How do I do what Andalyn’s pediatrician counseled me when he said, “I know it’s difficult to always feel like you’re living on the edge of a cliff, I wish I could change that. When we get to a place where we need to discuss death and dying, I will be straightforward and honest with you. For now, keep walking that path without peering too far over the edge.”
How exactly does one walk on the path that traces its way along the edge of uncertainty’s cliff without “peering too far over the edge?” How do I get better at living in the shadows of uncertainty especially in times when death feels far too close? Is that even possible? If it is, what does that look like? Does it look different for different people or is there one basic answer that works for everyone? Is there even an answer to be found at all?
These are questions that have taken me years to find the courage to be willing to acknowledge and voice. I wish I could say I have this all figured out. I wish I had insight and knowledge that might help others looking for the same answers, but the truth is, these questions are still fresh and new to me. In a lot of ways they are just beginning to tear their way through my soul so they can crawl into the daylight. As these questions are working their way to the surface, I’m afraid to look too closely and yet I’m unable to look anywhere else at the same time.
I want to understand. I want answers. Mostly I want there to be tricks somehow to magically get back some illusion of control over the fears that loom heavy just outside my grasp but always just above my head. While I definitely don’t have many concrete answers, there are a few things I have stumbled across–mostly by accident–that help (sometimes). Being honest with safe people, turning to writing and music, and using facts to challenge fear as a way to ground myself in the present are the things I most often do in my attempts to not peer too far over the edge.
Being honest with safe people for me means finding and confiding in those rare humans who truly understand the power of what it means to be present. Sharing what I am going through without worrying about how I will be perceived allows me to focus my energy to get below the superficial layers and dig into the deeper root of what I am struggling with. Safe people allow time and space for pain, grief, anger, fear and any other feelings that are generally unpleasant, without trying to change or eliminate them. They understand that when feelings are allowed to exist as they are and to be fully experienced, they can be powerful channels to release the pent up emotions that cause headaches, issues sleeping, panic attacks, and other physical problems. The sheer pressure to keep all my crazy wrapped up in a neat little box so the world doesn’t see it, is incredibly intense and isolating. Having safe people to let it all out with has been one of the most–if not THE most–beneficial things I have discovered.
When I am desperate to feel anything other than the numbness that living in a constant state of revolving crisis inevitably creates, I sometimes use music to connect with my repressed feelings. A powerful song can tell the story of my pain when my own words feel inadequate. Sometimes music is the only thing that can break through my walls and connect the two parts of myself back together again.
In times when I am not fragmented by trauma, I often turn to writing. Writing gives me a way to externalize pain and give it a voice. It creates a space to both fully explore and disconnect from painful experiences, often in the same piece. It also gives me a way to have some control over my grief and trauma. When I write I feel like I can hook the pain with words and pull it out of me, being careful that as it disentangles it doesn’t also unravel my soul. After the pain is drawn out of me, I can capture it inside carefully woven descriptions that get tethered to the page. I can take my time to work through things little by little or I can allow myself to become completely immersed in the words.
For times when I need to push back against the monster of PTSD, I do my best to try to ground myself in the present moment by using facts and experience to challenge my fears. It’s barely effective, though, against the memories that haunt me. When we are in the hospital, the past plays over and over like a bad movie on a loop forcing me to relive the trauma from prior hospitalizations and multiple bouts of sepsis Andalyn has battled. I desperately look for any differences between then and now to reassure myself that she isn’t dying–yet. Sometimes this is the extent of the comfort I can scrounge up between the beeping medication pumps and the pages sent by a bedside nurse to summon help in the middle of the night when things take a turn in the wrong direction. Focusing on the moment and the progression of needed interventions gives me a way to measure how many steps it is to the edge of the cliff.
I don’t know that I can ever stop worrying that every fever could become the infection that takes Andalyn from me and carries her over the edge. I have come to accept that Death will be quietly waiting in the corner of each of her hospital rooms but being able to shift from ‘what if she dies’ to ‘she isn’t dying yet’ is most certainly the only way I will survive the reality of him being there at all.
About Amanda
I live in Aurora, Colorado with my 12 year old daughter, Andalyn. I am divorced so I am navigating this journey as a single parent. We came from New Mexico in 2014 so that Andalyn could get the medical care she needed at Children’s Hospital Colorado. After spending 15 months in the Ronald McDonald house, we officially became Colorado residents when we moved into an apartment. Andalyn has complex medical needs and multiple challenging diagnoses. I have spent her life striving to make things for her as normal as possible because so little of her world is in our control. I have no idea how much longer she will get to be here but she has already lived far longer than many suspected she ever would. I survive most days on Diet Dr Pepper, sarcasm, and a little bit of dark humor sprinkled in for good measure. I am a very sensitive soul that feels all things deeply but I have found a way to thrive through the power of connection. That connection is what makes it possible for me to do impossible things for as long as they need to be done.
Amanda is a CPN Blogger in Residence, an opportunity available through support from Sanofi.
