On Practical Wisdom as the Art of Excellence
“For the man who is truly good and wise bears all the chances life becomingly and always makes the best of circumstances, as a good shoemaker makes the best shoes out of the leather that is given him.” — Aristotle, Nicomachean Ethics I.10
The alarm goes off at 2:47 AM. Not the clock but the pulse oximeter, which is a different animal entirely. My wife and I are moving before we are awake, a choreography so practiced that our bodies have memorized it faster than our minds have. Check the probe. Check her color. Check the rise and fall of her chest against the ventilator’s steady rhythm. My child is fine. It was a positional issue and the probe shifted on her toe. We resettle her. We resettle ourselves. The monitors quiet. The house resumes its mechanical breathing.
We lie back down. Neither of us sleeps.
In the dark, I find myself doing what I often do after the adrenaline has no more work to do: I begin to think through the night’s decisions. Did we make the right call? Should I have checked her temperature as well? What if it wasn’t just the probe? Was I too slow, or was I, in fact, exactly the right speed? This is not anxiety, or not only anxiety, but something more deliberate. It is a practice I did not choose so much as grow into, the same way a callous forms by repeated contact with rough material.
The ancient Greeks had a word for this practice. They called it phronesis. We translate it, a little flatly, as “practical wisdom” or “prudence,” though the philosopher Aristotle meant something far richer. For him it is the cultivated ability to perceive what a situation actually requires, and to act accordingly; not from rule, not from habit alone, but from a deep, seasoned attentiveness to the specific gravity of this moment, with this child, in this particular kind of dark.
If you are a parent of a medically complex child, you are already practicing phronesis. You may not have a name for it; but you know it.
Practical wisdom is not expertise in the clinical sense, though it can include clinical knowledge. You may have learned about the half-life of the rescue medication, the therapeutic index for various seizure meds, or the subtle differences between voltage-gated sodium or voltage-dependent potassium channelopathies. That knowledge is often necessary and always hard-won. But it is knowledge of universal facts that hold steady regardless of circumstance. Phronesis is different. It operates in the territory that textbooks cannot reach, the territory of particulars. Particulars like the specific quality of the cry that precedes a tonic-clonic, or the three-second window before a coughing fit becomes a desaturation.
Emma does not seize the way much of literature describes. She does not pale before; she flushes first and pales after. She does not stiffen first; she goes quiet. The monitors may say she is stable when, if you know her, you can see—by the particular set of her jaw and the way her hands are clenched—she is not okay. Something is building. This is not instinct, though it can look like instinct from the outside. It is the accumulated, deliberate act of paying attention over time. It is the eye of experience. And it is, in the fullest sense, a form of practical wisdom.
The practically wise parent recognizes that no protocol covers every situation because luck, that indifferent variable, regularly produces situations for which there is no protocol. Phronesis is what you exercise in the gap between the protocol and the moment. It is the ability to deliberate well under pressure, to hold two or three possible courses of action, weigh them against the specific texture of right now, and move. Not perfectly; but well enough. And then, afterward, in the dark, to review your actions—not to punish yourself, but to refine.
This is how practical wisdom grows. It is not given. It is made, in the repetition of hard nights.
There is a version of parenting advice that implies good parents are simply people with good intentions and warm hearts. This is not wrong, exactly, but I think it is insufficient. As they say, a sharp tool in untrained hands is a liability. Likewise, intention without discernment can cause harm in the most sensitive places such as the exam room, the IEP meeting, in the 2:47 AM alarm.
Our situation and things in it are akin to tools. Wealth, strength, access, opportunity. All of these are not good in themselves. They are instruments. A hammer in the hands of someone who does not know what they are building is just a thing that damages whatever it touches. But in the hands of a craftsperson, it builds something that lasts.
The same is true of everything that comes to us by luck; including the good luck of having a strong advocate for a partner, a generous specialist, a good insurance plan, a smooth stretch of weeks. These things are genuinely good. But they do not automatically make you a good parent. Practical wisdom is what converts good fortune into good action. It is the skill that looks at a stable week and asks, ‘What do I do with this?’ Do we push for the therapy evaluation we have been delaying? Do we rest, because rest itself is preparation? Do we make the phone call we have been dreading?
The prudent parent is not simply reactive, they are responsive. Reactivity is your nervous system’s answer to a crisis. Responsiveness is your character’s answer to each of life’s challenges. One is automatic. The other is cultivated.
There is an analogy, again borrowed from Aristotle, that helps illustrate what this kind of wise response to life looks like. A good shoemaker makes the best shoe possible from the leather available. Not the shoe they wished they had leather for. Not the shoe they could make if the leather were different. The best shoe from this leather, right now. A good parent makes the best of the circumstances they have. Perhaps that includes working to improve those circumstances, but it is not a life spent fantasizing about what they wish they had.
This is the practical wisdom available to us. Not the wisdom of better circumstances, but the wisdom fitted to these ones. The ‘leather’ of our situations—the diagnosis, the prognosis, the limitations of a body that requires extraordinary maintenance—are often poor by any conventional measure. And what’s more, our children’s lives are housed in systems that regularly treat them as line items instead of human beings. There is a relentless, compounding fatigue that makes every decision feel weightier than it should. And yet, something is still being made from this. I see it when my wife navigates a prior authorization call with a patience that has iron in it. A patience deliberately chosen because she has learned that fury spent carelessly accomplishes nothing for Emma, while fury channeled into clear, firm, documented language sometimes opens a door. That is phronesis. That is a shoe being made from difficult leather.
I see our good parenting in the 2:47 AM deliberation. It is instinct that is not quite instinct, the fast, practiced assessment that looks effortless only because it has been done hundreds of times and each time, slightly refined. I see it in the ability to hold open the question: what does she need right now? Not what does the monitor say? Not what does the protocol dictate? Instead we ask, what does she need, now, from us? We answer it well, or well enough.
There is one more thing worth naming, because it surprised me when I came to understand it. Practical wisdom does not eliminate bad luck. It does not, in the final accounting, protect Emma from the facts of her condition. What it does is reduce the surface area where bad luck can do additional damage. The practically wise parent is harder to catch off guard. This is not because they are unfeeling, but because they have learned from the work of attending to their child, to their own responses, to the difference between what they can control and what they cannot. They carry what they are choosing to carry; but, they carry it with technique.
You are already doing this. You do it in ways you probably do not credit yourself for, in the middle of the night, in the fluorescent offices, and in the ordinary hour when you look at your child and know—just know—what they need before they can ask.
That knowledge is not nothing. It is, in fact, everything. It is the good shoemaker’s art. The art of the excellent parent. The Good Parent.
And it belongs to you.
Phronesis is not a skill you acquire and then possess; you cannot develop it by reading about it. It is a practice which means it requires a repeatable form. Over time, I have come to rely on three questions I return to when the situation is unclear, the stakes are high, or I have just acted and am lying in the dark wondering if I acted well.
The first is: What does this moment actually require?
