthcare system and medical team in the state of New Hampshire. In time we’ve found ourselves an incredible medical team of over 10 specialists that supports both Sasha’s physical health and her mental wellbeing. When we struggled to keep Sasha safe in bed at night due to frequent nocturnal seizures, her neurologist wrote a medical order for a “sleep safe bed”. At that same time, pharmaceuticals were slowly introduced until we found the right mix to halt a most harrowing seizure condition. When her mobility started to wane, multiple consults took place with equipment vendors, doctors and physical therapists to obtain a highly specialized gait trainer- a “walker” to keep her upright for bone health and moving safely through her world. A shower chair to support both her and our safety was introduced.
We have also been fortunate with our healthcare system and medical team in the state of New Hampshire. In time we’ve found ourselves an incredible medical team of over 10 specialists that supports both Sasha’s physical health and her mental wellbeing. When we struggled to keep Sasha safe in bed at night due to frequent nocturnal seizures, her neurologist wrote a medical order for a “sleep safe bed”. At that same time, pharmaceuticals were slowly introduced until we found the right mix to halt a most harrowing seizure condition. When her mobility started to wane, multiple consults took place with equipment vendors, doctors and physical therapists to obtain a highly specialized gait trainer- a “walker” to keep her upright for bone health and moving safely through her world. A shower chair to support both her and our safety was introduced.
Yet, these supports come with a price tag. Let me illustrate just a few. The out-of-pocket cost for the sleep safe bed would have been $10,000. The pharmaceuticals that have remarkably kept Sashsa’s seizures at bay for 12 years would cost $1800 per month without assistance from Medicaid. The out-of-pocket cost for the gait trainer to assist Sasha in safe ambulation would have been over $8,000 and the shower chair we rely on for safe sanitation charged our private insurance over $2,000. Thankfully, these items have all been covered either through our private insurance or Medicaid. While my family situation is secure, I can honestly tell you that bearing the responsibility for these costs without Medicaid, even with private insurance, would break any family including my own.
But this is where so many families like mine sit – in that divide of who benefits and how the financial burden is shared. It is an uncomfortable conversation. I fully see and understand the financial implications that we as society face as we address heaping debt. And yet medical ill fortune could fall on any one of us in an instant.
In nursing school, I had an opportunity to study internationally and perform clinical work with underserved and developmentally impaired communities. This time revealed the sobering truth of why robust medical teams, research and development and social services are so vital here in the United States. The support we have here in the US helps carry us in our day to day lives and it keeps my child living at home, where I want her to be, and where I know her care is less economically burdensome to society at large.
 I have long maintained that, to me, Sasha is truly one IN a million. The physical challenges coupled with the emotional toll of watching her vitality fade NEVER overshadows the joy she brings to my daily life. The lessons she has taught me about love and commitment and gratitude are forever at the forefront of my days. But one could also argue that Sasha is one OF a million. From a financial burden standpoint, if you multiply the above-mentioned costs, you would arrive at a staggering financial total.
I have long maintained that, to me, Sasha is truly one IN a million. The physical challenges coupled with the emotional toll of watching her vitality fade NEVER overshadows the joy she brings to my daily life. The lessons she has taught me about love and commitment and gratitude are forever at the forefront of my days. But one could also argue that Sasha is one OF a million. From a financial burden standpoint, if you multiply the above-mentioned costs, you would arrive at a staggering financial total.
Yet you can not try to tell me there is a price tag you can place on Sasha living to her fullest capacity. There is NO price tag on well-being. Is it costly? YES. But what I also know is that every single child struggling with a rare disease, however complex to navigate, deserves an unbridled full shot. We all do.
I do not know what will happen regarding the bi-annual review of our upcoming Medicaid application. What I do know is that when individuals furthest removed from this reality have the power to make medically impactful legislation, for better or for worse, they may choose to contemplate price tags over human decency and physical health. Officially in the United States, we do not ration health care. But cuts to Medicaid are certainly going to do that. My aim is to not let that happen.
________________________________________________________________________________________________________________
Joanne Huff comes to Courageous Parents Network as a long time follower and parent enthusiast of the organization. As the Mother of two girls, the oldest of whom has the rare disease MPS IIIA/Sanfilippo Syndrome, Joanne has benefited tremendously from the intimate parent interviews and candid, vulnerable story sharing throughout numerous thought provoking blog posts. As her daughter’s activities and lifestyle started to slow down with disease progression, CPN became a larger anchor in times of uncertainty and unrest. It is through this lens that Joanne hopes to share experiences and insights via the CPN blog.