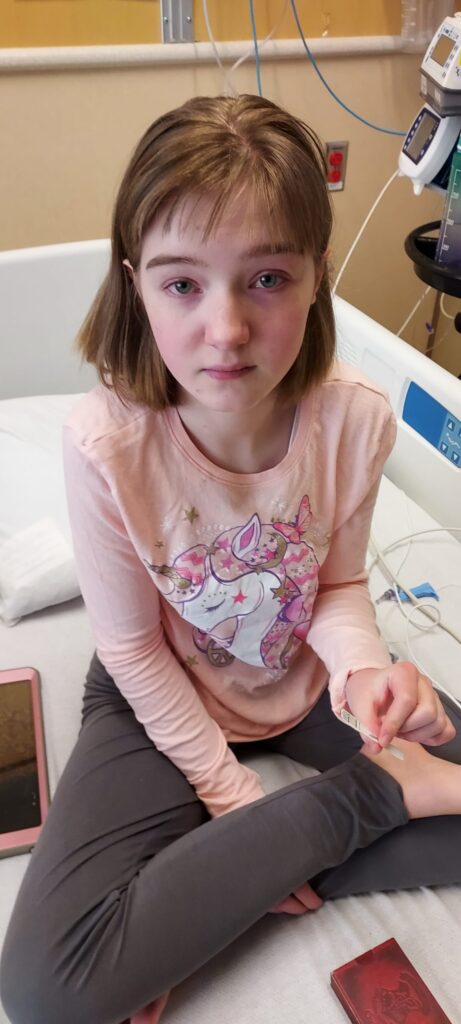
There was a time in Andalyn’s life that I would have done absolutely anything for answers about her medical condition, heck even for the hope of a hint at an answer. I took lots of “long shots” and tried every single intervention her medical team could think of out of sheer desperation to find the magic fix that would give us the life I dreamed of for her. I felt like a crazed treasure hunter searching for the buried gold under some impossible to find ‘X’ on a map that felt like no one even knew existed.
Not knowing what was wrong with my daughter was torture and the uncertainty was killing me slowly. My own will to live was getting swallowed up in her disease. Every decision I made was in the shadow of unrealized expectations. With all my energy focused on keeping her alive so she could be “cured,” the irony was that we weren’t really living much at all. We were alive obviously, but we were not experiencing much outside of medical treatments or interventions and I was doing my best, constantly in survival mode, just to keep going.
Looking back I definitely have regrets that I didn’t make more room for time to be happy, for living in the moment, and for letting her illness be whatever it was instead of feeling compelled to try to change it. I didn’t know how to live in the middle of constant crisis and I didn’t yet understand that acceptance is not the same as giving up. I spent years fighting against a reality I just couldn’t face head on. I didn’t know how to stand under the weight of the truth that my child could die at any moment without being crushed by it. This took time and only recently has become something I have been able to articulate.
As I re-evaluated the way our life was playing out and began to think through what quality of life looked like for us, a new perspective began to take shape, clarifying what I wanted for my little girl. I was sick with anxiety over the idea of sharing my feelings with her medical team after figuring out what was important to us.
I had a paralyzing fear that they would call child protective services or that the ability to make decisions for my child would be taken away from me. I worried they would not understand the way I was feeling and wondered if they would continue to support me after changing my goals for her care. My approach to decision making related to interventions was starting to shift to a quality-of-life perspective. I was afraid this perspective would be mistaken for giving up, or worse, not wanting to take proper care of her anymore.
It took incredible bravery to open up about the most vulnerable pieces of my heart and what kind of life I wanted for my child. I was nudged in the right direction by a churning mixture of hope for something better, exhaustion trying to maintain unsustainable routines, and eventual acceptance that my “fairy tale life” was going to be very different than I planned. With wisdom and guidance from her pediatrician and really good palliative care support, I slowly began to understand that gratitude and grief can coexist in the same experiences. I know now that I can be excited and feel relieved when something that I fought to get for Andalyn works out while also grieving the fact that she needs whatever I had to fight for in the first place. I can also be filled with relief when a fever doesn’t mean a life threatening infection and still struggle against unpredictable waves of trauma from being in the hospital yet again.

Because of the support I have, I have come to understand that it is ok-even normal-to hold overwhelming sorrow in one hand while holding joy in the other. I am learning how to shift from frantic denial to quiet acceptance through the experiences of holding suffering and peace in the same moments.
I haven’t given up on my daughter by any means. I still advocate for what Andalyn needs. I most definitely still participate in, and seek out, treatments but the motivation driving me along with my decision making process are shifting in relation to her baseline. I still fight for her as I always have and I always will. Only now, I have the insightful ability to see meaningful purpose in those things that I decide are worth fighting for.
________________________________________________________________________________________________________________
About Amanda
I live in Aurora, Colorado with my 12 year old daughter, Andalyn. I am divorced so I am navigating this journey as a single parent. We came from New Mexico in 2014 so that Andalyn could get the medical care she needed at Children’s Hospital Colorado. After spending 15 months in the Ronald McDonald house, we officially became Colorado residents when we moved into an apartment. Andalyn has complex medical needs and multiple challenging diagnoses. I have spent her life striving to make things for her as normal as possible because so little of her world is in our control. I have no idea how much longer she will get to be here but she has already lived far longer than many suspected she ever would. I survive most days on Diet Dr Pepper, sarcasm, and a little bit of dark humor sprinkled in for good measure. I am a very sensitive soul that feels all things deeply but I have found a way to thrive through the power of connection. That connection is what makes it possible for me to do impossible things for as long as they need to be done.