Not what do I fear? Not what does the protocol say? Not what did I do last time? The question I specifically ask is: What does this child, this hour, this specific circumstance actually require of me right now? This question slows the reactive nervous system just long enough for the responsive character to engage. It is the perceptual move that phronesis begins with: seeing clearly before acting.
The second is: What is the best I can do with what I have?
This is the shoemaker’s question. It releases you from the fantasy of better leather, the better diagnosis, the better system, the better version of yourself who got more sleep. It returns you to the only territory where excellence is actually possible which is here, now, with these resources, these constraints, this child. It is a question of radical presence. And it is, in my experience, the one that most reliably converts frustration into action.
The third is: What will I do differently next time?
Not what did I do wrong? That framing would lead to punishment, not refinement. Instead let’s ask, What will I do differently next time? This is the 2:47 AM question, the one I ask in the dark after the adrenaline has no more work to do. It is how the callous forms. It is how the instinct that isn’t quite instinct gets built, slowly, out of repetition and honest attention.
You don’t need to ask all three in sequence. Some moments only call for one but they are portable enough to carry each at all times. They fit in the exam room, the insurance call, the ordinary hour when you look at your child and feel the full gravity of what is being asked of you.
This is not a fix. These questions won’t lift you out of crises; but they will help you carry your burden with technique. A technique which, over time, becomes something very close to wisdom.
 Stephen Hager goes by his second middle name (he has three), Bud, because it’s easier to remember and baristas never misspell it. Along with his wife he is a caregiver for their 8-year-old daughter, Emma, who has pachygyria, a rare neurological disorder. He believes in taking an active approach to advocating for his child and others like her. To this end, he sits on various advisory councils at Children Hospital of Orange County (CHOC), volunteers on consulting and directing boards for various non-profit centers and lends his writing skills where he can. Experiencing a lack of support for parents of medically complex children, Bud founded a support group through CHOC focusing on parent-to-parent interaction. He is also a professor of psychology and has a small private psychotherapy practice.
Stephen Hager goes by his second middle name (he has three), Bud, because it’s easier to remember and baristas never misspell it. Along with his wife he is a caregiver for their 8-year-old daughter, Emma, who has pachygyria, a rare neurological disorder. He believes in taking an active approach to advocating for his child and others like her. To this end, he sits on various advisory councils at Children Hospital of Orange County (CHOC), volunteers on consulting and directing boards for various non-profit centers and lends his writing skills where he can. Experiencing a lack of support for parents of medically complex children, Bud founded a support group through CHOC focusing on parent-to-parent interaction. He is also a professor of psychology and has a small private psychotherapy practice.
For the uninitiated, the last day of February is set aside to honor people living with and alongside rare diseases. There are hashtags, purple ribbons, awareness campaigns, carefully chosen stock photos of smiling children in wheelchairs, copy about resilience. The grammar of awareness is familiar by now. It asks us to notice, to learn, to care.
But as I sat down to write about just how rare she is, something else came to mind.
She isn’t rare at all; she is the opposite. She is ubiquitous. She is the single most present thing in my life. We are two folds in the same tablecloth at the banquet of life, tugging and smoothing the same fabric, spilling on the same places, living inside the same stains.
Rarity is a statistical category. It lives in spreadsheets, in prevalence rates, in the language of funding cycles and research pipelines. It belongs to the way medicine sorts and prioritizes bodies, the way institutions decide which lives get legible, which conditions get named, which suffering gets indexed. All of that matters. It shapes who gets help and when. It determines which clinics exist, which specialists you can see without driving three hours and taking a day off work, which questions can be asked because there’s a billing code to hold them.
But none of that is how she exists to me.
To me she is the sound of her breath at 2:13 a.m., the way the house goes still when a machine alarm cuts through a dream. She is the weight on my chest when her body is cold and needs to borrow my warmth for a while. She is the particular way her laugh breaks open a room that is otherwise heavy with unspoken fear. She is the choreography of tubes and medications and the small, fierce rituals of care that bracket our mornings and nights.
This isn’t to say there aren’t rare aspects of her. There are several: a certain genetic mutation; her wondrous talent for making conversation without making it entirely about her trauma; her penchant for bringing people together; her friends and family who have been willing to grow with us and learn how her life rigidly demands flexibility.
Her rarity shows up in exam rooms when clinicians lean in a little closer to the chart, when we become case studies by accident, when we are thanked for our “patience” because there is no protocol for this constellation of needs. It shows up in the way things like insurance systems, school districts, transportation requirements all assume a default body and then quietly fail anyone who doesn’t fit inside that template. Her rarity shows up in the assessment forms with boxes too small to hold the truth, in the phone trees that loop endlessly when you try to explain that your child’s needs don’t align with the options on offer.
It has been tempting these past six years to view her rare diagnosis as an obstacle. As an intrusive “something over there,” while who she really is lives “over here.” To tell ourselves that if we could just cure it, get around it, un-dam the damn thing, then maybe the rivers of our life would finally flow. As if there is a normal life stalled somewhere upstream, waiting for us to clear the blockage so it can arrive on time and according to plan.
Meanwhile many of the things we hoped for have not come to be, and many of the things we dread are now here.
This is the futility of a hope that is only oriented toward the life we were promised rather than the life we are living. This kind of hope can become a way of postponing presence. A way of loving some imagined future version of your child more than the child who is breathing in front of you right now. It can turn care into a holding pattern with mantras such as we’ll really begin once this diagnosis loosens its grip; we’ll really live once the system stops being so disorienting; we’ll really rest once the crisis phase is over.
But the crisis phase is no longer just a phase.
Her diagnosis isn’t something that happens to her. It’s just one way of trying to understand one facet of her existence. It is the language that medicine uses to speak about her body. It is not the language she uses to speak about herself. And when I confuse those two, I start relating to an abstraction instead of a person.
Parsing out her biological rarity, then, is a comparison game; and I have no great interest in doing that. Rare, compared to what? Compared to whose body, whose baseline, whose imagined normal? Comparison is the thief of connection. It tempts me to measure her life against a statistical average and call the difference a catastrophe, rather than to meet the singularity of her being and call it a relationship.
Letting her diagnosis be just one part of the entirety of who she is lets me experience the passing of holidays, milestones, and awareness days with less emotional ambivalence. It lets me hold gratitude and grief in the same hand without asking either of them to justify being here. It lets me show up to Rare Disease Day without needing to perform inspiration or despair, without seeking absolution for experiencing conflicting (or unpopular) thoughts and emotions.
There are days when awareness campaigns feel like a thin layer of paint over a cracked wall. On those days I want to ask what awareness does when it doesn’t come with structural change such as respite care, or accessible housing, or reliable home nursing, or schools that don’t require parents to become full-time case managers just to secure basic accommodations. There are days when “honoring” feels like a euphemism for noticing without altering the conditions that make life so hard.
And there are days when I’m grateful for the simple fact of being seen, however imperfectly. For the provider who says, “I don’t know, but I’m willing to learn.” For the stranger who doesn’t look away when my daughter’s body draws attention in public. For the small mercies of community that appear in waiting rooms and online forums, in late-night messages between parents who recognize each other’s exhaustion.