Joanne completed nursing school after her daughter’s diagnosis, receiving her Bachelors of Science in Nursing from Plymouth State University, Plymouth NH. She enjoyed community liaison work with home care providers of adults with special needs up until her own daughter’s care became increasingly more involved. In addition to serving on the Boards of New England Regional Genetics Group (NERGG) and Adaptive Sports Partners through 2024, she has found great purpose in volunteer work advocating for policy improvements and change in Washington DC with the National MPS Society. In her free time, Joanne seeks balance and refuge with yoga, hiking and performing as an ensemble Soprano vocalist with the Pemigewasset Choral Society. When not blogging for CPN, Joanne enjoys sharing offerings on her personal Blog Folding Origami for God. She resides in Bow New Hampshire with her two daughters, Sasha and Nika, her husband Mike and her yellow lab Suki.
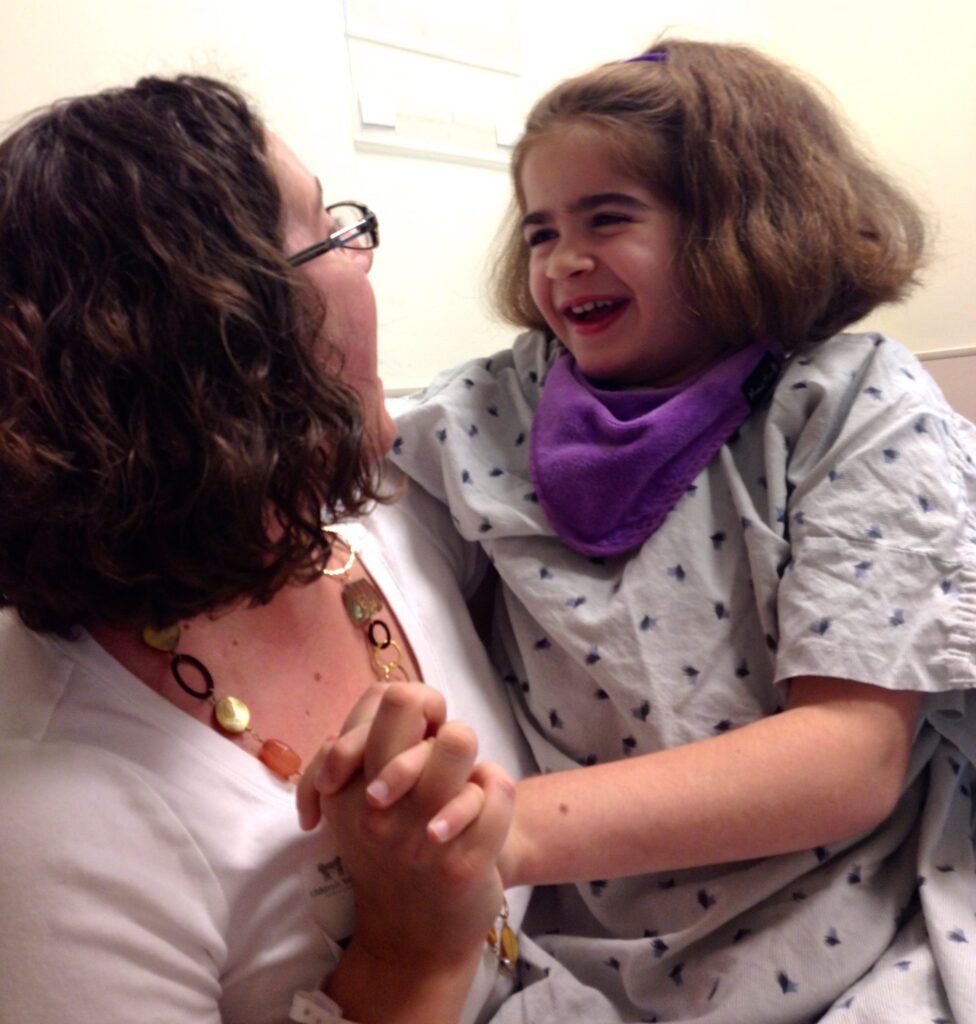
Eighteen years ago, my world was turned upside down when my daughter, Waverly, was diagnosed with Sanfilippo Syndrome. One month later, my son, Oliver, was given the same diagnosis. My family was living in London, embarking on a new career adventure when everything we had planned was no more.
My husband and I felt an extreme need to be back stateside to settle down, make a home, and build structure for the chaos we found ourselves now living. We were in a position where I could forgo my career to become the primary caregiver, devoting my time to the daily tasks of mothering two children with complex medical care needs. My husband worked to provide our family with insurance and financial stability. Most therapy appointments, doctor and equipment clinic visits, Medicaid applications, insurance appeals, and school forms were my responsibility.