I feel like the word is too nice of a term. It sounds overly positive. Vigilance is a good thing, so surely being extra vigilant is even better. Right? Let me assure you it is not. Since the day I learned about my daughter’s life-threatening medical needs, I have lived in a constant state of hypervigilance to varying degrees. For someone looking in from the outside, it can sometimes look like I am just a giant control freak–which is true–but a separate issue. Other times, it can just look like I’m extremely organized and almost normal. Most often, however, it looks like I am overthinking and overcomplicating everything.

In Andalyn’s case, more often than not what you see is most definitely not what you get. If you happen to catch us in the grocery store without any of her medical gear you would never know she has medical issues at all, much less intestinal failure and other complex diagnoses. You would likely see a mother who appears a bit too impatient with a daughter who never stops moving or asking questions and who voices her constant observations of the world just a little too loudly and with a little too much honesty. You would see a bright-eyed, healthy child full of energy and sassy spunk. You would see a young girl on the cusp of her teen years just a few inches shorter than her exhausted and slightly disheveled mother. If you looked really closely you might even see that Andalyn is still very much wrapped up in the innocence and wonder of a child half her age, one not yet aware that she should be too old for such things as cartoons, toys, or believing in the magic of fairies, unicorns, and Santa Claus.
What you wouldn’t see are the various scars that cover her chest and abdomen from nearly three dozen surgeries. You wouldn’t see the central line or the gastrostomy tube. Her massively enlarged spleen, artificial pulmonary heart valve, liver damage, and intestinal failure are also hidden beneath her shirt along with many layers of cumulative trauma.
Andalyn’s central line for the required daily IV infusions puts her at increased risk for central line associated bloodstream infections (CLABSI). This means she has to be hospitalized every single time she gets a fever of 100.4 or higher for close monitoring and IV antibiotics. She has endured several of these infections, so I have seen first hand how scary they are and how rapidly they can progress to sepsis, twice nearly killing her. These traumatic memories insist on living at the edge of my thoughts, pointing out danger, and reminding me of how fragile her life is. Even when I am doing my absolute best, I can’t protect her from certain things, and this knowledge haunts me. Chronic hypervigilance makes letting my guard down feel nearly impossible, and somewhere along the way it became my unwanted, constant companion. My relationship with hypervigilance is definitely one of love/hate.
This hypervigilance has endowed me with nearly superhero powers of observation. I’m even able to recognize and detect problems before they can fully manifest to her medical team. Hypervigilance also helps me to follow care routines consistently. In moments when I want to give up or when things feel impossible, somehow it lends me strength and the ability to keep moving forward for Andalyn. Hypervigilance is a huge part of what makes me an excellent caregiver and has helped save my daughter’s life on more than one occasion. Unfortunately, it is also one of the biggest reasons I feel caregiver burnout. Feeling like I have to always be watching for signs that things could fall apart and constantly adjusting things in her care to mitigate those risks takes a huge toll on me.

Because all of my energy has been focused on her medical needs for so long, chronic hypervigilance has made finding balance in life incredibly difficult. So difficult in fact, that I couldn’t figure it out on my own. It’s hard to enjoy the good moments when I’m constantly trying to anticipate and avoid the next crisis. I am fortunate to have an excellent pediatrician who recognized the need for palliative care support and am blessed to have an amazing GI team. Her team understands the need to live a good life, and so they prioritize our goals for quality of life in treatment plans and interventions, which makes all the difference. They say it takes a village to raise a child, but when that child has complex needs your village is often filled with people you didn’t choose. More often than not, they come with name badges, stethoscopes, and clinic appointments. I may not have been able to pick the people in my village and it may not look like the one I envisioned long ago, but I can’t imagine being in a better one. Throughout the ups and downs her medical team has been there for us. They help me reevaluate what is important and what is ok to let go of, reassuring me when I struggle to do that and always trying to help make things easier in the day-to-day routines. In my opinion, this kind of support has been as important–perhaps even more so–than the medical interventions have been. The support, perspective, and shared decision making is what makes the rest of what is required of me possible.

Because of chronic hypervigilance, the way I see my child has been changed and so has how I see the world. Despite wonderful support from the medical team I often find myself struggling with feelings of inadequacy and deep guilt when striving to find balance. Hypervigilance compounds my insomnia and makes my anxiety feel unsurvivable at times. The idea of putting Andalyn in settings where I have to trust others to do what I do has been panic-inducing more times than I care to admit. Andalyn recently had an opportunity to participate in a service project with some other girls from church. A close friend who is familiar with her medical needs offered to take care of her since she was already going. Andalyn was so excited that I thought she would wiggle right out of her pants. I knew this would be good for her. Yet as soon as the door closed, instead of enjoying some much needed “me” time, it mostly felt like my intestines had been filled with razor blades and then tied into knots. Regrettably, as I spent the day battling with hypervigilance and his good friend, anxiety, I was robbed of the peace and rest I so desperately needed. I tried with minimal success to take comfort in knowing that this was precisely the quality-of-life experience her team and I had been working so hard to give her and reminding myself of that helped to ease some of the angst. Still, I was barely able to enjoy the fact that she was getting to do something normal and had to push against the waves of intrusive thoughts filled with fear and worry that came and went, leaving me exhausted by the end of the day.

Trying to figure out how to prioritize my energy and focus when every detail in our life feels equally demanding and important often takes an outside perspective. Having a medical team to help figure out which things to let go of and who provides reassurance that it is ok to occasionally take a break from being hypervigilant helps me in that process to find the balance I am striving for. Even with their support and encouragement, I am still learning how to be comfortable with putting aside hypervigilance. While I am not yet in a place where I get to really enjoy it, I suspect eventually I will get there. Like everything else in our world, this, too, is a process.