Her diagnosis is rare, and yet her personhood is the absolute foundation of my facticity. This is the ground of my life now. The systems I move through, the language I use, and the questions I ask – about what counts as care, about whose bodies are considered costly, about how grief and wonder can coexist in the same afternoon – have all been rewritten by the daily labor of loving her.
As we honor Rare Disease Day, I hope a growing community takes time to reflect on the ways our culture struggles to make room for bodies that don’t conform to its narrow expectations of productivity, independence, and ease. My deepest hope is that we change the way we treat care as a private burden rather than a shared practice; because the truth is, people living with medical complexity are not edge cases. Rare diseases exist amongst our neighbors, our classmates, our colleagues, our family, and our friends.
She is rare, and she isn’t.
She is everywhere in my life: in the way I think about time now as something elastic, punctuated by alarms and appointments and the long, slow work of waiting; in the way I understand dignity as something that has nothing to do with efficiency or self-sufficiency and everything to do with being met where you are; in the way I imagine a good society as one that is built for the most vulnerable first, becoming gentler for everyone else.
On Rare Disease Day, I can hold the colored ribbons and the spreadsheet in one hand, and her warm, inconvenient, luminous presence in the other. I can honor the language of rarity without mistaking it for the truth of who she is. And I can say, with as much steadiness as I can manage: she belongs without qualifiers. Rarity is a framework for medicine and advocacy, not a measure of worth. She is life, up close.
 Stephen Hager goes by his second middle name (he has three), Bud, because it’s easier to remember and baristas never misspell it. Along with his wife he is a caregiver for their 8-year-old daughter, Emma, who has pachygyria, a rare neurological disorder. He believes in taking an active approach to advocating for his child and others like her. To this end, he sits on various advisory councils at Children Hospital of Orange County (CHOC), volunteers on consulting and directing boards for various non-profit centers and lends his writing skills where he can. Experiencing a lack of support for parents of medically complex children, Bud founded a support group through CHOC focusing on parent-to-parent interaction. He is also a professor of psychology and has a small private psychotherapy practice.
Stephen Hager goes by his second middle name (he has three), Bud, because it’s easier to remember and baristas never misspell it. Along with his wife he is a caregiver for their 8-year-old daughter, Emma, who has pachygyria, a rare neurological disorder. He believes in taking an active approach to advocating for his child and others like her. To this end, he sits on various advisory councils at Children Hospital of Orange County (CHOC), volunteers on consulting and directing boards for various non-profit centers and lends his writing skills where he can. Experiencing a lack of support for parents of medically complex children, Bud founded a support group through CHOC focusing on parent-to-parent interaction. He is also a professor of psychology and has a small private psychotherapy practice.
On a Repurposed Life
I noticed the bottle one afternoon while cleaning out the refrigerator. Dark glass. A narrow neck. It must have been the kind of bottle you don’t throw away right away because it held something worth remembering. I turned it in my hand and read the label: 2014. That was, by all accounts, a very good year. I remember receiving it now, who we were with, and the unspoken assumption that there would be many more like it.
At the time, I would have told you this was how a life was supposed to work. You laid things down carefully; you let them age, and you trusted that, when the moment came, you would know how to pour. That bottle belonged to a different life, one designed for long evenings and unhurried company, for the clink of glasses meeting midair and the smell of woodsmoke threaded through conversations about the future. All my yesterdays were so full of tomorrows.
And as I stare at the bottle, an unfounded guilt starts to gather.
Not the guilt of having broken something, but of having misused it. As though a life without a medically complex child could be opened fully and savored without interruption. Not necessarily a life without hardship, but hardships born lightly and moved through expediently. Before, I thought that suffering must be done nobly, with a composed voice and steady hands. Could life be measured based on what it actually holds and not just what I wanted it to hold? The bottle was never ruined after all; it just isn’t holding what it once promised to hold. I set it on the counter and kept cleaning.
Standing in front of the open fridge now, the analogy continues to unfold. The bottle is still sound, the glass uncracked. The wine held fast by an undamaged cork. The label remains crisp and legible, displaying, in my mind, so much more than year and vineyard. It is announcing a whole life built of the expectations of that younger version of myself.
Like so many years ago, I again did not throw the bottle away. This time, instead of returning it to the fridge, I rinsed it out, letting the water run until the last traces of the old vintage were gone. I peeled back the label slowly, careful not to rip apart the memories it contained. What remained was simpler than what had been promised.
The bottle, and the life that it represents, is not a failure. It has been repurposed, it is a vase now.
The admission lands with less drama than I may have expected. A vase is a modest thing. It does not hold intoxicating promises. It is meant to stay put, to be stable, to hold without calling attention to its own design. Before, I imagined myself a full bottle, offering something rich and expansive. I have become more like the vase, holding something much simpler yet necessary to keep something precious alive.
The world still demands the mindset of that former self though. It shows up in many areas of my life. My career that rewards the privilege of consistent momentum. The friendships that aren’t as easy to maintain now that I’m always requesting accommodations. The invitations to travel, the asks to show up, to say yes, all while having to calculate what it will cost at home. Conversations still open with What’s next? as though the future were a neutral resource. Even praise for me as a caregiver is spoken in the old grammar, with phrases that call me impressive, productive, or busy.
I’ve come to realize that the ache of who I once imagined I would become doesn’t fade just because I’ve given my role a new name. The world is still calling, regardless of my positive reframing. The sense that a life once forecast with confidence has come in under expectation reverberates even in the smallest moments, like when a friend texts to ask if I can meet for coffee, as though they are reaching for the older version of me. I have spent so much time living as though the person I might have been is here now, waiting for me to explain myself.
It has been an ongoing challenge for me to shift my understanding of what I want my life to look like now that my days are dictated by the needs of a medically complex child. And though I am no longer full of the vivacious libations I once was, neither am I empty. I now hold what is necessary for those that cannot survive without me. I am a vessel for a life that no longer photographs well, but that quietly persists. I have found mercy in letting my life as a caregiver be what it is without demanding it justify the change.
To live as the vase is to stop apologizing for not becoming the person I might have been. It is to acknowledge the uncomfortable certainty that I am the parent I have needed to become, and to understand that this is not a moral failure. The bottle was altered by necessity, not neglect. Life was altered by love.
 Stephen Hager goes by his second middle name (he has three), Bud, because it’s easier to remember and baristas never misspell it. Along with his wife he is a caregiver for their 8-year-old daughter, Emma, who has pachygyria, a rare neurological disorder. He believes in taking an active approach to advocating for his child and others like her. To this end, he sits on various advisory councils at Children Hospital of Orange County (CHOC), volunteers on consulting and directing boards for various non-profit centers and lends his writing skills where he can. Experiencing a lack of support for parents of medically complex children, Bud founded a support group through CHOC focusing on parent-to-parent interaction. He is also a professor of psychology and has a small private psychotherapy practice.