In all the literature we read and conversations we had with other families, we were naïve about the impact severe neurological impairment would have on the children’s body systems as they neared the end of their lives. My husband and I made countless difficult decisions about their care. However, the most painful and gut-wrenching decisions revolved around feeding.
We opted for a G-tube when Waverly was 8 years old. She had been having trouble swallowing for several years. We thickened and puréed, but after some choking episodes, we had a g-tube placed. I took photos of her perfect belly and wept knowing our decisions were causing her to undergo surgery and pain. As parents, we weigh the options and make the best decision we can with the information we have at the moment. We constantly ask ourselves, “What is the ‘right’ decision?”
We continued with pleasure feeds, allowing Waverly to taste her favorite foods. We watched for signs of distress around eating, like squirming and crying. We noted signs of pain as we started a feed and then relief when we stopped. We would decrease rates and reduce volumes to maintain comfort. She began having more diarrhea and vomiting, spitting up formula during feeds. Waverly was experiencing edema throughout her body. We consulted with her team and made recommended changes, but her system continued to decline.
We had difficult conversations with providers we trusted. We weighed their guidance with our philosophy and ethics. I relied on my mother’s intuition, but Waverly was our guide. We followed her lead. Waverly was signaling to us that her body was tired.

It took time to see that feeding her was causing her pain. We charted every feed, how many milliliters and over what period. We noted any movement or grimace that we recognized as pain. We stopped and started, gave breaks, and switched to Pedialyte. We dripped tiny amounts of food into her belly only to stop as her body showed signs of distress. My husband and I both needed to agree that it was time to stop feeding.
We transitioned into a hospice approach focused on comfort. We had time to invite loved ones into our home to spend time with her, continue to make memories and build her legacy. She died in our bed days after she turned 12 years old.
I spent a significant amount of time perseverating on our decision to stop feeding her. I would be rendered inconsolable, and overwhelmed with guilt. My husband would walk me through the events, logically laying out the cause and effects, and why we came to our decision. Repeatedly organizing the facts allowed my emotional responses to quell. I needed that framework to assuage any guilt and confirm the decisions were made to alleviate the suffering of our daughter.
And we knew we had to do it all over again with Oliver.
We were practiced. Waverly once again smoothed the path for her little brother. We noticed the signs earlier and knew what adjustments to make. Our medical team was also more versed having navigated Waverly’s decline with us just three years prior. The decisions came quicker and with a tinge less doubt. Oliver died a few weeks before his twelfth birthday.
My guilt was lessened with Oliver’s death. I felt more confident in our decisions. I also felt more supported by all of those around me. My expertise was validated by Oliver’s care team.

As parents of children with rare diseases, we are often the experts in the room, explaining the nuances of our children to those more credentialed than we are. We bring binders and share literature to inform those caring for our children. We were fortunate to have a medical team who invited us to have a seat at the table for all decisions. And if they weren’t open to that, we found another provider who was willing to say, “I don’t know” and “let me consult with others”.
Having abandoned a career and spent fifteen years as a full-time caregiver, I wanted to build upon my children’s legacy. I wanted to work in a field supporting children like mine. I returned to graduate school and became a pediatric social worker and grief counselor. I work for a community-based hospice and palliative care agency in Washington, DC.
As a pediatric hospice and palliative care social worker, I support families as they navigate complex decisions. I see my role as ensuring full parental participation and advocating for the parents’ goals of care. I am in their homes, supporting the entire family system, building trust and rapport, ideally early on so a relationship is established as decisions become more complex.
I have utilized the Courageous Parents Network both as a parent and as a professional. The educational videos were especially helpful in normalizing my experience as a mother. And I found it validating to hear others vocalize my thoughts and feelings. As a social worker, I return to the same videos with the families I support, hoping for a similar outcome.
The new NeuroJourney tool is invaluable. I wish I had access to this when I was parenting my children. However, I am thrilled to have this instrument available to my patients and their caregivers. I have introduced several families to the website, exploring the impact severe neurological impairment has on their child’s body systems. The website provides information and tools to parents and providers.
I have found the GI section especially helpful as it addresses a caregiver’s innate need to nourish their child. It provides a guidebook for one of the most challenging decision points. By using this tool, I have watched families recognize the signs of feeding intolerance and decline in their children. It opened the door to an honest conversation about prioritizing comfort and adjusting goals of care.
My hope, as both a bereaved parent who held onto guilt and as a therapist who supports caregivers experiencing guilt, is that this tool can aid in adjusting to changes and navigating decisions. This information has the potential to improve caregivers’ confidence in their choices by providing clinical data and reducing the potential for a more complicated grief process.