________________________________________________________________________________________________________________
Amanda has a BS in psychology from the University of Wyoming and has recently written a book, A Tattered Soul: A True Story About Chronic Illness and a Mother’s Journey from Brokenness to Acceptance. She is the sole caregiver for her daughter, a child with complex medical needs including intestinal failure and chronic Total Paraenteral Nutrition (TPN) dependence. Her daughter’s needs have taught her to be a skilled advocate driven by the desire to help others navigate their way through the world of chronic caregiving.
 Sometimes I think about the deterioration of my marriage as just another casualty of Andalyn’s complex medical needs. After its death, this companionship was laid to rest in the basement of my soul, tucked carefully between unrealized hopes for more children and growing old with my best friend. The transition from being a “we” to a “me” was something I was not prepared for even though it was not entirely unexpected. I have somehow found my way through the past nine years, but being just a “me” frequently feels like it’s not enough.
Sometimes I think about the deterioration of my marriage as just another casualty of Andalyn’s complex medical needs. After its death, this companionship was laid to rest in the basement of my soul, tucked carefully between unrealized hopes for more children and growing old with my best friend. The transition from being a “we” to a “me” was something I was not prepared for even though it was not entirely unexpected. I have somehow found my way through the past nine years, but being just a “me” frequently feels like it’s not enough.
With all of the arrogance and selfishness of an uninvited, unwelcome guest, divorce barged into our home just as the leaves were beginning to fall and the smell of pumpkin spice everything filled the air. Divorce wasted no time taking over the whole house. Because of Andalyn’s medical needs, anxiety, depression, anger, and grief had already moved in with me so having an additional intruder made the house pretty crowded. When divorce showed up I didn’t have room to unpack his many suitcases bulging with hurt feelings, painful memories, and broken dreams, so I shoved all his crap into closets, under beds, and behind storage bins full of Christmas decorations just so I wouldn’t have to see any of it. I did my best to ignore the messes that divorce created all over the house so I could focus on Andalyn.
 This sort of “tunnel-vision focus” wasn’t really much different than the way things had been all along. With all of my energy being poured into our chronically ill child, it didn’t leave much left to tend to my marriage. Sleeping in separate beds to share the tremendous burden of 24-hour care seemed like a good idea in the beginning. We figured at least one of us got to sleep every other night. But the separation grew steadily and spread beyond sleeping arrangements to all the other areas of our relationship. As the days stretched into months and the months into years, I barely noticed the distance increasing between us. A thousand little things, and a few that were not so little, steadily piled up until they buried our relationship under a thick blanket of resentment and unmet needs. Ironically the thing that initially deepened our connection–her medical fragility–was now the very thing forcing us apart.
This sort of “tunnel-vision focus” wasn’t really much different than the way things had been all along. With all of my energy being poured into our chronically ill child, it didn’t leave much left to tend to my marriage. Sleeping in separate beds to share the tremendous burden of 24-hour care seemed like a good idea in the beginning. We figured at least one of us got to sleep every other night. But the separation grew steadily and spread beyond sleeping arrangements to all the other areas of our relationship. As the days stretched into months and the months into years, I barely noticed the distance increasing between us. A thousand little things, and a few that were not so little, steadily piled up until they buried our relationship under a thick blanket of resentment and unmet needs. Ironically the thing that initially deepened our connection–her medical fragility–was now the very thing forcing us apart.
It was very painful for me as Andalyn’s dad and I struggled to figure out the dance of joint custody and co-parenting. Initially, it almost felt like we were still married but living in separate houses because we still spent a lot of time together. As Andalyn’s medical needs became more complicated and life took us in different directions, however, the last threads of decency between us unraveled. It took several years and some significant events to put us back on a path headed in the right direction. Even so, her dad and I struggled for a long time to find our way back to a place that felt like friendship. Finding our way out of conflict was a very difficult process, but eventually things shifted into a place of empathy, kindness, and mutual cooperation. Compassion smoothed over the broken places and created a space for us to stand together on softer ground.
Without careful tending of this new landscape, the softer ground we have managed to cultivate could quickly become inundated with thorns, rocks, and other harmful barriers. It would be easy to get frustrated and be unkind to one another. When things come up unexpectedly, we try to be understanding and consider the circumstances in each other’s lives. Being flexible and keeping Andalyn as the focus really helps us work together to find creative solutions and avoid a multitude of hard feelings.
Navigating any relationship takes work, communication, and a mutual spirit of cooperation. I would dare to say that on occasion I have found myself working harder on this in our relationship now that I am divorced than I was capable of at times in the marriage. I am also far more capable of being objective now that we are living separate lives.
Having a medically fragile child adds a compounded complexity to divorce so finding ways to keep the peace definitely is the best way to go. Reflecting on all the ups and downs it took to learn how to do this, there are a few things that stand out that have been particularly helpful.
The first and most important is that we finally figured out how to establish consistency. Lack of consistency between households for a medically fragile child can literally be a matter of life and death. Differences in parenting styles, routines, and activities between households have to be carefully balanced with medical, emotional, spiritual, and physical needs of everyone involved. This is not an easy task. It is exponentially harder if there are unresolved misunderstandings or a lack of good communication.