Stephen Hager goes by his second middle name (he has three), Bud, because it’s easier to remember and baristas never misspell it. Along with his wife he is a caregiver for their 8-year-old daughter, Emma, who has pachygyria, a rare neurological disorder. He believes in taking an active approach to advocating for his child and others like her. To this end, he sits on various advisory councils at Children Hospital of Orange County (CHOC), volunteers on consulting and directing boards for various non-profit centers and lends his writing skills where he can. Experiencing a lack of support for parents of medically complex children, Bud founded a support group through CHOC focusing on parent-to-parent interaction. He is also a professor of psychology and has a small private psychotherapy practice.
The team came by during early morning rounds, when the hallway lights were still dimmed and the night shift was only halfway gone. Our daughter was hooked up to long-term EEG monitoring, her head wrapped in gauze and wires. We stood around her bed, watching her sleep through a silence so loud it felt deliberate. A cough echoed from the hall and someone closed the door. Closing a door in a hospital is its own kind of diagnosis.
The neurologist scrolled through the results on her tablet, paused, and said almost conversationally, “Her background looks terrible.”
I said, “So you’re telling me she’ll never pass a DOJ screening.”
She blinked.
“What?”
“You said she has a bad background,” I said. “That’s going to be a problem for a background check,” and then, dramatically hanging my head, “there go our hopes for her getting a job with security clearance.”
The silence returned as the room recalibrated around my joke. The doctor looked back at the tablet. I looked at my daughter, whose fingers were curled over her thumb the way they always did when she slept, a habit that had survived every medication change. The feed pump chugged a few times.
Then the doctor stopped, looked up, and said, “Wait. Actually… that’s hilarious.”
I’ve replayed that moment over and over, not because the joke was particularly good, but because of what followed it. Relief, connection, maybe. But also something more complicated. A guilt for having joked at all. For not bearing the moment properly. For not suffering well.
Many people use humor in awkward situations to smooth things over. To clear the air when it gets thick with discomfort, the way you might crack a window. Sometimes that discomfort belongs to you. Sometimes it belongs to the room. Sometimes it’s shared, but unevenly distributed.
In other words, we joke because we feel guilty.
When I joked about my child’s EEG sounding like a criminal record, it was because I felt awful. As a parent, I had failed at the one job parents are not supposed to fail at: keeping their children safe, intact, progressing along the expected arc of things. I was not all I could be. I was not all I should be.
Guilt.
But the joke didn’t end there. Almost immediately, it turned back on me. Guilt for saying something so dark. For not being reverent enough. For not performing composure the way we imagine grief should be performed. Initially, when the joke collapsed in on itself, it became further evidence of my inadequacy.
This is bound up with a belief we rarely name but often enforce: that those who suffer are responsible not only for carrying their suffering, but for carrying it nobly. We praise the parent who remains gracious. We admire the ones who speak softly, who never seem sharp or strange or inappropriate. We tell stories about strength and resilience and grace under pressure, as though grief were a performance and composure the yardstick by which it should be measured.
By that standard, humor is suspect. Especially dark humor that announces just how poorly we are shouldering our suffering.
And yet, parents will tell you that they joke in these moments because it helps them cope. Because the weight of the moment is too heavy to carry straight on. Because exhaustion has stripped away the energy required for decorum. Because humor offers a brief exit ramp from a reality that feels otherwise inescapable. ‘You’re funny!’ ‘Thanks, it’s my trauma.’
All of that is true, but I don’t think that’s the whole story. These situate humor only as a reaction against crisis, as something that negates or briefly erases what is happening. Humor as disappearance or denial.
I think humor can be something else entirely.
I think it can be one of the clearest expressions of hope.
We often imagine hope as dignified. Upright. Calm. The kind of thing done with steady hands and a composed voice. Hope, in this telling, is clean and forward-facing and noble. It photographs well.
But hope rarely looks like that in practice.
More often, hope is clumsy. It slips. It misjudges the angle. It trips over its own good intentions. There is a slapstick quality to it that rarely makes it into the stories we tell later. It’s a physical sort of comedy born of being too close to the ground to maintain any illusion of grace.
The work of hope, especially in medical settings, is full of these moments. You set out to do the right thing and end up apologizing to someone on the phone who keeps transferring you to another department. You fill out the wrong form. You miss the deadline. You bring the wrong supplies. You do everything with sincerity and still manage to look ridiculous.
Humor is the controversial admission of this fact.
It is the acknowledgment that sometimes, while doing the work of hope for our children, we don’t look brave. We look foolish. And instead of pretending otherwise, we laugh. This is where humor begins to do something important.
Hope, when it appears beside hospital beds or in discussions that start with “I’m sorry to tell you…,” is often treated as a sacred, solemn obligation. Something to be handled with hushed voices and appropriate reverence.
But hope does not live in the abstract. It does not hover above the room. It lives here, in the present moment among IV poles and medication schedules and bad coffee and conversations you hope to never hear the end of. Humor brings hope back down to this level. A laugh in the middle of a serious chat doesn’t always cheapen what’s being discussed; it reanchors it. It reminds us that we are still here, still embodied, still subject to timing and gravity and fatigue.
Humor, then, is not a distraction from the work. It is one of the ways we stay in it without being swallowed.
Not every joke counts as hopeful though. Some humor keeps things exactly where they are. It relies on cruelty or stereotypes. It narrows rather than opens. It releases tension by pinning someone else in place.
Hope cannot live there.
Hopeful humor has movement built into it. It leans forward. It refuses to treat the present as a prison. It acknowledges reality without embalming it. It makes just enough room to keep going.
For me, that humor often uses the materials of missed sleep, long nights punctuated by alarms, numbers that matter more than they should, the ever-disparaging look from my daughter. It doesn’t deny the darkness. It doesn’t float above it either. It stays close. It works with what’s there.
A well-timed laugh can interrupt grief mid-sentence. It can loosen a body that has been braced too long. It can turn observation into participation, paralysis into action. Not because it solves the problem, but because it allows movement through it.
That movement is what makes humor hopeful.
When the doctor laughed that morning, something shifted. We were no longer performing “seriousness” for one another. We were simply there, together, attending to what was unfinished.
By keeping us here, together, and moveable, humor, like the hope it expresses, refuses to let suffering have the final word. Humor does not deny the darkness. It insists that even here there is still room to act, to respond, and to choose one another again, and again.
Those who hope will always have the last laugh.
 Stephen Hager goes by his second middle name (he has three), Bud, because it’s easier to remember and baristas never misspell it. Along with his wife he is a caregiver for their 8-year-old daughter, Emma, who has pachygyria, a rare neurological disorder. He believes in taking an active approach to advocating for his child and others like her. To this end, he sits on various advisory councils at Children Hospital of Orange County (CHOC), volunteers on consulting and directing boards for various non-profit centers and lends his writing skills where he can. Experiencing a lack of support for parents of medically complex children, Bud founded a support group through CHOC focusing on parent-to-parent interaction. He is also a professor of psychology and has a small private psychotherapy practice.
Stephen Hager goes by his second middle name (he has three), Bud, because it’s easier to remember and baristas never misspell it. Along with his wife he is a caregiver for their 8-year-old daughter, Emma, who has pachygyria, a rare neurological disorder. He believes in taking an active approach to advocating for his child and others like her. To this end, he sits on various advisory councils at Children Hospital of Orange County (CHOC), volunteers on consulting and directing boards for various non-profit centers and lends his writing skills where he can. Experiencing a lack of support for parents of medically complex children, Bud founded a support group through CHOC focusing on parent-to-parent interaction. He is also a professor of psychology and has a small private psychotherapy practice.
How an Instruction in Critical Care Became a Philosophy of Living
The room is dim except for the flickering of the pulse oximeter’s slow waveform. My hands are on her small body, rolling her onto one side. Even this simple act requires choreography: lift under the shoulder, steady at the hip, watch the feeding tube, the oxygen, the monitor cords that twist like roots if you’re careless. She exhales with a wet rattle that tells me which lung needs help. I listen, adjust the pillow under her ribs, and tilt her until the rhythm evens.
“Good lung down.”
I wrote good lung down in the notebook and now the words arrive before the memory does. A respiratory therapist said them once, many admissions ago, while angling her in the hospital bed just so. I can still see his hand on the rail, the confidence of habit. “You want the healthy lung on the dependent side,” he said, “so it can carry the weight, help the other expand.” He spoke like it was obvious. At the time, it wasn’t.
Now it is.
Her right lung was the good one that night, the left still recovering from pneumonia. Her body was warm and surprisingly heavy. Not dead weight, but dense with sleep and medication. I kept a hand against her ribs, feeling for the subtle lift that means air is reaching where it couldn’t before. Gravity does its slow work. I’ve done this hundreds of times, but it never becomes autopilot. Each turn asks for precision. Her body’s healing depends on such small degrees.
When her breathing steadies, I step back. The pulse-ox climbs: eighty-seven, then ninety-three. I exhale with her. Between each breath the room seemed to hold its own too. The phrase hums in my head like a refrain, less instruction now than ritual. The waiting that follows is its own form of care.
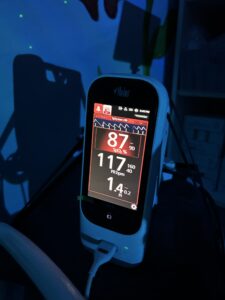 There was a night, early on, when I got it backwards. She’d been restless for hours, her numbers dipping, and I thought I could make her more comfortable by turning her away from the sore side. Within minutes the monitor shrieked. I remember the panic, the scramble to correct, the instant relief when I put her good lung down again, the breath returning. I learned that lesson in the blunt language of oxygen saturation.
There was a night, early on, when I got it backwards. She’d been restless for hours, her numbers dipping, and I thought I could make her more comfortable by turning her away from the sore side. Within minutes the monitor shrieked. I remember the panic, the scramble to correct, the instant relief when I put her good lung down again, the breath returning. I learned that lesson in the blunt language of oxygen saturation.
The body doesn’t lie about imbalance.
Still, I kept living by the wrong orientation in my own quiet ways. When people asked how we were doing, I gave the wins: a stable week, a smile, a rare stretch of sleep. I performed competence habitually and protectively, the way you perform posture. I didn’t want to burden anyone with the other side of it, the fatigue that seeps into bone, the private griefs that have no clear edge. I led with the good lung up, trying to keep what hurt from showing.
That’s what most of us do. We present the stable side first, compressing the rest beneath it. We tell ourselves it’s for others’ comfort, or our own control. But over time the pressure builds; the wounded parts can’t expand. Somewhere in those long hospital nights, I began to wonder if I’d been positioning myself backwards. I’d been protecting the hurt instead of giving it air. I’d been tucking it away, the way you’d cradle a wound and tell yourself it’s safer that way. But the physics didn’t work. Healing required exposure, dependence, gravity. The good lung had to go down so the bad could breathe again.
What if the same logic applied beyond the body?
She’s resting now, angled just right, her chest lifting in a steady rhythm. The good lung down, bearing the weight so the other can open. The physics of healing is counterintuitive. But the lungs know what the mind resists: expansion requires exposure.
other can open. The physics of healing is counterintuitive. But the lungs know what the mind resists: expansion requires exposure.
I think about that often, the physics of healing. How the stronger side becomes foundation, not façade. How what is whole steadies what is struggling. We’re taught a different pattern, of course: stay positive, be strong, keep the hurt tucked away. Especially in the world of care the performance of lone resilience becomes reflex. Strangers call you amazing. Providers say you’re an inspiration. You start to confuse endurance with enlightenment. You mistake competence with completeness.
But that’s bad lung down.
When we lead with where we are strong by ignoring where we are weak, we smother the places still trying to breathe. We compress the grief until it can’t clear, the exhaustion until it ferments into shame. “Good lung down” suggests letting stability carry the pressure so fragility can have air. The good doesn’t disappear; it simply takes a supportive role.
This integration is essential when dealing with loss that has no clear boundary; what some call ambiguous loss. The life I grieve is a ghost that coexists with the life I have. I cannot bury this grief, nor can I cut it out; the body is here, but the expected future is gone. The work is not to achieve closure, but to achieve meaning-making by allowing the healthy parts of my identity and my life to bear the weight of the reality, not to deny it, so that the wounded parts (the fatigue, the fear) can be positioned for true expansion. The fragile side must be seen and supported, not suppressed.
This isn’t wallowing, you aren’t sanctifying the bad lung. But this also isn’t extirpation, you don’t cut out the affected lung. You reposition it and allow the wounded parts to face the air, trusting the rest of you to hold steady. Healing isn’t heroic, it’s gravitational. It’s the slow rotation toward openness, the willingness to let pain expand instead of sealing it off.
Like respiratory care, it’s a practice. You listen, adjust, wait. You keep turning until the breath moves freely again. There’s tenderness in that discipline. The same precision I use for her body belongs elsewhere too. To my own heart, to the unseen spaces that tighten when I try too hard to protect them. The wisdom is already there: the strong must be yielding for the fragile to heal.
True healing comes not from hiding but from bringing the hurt to light and allowing stronger parts to hold. Which means that true strength comes from being supportive, not from dominating.
Good lung down. Not forever. Just long enough.
What, or who, are the ‘good lungs’ in your life? Who are you the ‘good lung’ for? Are you letting them hold your hurt? Are you holding theirs?
If you would like to share your response to Bud’s question in an email please send to connect@courageousparentsnetwork.org and we will be sure Bud receives it.
 Stephen Hager goes by his second middle name (he has three), Bud, because it’s easier to remember and baristas never misspell it. Along with his wife he is a caregiver for their 8-year-old daughter, Emma, who has pachygyria, a rare neurological disorder. He believes in taking an active approach to advocating for his child and others like her. To this end, he sits on various advisory councils at Children Hospital of Orange County (CHOC), volunteers on consulting and directing boards for various non-profit centers and lends his writing skills where he can. Experiencing a lack of support for parents of medically complex children, Bud founded a support group through CHOC focusing on parent-to-parent interaction. He is also a professor of psychology and has a small private psychotherapy practice.