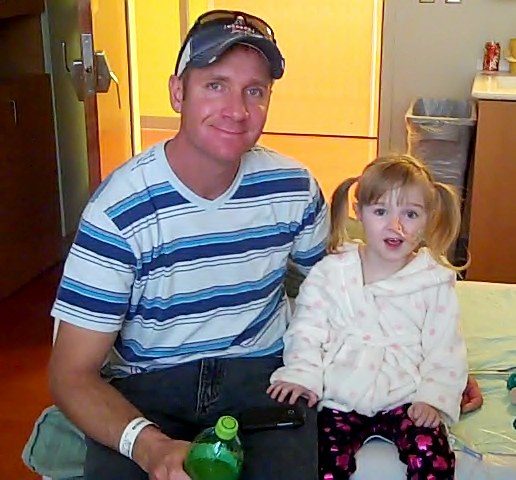 Clear and ongoing communication is incredibly important and so this means involving the medical team on occasion. Allowing providers to shoulder the responsibility to ensure that Andalyn’s medical needs get communicated correctly when there is a potential conflict or when something needs to be clarified puts Jonathan and me on the same level. More importantly, it puts everyone on the same team. However, if I am put into the role of being the teacher or the person dictating how something needs to be done, it can easily upset the delicate balance of power by shifting me into a role of being his supervisor in a way, and that only leads to resentment. The benefits of letting clarification regarding when something needs to be done differently, or explaining the importance of doing something in a specific way, takes me out of the middle and means we both receive information and instructions from the source. Working together with the medical team in this way has taken some of the burden off of my shoulders and has helped to rebuild some areas of broken trust. This simple but incredibly powerful approach has prevented many potential conflicts before they could even happen.
Clear and ongoing communication is incredibly important and so this means involving the medical team on occasion. Allowing providers to shoulder the responsibility to ensure that Andalyn’s medical needs get communicated correctly when there is a potential conflict or when something needs to be clarified puts Jonathan and me on the same level. More importantly, it puts everyone on the same team. However, if I am put into the role of being the teacher or the person dictating how something needs to be done, it can easily upset the delicate balance of power by shifting me into a role of being his supervisor in a way, and that only leads to resentment. The benefits of letting clarification regarding when something needs to be done differently, or explaining the importance of doing something in a specific way, takes me out of the middle and means we both receive information and instructions from the source. Working together with the medical team in this way has taken some of the burden off of my shoulders and has helped to rebuild some areas of broken trust. This simple but incredibly powerful approach has prevented many potential conflicts before they could even happen.
The best way for us to maintain good communication and consistency in Andalyn’s medical needs is to utilize a written plan. Having both a written care plan and a schedule means I don’t have to worry about forgetting important details, and her dad doesn’t have to remember a massive amount of information about her constantly shifting needs. He lives in a different city about 80 miles away from us, so co-parenting and visitation arrangements have to include careful cooperation otherwise Andalyn could suffer life-threatening complications. As various things have changed over the past few years, the situation has made it necessary for me to take on nearly all of Andalyn’s care, even when she spends time with her dad. It is not a common scenario for anyone to have to spend long periods of time with an ex-spouse and their new family. Fortunately, what was initially very painful and terribly awkward has slowly softened into mildly uncomfortable and less awkward. Choosing to do whatever it takes so that my daughter can spend time at her dad’s house may not be easy but it is intentional. An unexpected blessing has unfolded with the beginning of a new and cautious friendship.
Finally, organization makes all the other strategies come together. In Andalyn’s case, going anywhere longer than a few hours is a tremendous amount of work and demands careful planning. When the time comes to get things ready for a visit with her dad, even for just a day trip, it can take hours to make a plan to adjust medical care for travel, gather needed and emergency supplies, and then organize it all into a somewhat manageable chaos. Overnight trips with her dad are not always a possibility. So when they do happen, in order to make things go smoothly and for Andalyn to be safe, good organization is critical. It takes advanced coordination with her supply companies to schedule deliveries so that I have everything on hand that she will need before we go.
The way I handle this is by using a checklist I made that has everything she needs on it. This is my attempt to avoid a crisis–at least one related to things I can control–so I don’t forget anything that has to go back and forth between households. She has nearly 70 different items I have to pack related specifically to her medical needs for trips so obviously I can’t just toss a few things into a backpack at the last minute and drop her off for a weekend somewhere. While it’s not a big deal if I forget a personal item, clothing, or a toiletry, if I forget her medications or supplies, her dad can’t just make a Target run to grab a $3500 infusion pump or a $1000 bag of Total Parenteral Nutrition along with a spare toothbrush from the toothpaste aisle. In addition to remembering all her stuff I also need to make sure that I pack everything in a way that is easy for her dad to quickly find the things he needs. He appreciates my efforts to make doing her medical care easier for him and safer for Andalyn.
 Advanced planning, careful organization, care plans and checklists, anticipation of potential needs, making intentional effort to work together and prioritizing Andalyn’s needs ahead of my own are all necessary if I can ever hope to master the art of a good divorce. It certainly creates a tremendous amount of extra work for me but her dad is incredibly appreciative. When he acknowledges the sacrifices I make it feels wonderful to be validated. The peace of mind that comes from knowing at least in those visits I am doing everything I can to meet her medical needs AND she gets to be happy–that is what makes all the hard stuff 100% worth it.