Stephen Hager goes by his second middle name (he has three), Bud, because it’s easier to remember and baristas never misspell it. Along with his wife he is a caregiver for their 8-year-old daughter, Emma, who has pachygyria, a rare neurological disorder. He believes in taking an active approach to advocating for his child and others like her. To this end, he sits on various advisory councils at Children Hospital of Orange County (CHOC), volunteers on consulting and directing boards for various non-profit centers and lends his writing skills where he can. Experiencing a lack of support for parents of medically complex children, Bud founded a support group through CHOC focusing on parent-to-parent interaction. He is also a professor of psychology and has a small private psychotherapy practice.
Each morning begins in the small sensations that remind us we are alive.
The bubble of the kettle. The smell of coffee. The way light catches the rim of the mug, making even the ordinary seem briefly radiant. These are moments that belong wholly to the inside of our experience. We feel them before we ever name them. The warmth against our palms, the hum of a refrigerator, a child’s distant cough in another room. All of it arises in sensation before thought can measure or assign meaning.
 And yet, we are never only inside. Coffee is a compound of molecules; that light is a frequency; that coughing can be plotted as sound waves measured in decibels. We live, always, in this doubleness, moving between the world as it feels and the world as it is recorded. We live in a body that aches, stumbles, delights and then we invent the abstractions that allow us to make sense of what the ache or the joy might mean. Between these two is the tension of knowing we can never live entirely in either space. We are tethered to changing sensation just as we are ever compelled to find static language for our senses.
And yet, we are never only inside. Coffee is a compound of molecules; that light is a frequency; that coughing can be plotted as sound waves measured in decibels. We live, always, in this doubleness, moving between the world as it feels and the world as it is recorded. We live in a body that aches, stumbles, delights and then we invent the abstractions that allow us to make sense of what the ache or the joy might mean. Between these two is the tension of knowing we can never live entirely in either space. We are tethered to changing sensation just as we are ever compelled to find static language for our senses.
Perhaps this oscillation between immersion and distance, heartbeat and calculation is what makes us human: we are the creatures who measure what we feel and feel what we measure. It is in moments of extremity where we find that measuring either side becomes difficult.
Exploring this tension, philosopher Thomas Nagel once wrote about what he called the view from Nowhere. It’s an impossible vantage point where one sees the world stripped of all subjectivity, rendered in pure, detached clarity. From such a height, emotion and circumstance fall away; all that remains are facts, patterns, causes. Against this, there stands the view from Here with its thick, gauzy embodied immediacy of our personal lives, from which every sound, texture, and heartbeat is felt before it’s understood. The view from nowhere seeks precision and coherence. The view from somewhere clings to meaning, to what it feels like to be a person in a body, loving another person in theirs.
Both views are real, but they speak different dialects. We spend our lives crossing the invisible bridge between these two, wanting to know what’s true, yet unable to let go of what’s ours.
For parents of medically complex children, this tension becomes more than philosophical. It almost becomes the air we breathe. What’s more, we can never rest fully in either. The Here demands tenderness and attention, the kind that can feel the weight of her trust as she melts into your arms. This is the precious ground that friends, family, and fleeting visitors get to stand on. Holding a hand or singing a song, with love unburdened by the brutal calculus of a medication schedule or the terrifying consequence of waiting too long into a seizure to give oxygen. Then there is the Nowhere, which pulls just as hard, insisting only on the cold, unblinking precision of milligrams, milliliters, and flow rates. This is the domain of the provider, where the body is viewed through the necessary lens of protocol and data. Both places, populated by both peoples, are necessary.
To parent a medically fragile child though is to live on the fault line between love and logistics, between the memorable and the measurable. We are forever translating, reading the body as data and the data as life. Always feeling so burdened to find answers in order to make the right decisions.
It is exhausting.
Each step further into the dark brightness of medical parenting feels like an ascent up the mountain into the cloud of unknowing. A climb into thinner air where what once seemed solid begins to shimmer and blur. The higher we go, the ground of the everyday where we once believed love and reason could coexist without fracture begins to erode, and more distance stretches between the Here and the Nowhere.
This widening itself isn’t a problem. All parents, in one form or another, live within the tension between presence and abstraction. We watch our children play, delight in their laughter, then measure their growth on a chart and calculate hours of sleep or minutes of screen time. With enough community, family, and practical support, this balance holds. But for parents of disabled, medically complex, or fragile children, the gap widens until the span feels unbridgeable. Sustaining both perspectives can stretch even the most resilient heart past what ordinary networks can hold. The oscillation that once felt like breathing begins to feel like gasping.
When the ground between Here and Nowhere begins to quake, what parents need most is not to choose a side but to find a companion who can walk the fault line with them. And for parents like us this guide is Pediatric Palliative Care.
Unfortunately, many of those who could benefit from palliative care enter into it too late, often because palliative care is often misunderstood for hospice. However, its most powerful role begins at the moment of diagnosis and especially whenever the medical complexity starts to cause significant family strain, regardless of prognosis.
Its work is not to collapse the Here and Nowhere, but to reveal their interdependence and to steady the traveler caught between them. It does not dissolve medical demands—the Nowhere remains—but what it does is gently make room for the Here.
Neither the Here nor the Nowhere is sufficient alone. The child’s life insists on both.
If you find yourself constantly translating data and gasping for breath, remember that seeking palliative care is not a failure but an act of self-preservation that will help medical precision to become a form of care, and tender presence to become a form of healing.
It is love learning to breathe again.
 Stephen Hager goes by his second middle name (he has three), Bud, because it’s easier to remember and baristas never misspell it. Along with his wife he is a caregiver for their 8-year-old daughter, Emma, who has pachygyria, a rare neurological disorder. He believes in taking an active approach to advocating for his child and others like her. To this end, he sits on various advisory councils at Children Hospital of Orange County (CHOC), volunteers on consulting and directing boards for various non-profit centers and lends his writing skills where he can. Experiencing a lack of support for parents of medically complex children, Bud founded a support group through CHOC focusing on parent-to-parent interaction. He is also a professor of psychology and has a small private psychotherapy practice.
Stephen Hager goes by his second middle name (he has three), Bud, because it’s easier to remember and baristas never misspell it. Along with his wife he is a caregiver for their 8-year-old daughter, Emma, who has pachygyria, a rare neurological disorder. He believes in taking an active approach to advocating for his child and others like her. To this end, he sits on various advisory councils at Children Hospital of Orange County (CHOC), volunteers on consulting and directing boards for various non-profit centers and lends his writing skills where he can. Experiencing a lack of support for parents of medically complex children, Bud founded a support group through CHOC focusing on parent-to-parent interaction. He is also a professor of psychology and has a small private psychotherapy practice.
We have been told that to be resilient is to stand apart. To weather the storm unmoved, to endure without breaking, to carry the weight without complaint. Fathers especially are given this story. The good father is the oak: tall, steady, admired precisely because he does not need to lean. He shelters others but never asks to be sheltered. His strength is measured by how little he requires.
This myth has a certain beauty to it. We do not carve statues in the shape of vines; we carve them to look like pillars. All that is soft is gone, what remains is that which is hard or has been hardened. And yet, when you live long enough inside the weight of grief and care, the myth begins to feel brittle. A father who cannot bend, who cannot admit need, eventually snaps. The oak rots from the inside. The story I inherited about resilience has left me lonelier than I know how to name.
I did not really begin to question this until I found myself sitting at my daughter’s bedside, watching her chest falter in the dark. One breath would come, ragged and shallow, then a pause too long. Then another gasp, as if her small body was unsure whether to continue. In those moments, she did not fight. She yielded. She let the air and the mask, and our trembling hands do the work. She trusted that she could rely on what held her.
Her resilience was not in resistance but in reliance. And it startled me. Because if resilience for her is reliance, if her survival is the sum of many hands, many ties, many threads, why have we been taught to imagine resilience as the opposite? Why have we been told that to lean is failure, that to rely is weakness?
Endure in silence, carry your grief like a private stone, prove yourself by not needing anyone. This script makes us solitary. It distorts fatherhood into isolation, as though to love well is to disappear into a fuzzy invisibility. But a single knot, no matter how tight, cannot hold anything on its own. Only when the knots are tied together do they form a net. A father’s resilience, I am beginning to believe, is not found in how firmly he can stand alone but in how deeply he can rely and be relied upon. Resilience is reliance. Strength is not in separation but in connection.
There have been other moments, lower ones. Sitting on the floor holding my daughter when she is too weak to play, to sit, to do much but be held. I trace her small fingers as she drifts in and out of awareness. I often cry then, not from crisis but from the sheer fact that I cannot change her body, cannot take away the fragility she carries every day. Her eyes sometimes meet mine here for a moment before they close. She does not flinch from my weakness. She doesn’t need me to be unshakable; she needs me to be here. A father willing to remain, even if that means relying on her gaze to steady him.
This is the reversal our culture resists: fragility is not the opposite of resilience, but its ground. My daughter’s life has taught me that. The ventilator, the feeding tube, the medications, the meal trains, the help around the house, the thoughts and prayers and good vibes whispered over her—all of it is reliance. And yet it is precisely in this web of dependence that her life continues. Resilience emerges not in being untouched by need but in being held within it.
A spider’s web offers a better image of resilience to me now than an oak. The web trembles. It breaks. But it is also repaired, rethreaded, renewed. Its strength lies not in rigidity but in flexibility, not in singular hardness but in the pattern of connection. Each thread relies on the others; each knot tied to something beyond itself. Fragility is not erased; it becomes part of what holds it all together.
Fathers are rarely given permission to see themselves this way. We have inherited a silence, a script that says we must carry the weight without asking to be carried. And so, we rarely speak to each other about care, about grief, about the unbearable tenderness of watching a child suffer. We retreat into the myth of the oak and call it love. But what if fatherhood were something else entirely? What if resilience has always been reliance, and our silence has only deepened the fracture? I imagine naming aloud the weight of nights spent pacing hospital corridors, the helplessness of waiting rooms, the fear of not being enough. Not to prove endurance, but to weave ties. To hold each other as surely as we hold our children. What if fatherhood was not a fortress but a net?
Reliance does not mean passivity. It means fidelity. To keep showing up even when you cannot fix, to remain present when nothing changes, to lean and be leaned upon. This too is strength. When I sit beside my daughter during a seizure, I cannot stop it. All I can do is hold her hand, call her name, wait for her to return. My resilience in that moment is my reliance, on her will to come back on my wife’s presence, on the small circle of love that refuses to let go.
This is why yielding has become, for me, another name for love. To yield is not to surrender the bond but to trust it more deeply. To stay when you cannot control. To let others carry you when you cannot carry yourself. Yielding is not weakness. It is reliance. It is what nets are made of.
And in the end, this is what remains: not solitary strength, not the illusion of the oak standing alone, but the quiet fidelity of ties that hold. My wife’s hand in mine. Friends who ask the second question. Machines that breathe for my daughter until she can breathe again. My daughter herself, teaching me without words that life is carried by yielding. When I get to thinking like this, she looks at me as if to say, “Of course it takes more than one person. You’d last what, maybe 2 minutes on your own? 3 tops if someone left you snacks.” Alas, she is non-verbal, and I don’t read minds.
The myth told me that to be a resilient father was to stand apart. My daughter has shown me that resilience is the opposite, it is to stand together. To be one knot in a net strong enough to hold the weight of the nothingness of grief. To yield to reliance, and to find in that yielding not failure but promise.
Resilience as reliance, not resistance.
These ordinary instants are the ones that change your life.

Stephen Hager goes by his second middle name (he has three), Bud, because it’s easier to remember and baristas never misspell it. Along with his wife he is a caregiver for their 8-year-old daughter, Emma, who has pachygyria, a rare neurological disorder. He believes in taking an active approach to advocating for his child and others like her. To this end, he sits on various advisory councils at Children Hospital of Orange County (CHOC), volunteers on consulting and directing boards for various non-profit centers and lends his writing skills where he can. Experiencing a lack of support for parents of medically complex children, Bud founded a support group through CHOC focusing on parent-to-parent interaction. He is also a professor of psychology and has a small private psychotherapy practice.
The morning light, soft and diffused, bathed the nursery walls in gentle hues. My daughter, a few months old, lay on her back, her eyes locked on the mobile spinning above. Her clumsy hands swiped at the air. Then, it struck. A subtle twitch. Her head jerked forward, a tiny nod, her limbs tensing. I dismissed it as a baby startle, a quirk of her growing body. But then, a quiver. A tightening. Another. And another. These were no flukes—a rapid, relentless clenching squeezed the breath from me. Her head dipped again; her small frame locked in a silent, terrifying dance.
In that ordinary instant, a ritual we’d repeated countless times, time split. The soft light hardened, the quiet room rang hollow, and dread coiled in my gut. What was this? What gripped my child? Could this be… more? Fears, shapeless yet piercing, stabbed at my fraying mind.
Life twists on such moments, doesn’t it? A single breath—a glance—upends everything. Time, once a steady stream, shatters into jagged pieces, each reflecting a fractured reality. How do we grasp this? How do we endure when an unremarkable second carves a new existence? I offer no answers, only questions, lingering in the space where certainty crumbles. Here, time splinters, grief hushes, and the caregiver’s burden dawns—a solitary watch over a world forever changed.
 After that moment, time warped. Were they days? Weeks? For a place with so many clocks, time doesn’t seem to exist in hospitals and clinics. The waiting rooms reeked of sterile air, white coats drifting past. Each second crawled—a blood draw, a consultation, an EEG. My daughter’s spasms, those brief, eerie twitches, were trapped on video, replayed, picked apart. Doctors spoke in crisp bursts, their words sharp yet slippery, meaning evading me. Time stalled, a stagnant pool mirroring a warped present and an uncertain future.