Advanced planning, careful organization, care plans and checklists, anticipation of potential needs, making intentional effort to work together and prioritizing Andalyn’s needs ahead of my own are all necessary if I can ever hope to master the art of a good divorce. It certainly creates a tremendous amount of extra work for me but her dad is incredibly appreciative. When he acknowledges the sacrifices I make it feels wonderful to be validated. The peace of mind that comes from knowing at least in those visits I am doing everything I can to meet her medical needs AND she gets to be happy–that is what makes all the hard stuff 100% worth it.
________________________________________________________________________________________________________________
About Amanda
I live in Aurora, Colorado, with my feisty daughter and crazy cat. Andalyn has complex medical needs and multiple challenging diagnoses. I have spent her life striving to make things as normal as I can for her because she has already fought a lifetime of battles. Through a combination of faith, grace, my hypervigilance, and her incredibly tenacious spirit somehow she continues to beat the odds and has already lived longer than many suspected she ever would. Because I feel everything deeply, I have learned to cope with the challenges of meeting her needs through my writing, the power of connection, and bits of hope I find scattered along the way. I have been writing essays and short stories since I was a child but recently I accomplished my life long dream to publish a book. My novel, A Tattered Soul, is the true story of my journey coming to terms with Andalyn’s life-threatening illness and its undefined prognosis. When I am not writing or caring for Andalyn I enjoy sleeping, finding ways to help others, baking anything delicious, and watching TV. I survive most days on copious amounts Diet Dr Pepper, sarcasm, and a little bit of dark humor sprinkled in for good measure.

You might think that the hardest part about caring for a child with a chronic illness would be the day-to-day medical needs involved. That part is not easy by any means, but for me that is not the most difficult aspect of taking care of Andalyn. After the newness wears off, things start to feel normalish, or normal-adjacent as I like to say, as her medical care eventually become part of the routine. What actually wears me down is the never-ending care coordination and advocacy required to get her the care she needs. Whether it be quick and simple things like sending messages to her medical team to follow up on something minor, or complex and time consuming things like coordinating all the pieces necessary for her to go to school, it feels like a majority of my time and energy is consumed by advocacy.
When engaged in the war of advocacy, my weapons can’t be traditional weapons of warfare. Obviously, that not only would be ridiculous and ineffective, but also would make caring for a child quite difficult because prison tends to restrict freedom and other minor details. As such, I need to use different weapons and unconventional armor. Instead of tactical gear, I utilize logic and facts to prepare for these battles. Instead of a shield, I protect myself with research and knowledge about my rights. Instead of grenades, I use letters of medical necessity and other documentation. As much as I wish sometimes I could launch a missile to destroy obstacles standing in the way of what we need, I know that I have to utilize the drone strikes of persistence and self control to advance on these particular battlefields.
Sometimes I crash the drone when my temper gets the best of me. Other times in trying to carefully maneuver my way through a delicate situation, I stumble on a land mine that blows everything to pieces and a medivac has to pull me out of the carnage. These battles fought in my war of advocacy are as physically and emotionally draining as they are time consuming and ugly. And they are not without injury. Battle fatigue and PTSD in the war of advocacy is very real and can cause significant damage. Sometimes battle scars heal quickly and fade away over time until they are nearly invisible. Other times, pieces of shrapnel get lodged so deep they can’t be removed and then when conditions are just right, the old wound throbs once more.
There will always be another obstacle to overcome, another enemy to defeat, or another foreign land to navigate. The rules of engagement, however, pretty much stay the same even when the battleground changes or new adversaries appear. The temptation to go AWOL or get discharged for disorderly conduct is hard to resist at times, but honor, loyalty, and the full weight of the responsibility I shoulder for my child, all remind me to focus on the mission at hand. The strength and endurance I need to survive isn’t gained through physical conditioning or through practicing drills. Past experience and knowing who to radio for backup if I get into trouble are key to surviving these unique battles and living to fight another day.
Recently, the company that provided Andalyn’s IV nutrition and central line supplies announced it would be closing. Her medical team did everything they could to ensure a smooth transition to a new company. The GI nurses provided a list of the exact supplies that Andalyn needs, and with the exception of one or two items, the company confirmed they would be able to supply those things. To bridge the gap, the GI nurses generously gave us what the company wouldn’t provide until a more long-term solution could get figured out.
Our current TPN pharmacist also reached out to the new pharmacist to discuss Andalyn’s unique needs, encouraging them to order the special supplies in advance so that by the time we transitioned, they would have everything Andalyn needed. In an effort to reduce stress for me, while maximizing quality of care for Andalyn, she also worked with the medical team and me to coordinate the timing and other details of the transition. She even sent some extra supplies with the TPN deliveries leading up to the change to ensure Andalyn would have what she needed until the new company got things up and running.

Despite reassurance from the new company, I quickly discovered what a nightmare it was to work with them. All the effort and advocacy for Andalyn seemed to have been in vain. In the very first delivery, they substituted most of the items on her supply list for their standard supplies. They also refused to provide several items, including those necessary for weekly dressing changes and a second pump for her IV fluid boluses. When I called to correct what I assumed was a mistake, I was told the supplies they sent were “close enough” and “basically the same” and that I could order the specific supplies I wanted online myself but they would not provide anything different than the standard items they have in stock.