After that moment, time warped. Were they days? Weeks? For a place with so many clocks, time doesn’t seem to exist in hospitals and clinics. The waiting rooms reeked of sterile air, white coats drifting past. Each second crawled—a blood draw, a consultation, an EEG. My daughter’s spasms, those brief, eerie twitches, were trapped on video, replayed, picked apart. Doctors spoke in crisp bursts, their words sharp yet slippery, meaning evading me. Time stalled, a stagnant pool mirroring a warped present and an uncertain future.
Then, the years—or what felt like them—blurred. Therapies, medications, whispered hopes dashed against unyielding reality. Nights snapped apart with anxious wakings; days rolled into cycles of appointments, new drugs, fresh side effects—a tightrope walk between relief and ruin. Small wins faded under looming setbacks; milestones twisted into shadows of what might have been. Birthdays, seasons—slipping like water through a cracked cup, lost forever.
In crisis, time defies measure. A single twitch swells, flooding the mind with dread, while years shrink to a fleeting echo. For us, teetering on this edge, the ordinary haunts: feeding, bathing, holding—each a fragile stand against the unknown. Every laugh, every cry, stings with what was and what might be.
You see other parents—at the park, in the store. Their kids sprint, climb, chatter endlessly. They map out birthday parties, school plays, a future unfurling. You watch, and grief claws at you—not for what’s gone, but for what never will be. A simple life, snatched by fate’s twist.
This grief creeps in early, like a morning (mourning?) fog curling into your days. You study your daughter, tracing every fleeting smile, knowing some will never return—at least not as you dreamed. Guilt gnaws: if you grieve, are you ungrateful? If you mourn tomorrow, do you cheapen today? You love her fiercely and desperately, cherishing each touch. Yet the ache lingers, a quiet echo of what might have been.
This grief is a testament, not a betrayal. A testament to the depth of a love that stretches beyond the present, beyond the limitations of what is. It is a love that mourns the absence of a future that was, in its own way, already a part of you. You are, after all, made to care. And to care is to feel the sharp edge of loss, even before the final parting.
It’s not the hospital’s chaos that undoes you. It’s the quiet. Folding laundry, the soft fabric evoking tiny limbs. Stirring tea, the steam a fleeting balm. Sunlight spills through the kitchen window, warm and gold. A song hums on the radio—then stabs, too heavy to bear. And then, it hits you.
No crisis looms, no doctor drones on. You’re just living—or trying to. But grief ignores your rhythm, striking like an uninvited shadow. A tiny shirt whispers lost dreams. A spoon’s clink rings with unanswerable questions. Her shampoo’s scent clings. Her hand nestles in yours—all a fragile tether. A memory flashes from the beforetime, before fear, before doubt, when the ordinary wasn’t laden with dread. These moments are sacred. And unbearable. The mundane betrays you, hiding sorrow in its folds. The ordinary instant tests you—a monument to what was and won’t be.
You try to explain—to friends, family, coworkers. You weave words into sentences, stories. But they don’t grasp it. How could they? They see a child, a parent, a routine life. Beneath that, lurks a fear they can’t touch, a constant hum of dread thrumming through you. Every breath, every smile, weighs heavy with what they’ll never know.
The world spins on. Sun rises, seasons shift, plans bloom—vacations, promotions, tomorrows. Their lives surge forward while yours staggers, snagged between appointments, therapies, rare slivers of calm. You’re not alone in body, perhaps, but in spirit—an exile in a fractured realm. Your past’s upheavals bleed into today’s ordinary, a rift no story can span.
‘Why?’ gnaws at you, a relentless echo in quiet corners. Why her? Why this jagged path? You scour books, conversations, solitary nights for answers, craving a thread of order in the tangle of your days. But silence stares back, vast and unyielding, mocking your pleas. The sheer randomness—the cruel unfairness—threatens to swallow you whole.
So you forge meaning, stacking it brick by brittle brick. It glows in small triumphs—her fleeting grin, a steady day—moments of raw connection. You craft a tale of resilience, devotion, an anchor against the storm. Is it real? Or just a shield, a way to press on when despair tugs? Does meaning dwell in crisis, or do we wrest it from the void to survive? The questions hover, unanswered, a tightrope between surrender and fragile hope.
How Do We Know When Life Has Changed?
In one of those most ordinary instants, I was scrolling social media and came across a post by the Courageous Parents Network. It was a simple post with a splendid quote from Joan Didion, “Life changes in the instant. The ordinary instant,” followed by a caption prompting me to write about a time my life changed in an instant. And just like that, this blog post was born. But before I wrote it all out, my initial thoughts were as follows:
If life changes in the instant, and if ordinary instants are precisely those that don’t stand out, how do we know which  moments will change our life? And how would we even know if our life has changed at all? Do we only see the shift later, tracing the crack it left? Or do we live as if every mundane second brims with potential to reshape us? We long for stability—routines, plans, a tomorrow like yesterday was. But perhaps the answer is not in chasing the moments that change us, in searching for the grand, dramatic shifts, or even in the comfort of predictability. Perhaps it lies in living fully within the moments that don’t seem to matter at all. In noticing the small, subtle details of our lives, always. To the way the light falls across your child’s face. The sound of their breath. The warmth of their hand in yours. This isn’t a call to compartmentalize through hypervigilance, it’s a call to integrate your ordinary instants and live.
moments will change our life? And how would we even know if our life has changed at all? Do we only see the shift later, tracing the crack it left? Or do we live as if every mundane second brims with potential to reshape us? We long for stability—routines, plans, a tomorrow like yesterday was. But perhaps the answer is not in chasing the moments that change us, in searching for the grand, dramatic shifts, or even in the comfort of predictability. Perhaps it lies in living fully within the moments that don’t seem to matter at all. In noticing the small, subtle details of our lives, always. To the way the light falls across your child’s face. The sound of their breath. The warmth of their hand in yours. This isn’t a call to compartmentalize through hypervigilance, it’s a call to integrate your ordinary instants and live.
Live, not only in the gasps of catastrophes, or in the pages of research articles, or on brightly colored awareness days, but in the ordinary. Because in a life where time is fractured and grief is a constant companion, the ordinary becomes extraordinary. Because one day, these moments, these seemingly insignificant instants, may be the ones that mattered most.
These ordinary instants are the ones that change your life.
Stephen Hager goes by his second middle name (he has three), Bud, because it’s easier to remember and baristas never misspell it. Along with his wife he is a caregiver for their 8-year-old daughter, Emma, who has pachygyria, a rare neurological disorder. He believes in taking an active approach to advocating for his child and others like her. To this end, he sits on various advisory councils at Children Hospital of Orange County (CHOC), volunteers on consulting and directing boards for various non-profit centers and lends his writing skills where he can. Experiencing a lack of support for parents of medically complex children, Bud founded a support group through CHOC focusing on parent-to-parent interaction. He is also a professor of psychology and has a small private psychotherapy practice.