I reluctantly agreed to try one of their dressings. I put it on the opposite side of Andalyn’s chest, as far away from her Broviac as possible, in case she had a reaction. Sure enough, the next day she was bleeding and had a rash spreading across her chest. I removed the dressing and took pictures to send to her GI team with an update before I called the company. When I described how her allergy to the wrong dressings manifests in a blistering, itchy rash that she then scratches until she bleeds, it made no difference. The response I got was, “We don’t special order supplies or deviate from our standard procedures until WE determine it’s absolutely necessary. Even then, we only consider it after she tries everything we have available so we can decide if our products work for her or not.”
I was livid that she was being forced to ‘test’ their products to see how bad the reaction would be when we already knew which products were safe and worked best. I pointed out that someone with a nut allergy would never be expected to eat multiple foods with nuts just to see how sick they would get, and yet this was what they were forcing my child to do. Apparently we had very different definitions for what “necessary” means. Sometimes in the war of advocacy you have to choose your battles. This was a hill I was willing to die on, so I went to war for my child.

As for the second pump I asked for to infuse IV fluids, they refused. They wanted me to use gravity for IV fluid infusions when needed. Gravity drips make sense in a hospital setting or for a bedbound patient, but would be unrealistic for us. Even after I explained Andalyn uses a custom IV pole that would not work to do a gravity infusion because it is roughly three feet tall, they still refused to provide a pump for IV fluids. Instead they insisted she use a standard IV pole or a medical backpack and offered to send either of those.
I couldn’t get them to understand that even if I could somehow fit a bag of TPN, IV fluids, and formula, plus the TPN and feeding pumps into a medical backpack (which is impossible), it would be far too heavy for a child to carry. Obviously, I can’t put a standard IV pole in my car but the one I designed and built for her fits perfectly right next to her on the back seat. She can’t take a standard IV pole to school, the grocery store, or the park either. A standard IV pole also does not fit in our bathroom and other areas in our small condo. The one I made, however, allows Andalyn to move independently wherever she needs to go. One year I even figured out how to mount her TPN inside a rolling backpack that I turned into an accessory for her Halloween costume so she could trick or treat easily with her TPN.
Insisting my child give up her mobility and independence rather than provide a pump for IV fluids was not only unrealistic, it was poor patient care. Eventually we chose a different solution for IV fluids, but it was still very inconvenient. I would be lying if I didn’t admit I got a tiny bit of satisfaction when the TPN pump failed and a replacement had to be brought to me in the middle of the night on a weekend. The irony is that this emergency trip could have been avoided if they simply provided us with a second pump.
In the end, despite using everything in my arsenal, including a letter of medical necessity, calls, emails, and specific orders from her GI doctor, the company still refused to provide what Andalyn needed. Since it is useless to negotiate with terrorists, I had no choice but to go lethal and call in special forces to destroy basecamp and evacuate us from enemy territory. Intell pointed me in the direction of a potential asset in the form of a new homecare company. There was no fighting for resources, conflict or tense engagements over territory when we retreated there to take up refuge. Instead, we engaged in effortless peace talks and successful negotiations. Andalyn now has the things she needs to be comfortable, and I have the supplies that she deserves and that I need to keep her safe. Most of all, I have a new-found ally as I continue to wage the war of advocacy.
Having to struggle on the battlefields of this war, I have grown far more than I ever thought I was capable of. I am much stronger now than I was when I started basic training and I have become quite skilled in the utilization of the unique weapons required for this special form of nonviolent warfare. Even though I won this battle, it didn’t come without a cost: her pain and suffering, my anxiety, and sleepless nights. There were also some (not-so-minor) casualties-several large pieces of my sanity. Thank goodness for a medical team willing to climb into the trenches to fight beside me and call in the calvary when I need reinforcements. I may be on the front lines, but I have a powerful army behind me and I know that’s the only way I will ever be able to win this war.
________________________________________________________________________________________________________________
About Amanda
I live in Aurora, Colorado with my 12 year old daughter, Andalyn. I am divorced so I am navigating this journey as a single parent. We came from New Mexico in 2014 so that Andalyn could get the medical care she needed at Children’s Hospital Colorado. After spending 15 months in the Ronald McDonald house, we officially became Colorado residents when we moved into an apartment. Andalyn has complex medical needs and multiple challenging diagnoses. I have spent her life striving to make things for her as normal as possible because so little of her world is in our control. I have no idea how much longer she will get to be here but she has already lived far longer than many suspected she ever would. I survive most days on Diet Dr Pepper, sarcasm, and a little bit of dark humor sprinkled in for good measure. I am a very sensitive soul that feels all things deeply but I have found a way to thrive through the power of connection. That connection is what makes it possible for me to do impossible things for as long as they need to be done.
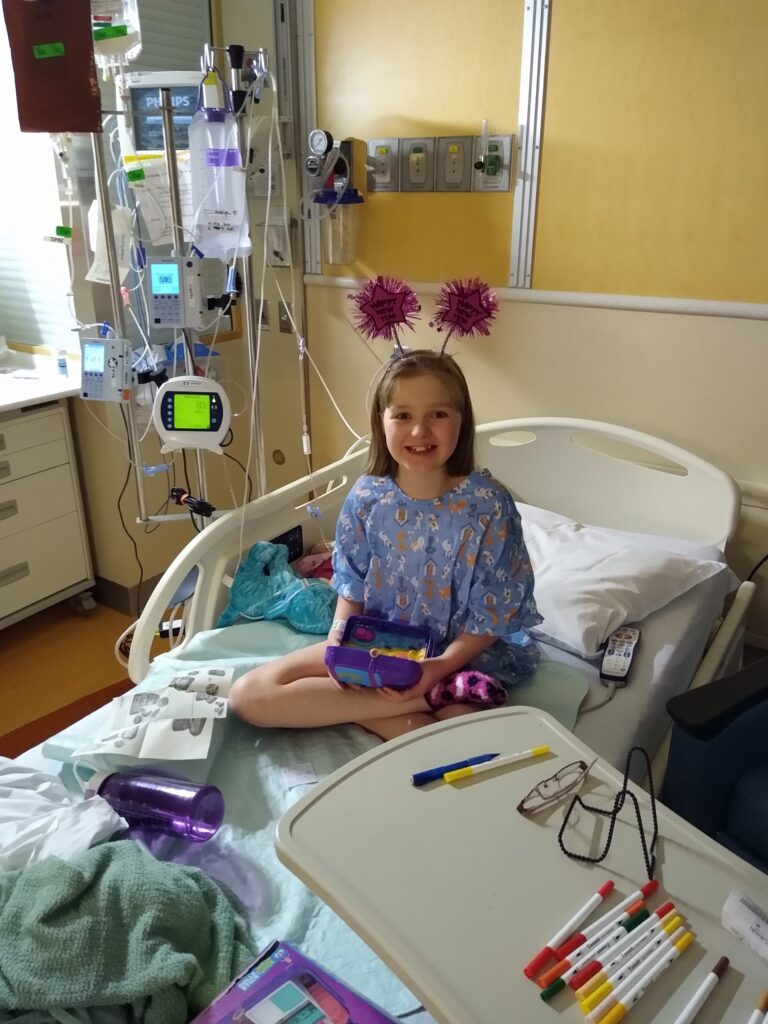
Over the past 12 years, Andalyn and I have endured 565 days in the hospital which includes 71 ER visits and 63 admissions at 7 different hospitals in 5 states. She’s been put under general anesthesia 86 times, had 35 surgeries, 34 upper GI studies, 27 endoscopies, and 2 colonoscopies. She has had 28 central lines; half of which I have taken care of. This does not include the days spent going to appointments, tests, and procedures. I wish providers understood the things they unknowingly, and often unintentionally, do that make being in the hospital harder than it has to be.
I wish they would try to meet me where I am instead of pushing me to where they think I should be. If they could see the wounds that never quite heal and feel the weight of unresolved trauma I carry it would make all the difference.
I wish they knew how broken I am from 12 years of worrying about how long my child will live and how scared I am that she will not survive her intestinal failure. She has almost died many times already, mostly from medical errors or “extremely rare and unlikely” medical events. If they knew all that we have been through, they would understand why I argue or push back over a “gut” feeling and they would not be so quick to assume I am just being anxious or difficult.
I wish they knew I live in increments of time dictated by a medical care schedule. I mark my days in terms of care to be done, medications to give, pumps and infusions to manage, and medical issues to coordinate – not in minutes and hours. As interventions are adjusted, I fear the impact those changes will have on my child’s already difficult life. So when I make a big deal over a little thing, this is probably why.
I wish they knew it is incredibly difficult for me to trust a provider that doesn’t know us. I know it means I will have to work three times as hard to get Andalyn the things that work best for her especially when they don’t fall within the standard practice. Even the smallest decisions can profoundly impact our quality of life and seemingly insignificant things have resulted in deep trauma for us. This is why I get angry or appear to overreact to minor things. In truth, I am probably exercising incredible control and what they see is nowhere near the depth of feelings I am battling.
I wish they knew I am constantly moving from one familiar trauma to the next, with unfamiliar traumas in between. New traumas emerge as complications arise and treatments compound needed interventions. This unceasing torrent of misery creates a whole new kind of PTSD. It’s not Post Traumatic Stress Disorder because “Post” implies the trauma is in the past; over and done. For me, that’s inaccurate. The intensity certainly fluctuates between tolerable and intolerable but my trauma is relentless, ongoing, almost constant. It’s definitely not in the past and it most certainly is not going away in the near future.
I have traditional PTSD for sure, but I also have what I call Persistent Traumatic Stress Disorder. Persistent traumatic stress isn’t so much “triggered” as endured since being triggered requires a period of time when you are not experiencing trauma. In persistent traumatic stress, you can’t unexpectedly re-experience something that never really stops in the first place, so “unexpected” gets replaced with “anticipated” when conditioned by persistent trauma.
I wish they knew that I am very good at pushing down feelings and using distraction and the ever compulsive need to keep moving as a protection from my own pain so I can help my child through hers. It is most often the little things that bring me to my knees when somehow they fracture the vault where I lock my deepest pain. The vault I created in order to have the strength to keep moving forward, since feeling the intense emotions from persistent trauma steals too much energy from the tasks of fighting, surviving, and advocating. This is probably why I seem fine managing really complex issues but fall apart over simple ones.
I wish they knew I feel totally overwhelmed despite the confidence I project. When I am alone in the chaos and all around me there is nothing but quiet, the feelings emerge from the vault and mercilessly threaten what little composure I manage to fake in my daily routine. Feelings destroy the illusion of control; the picture of strength the world sees from the outside looking in. Feelings expose the gaping wounds of my soul that allow the hope to escape in my most broken moments. Feelings become my strength’s undoing.
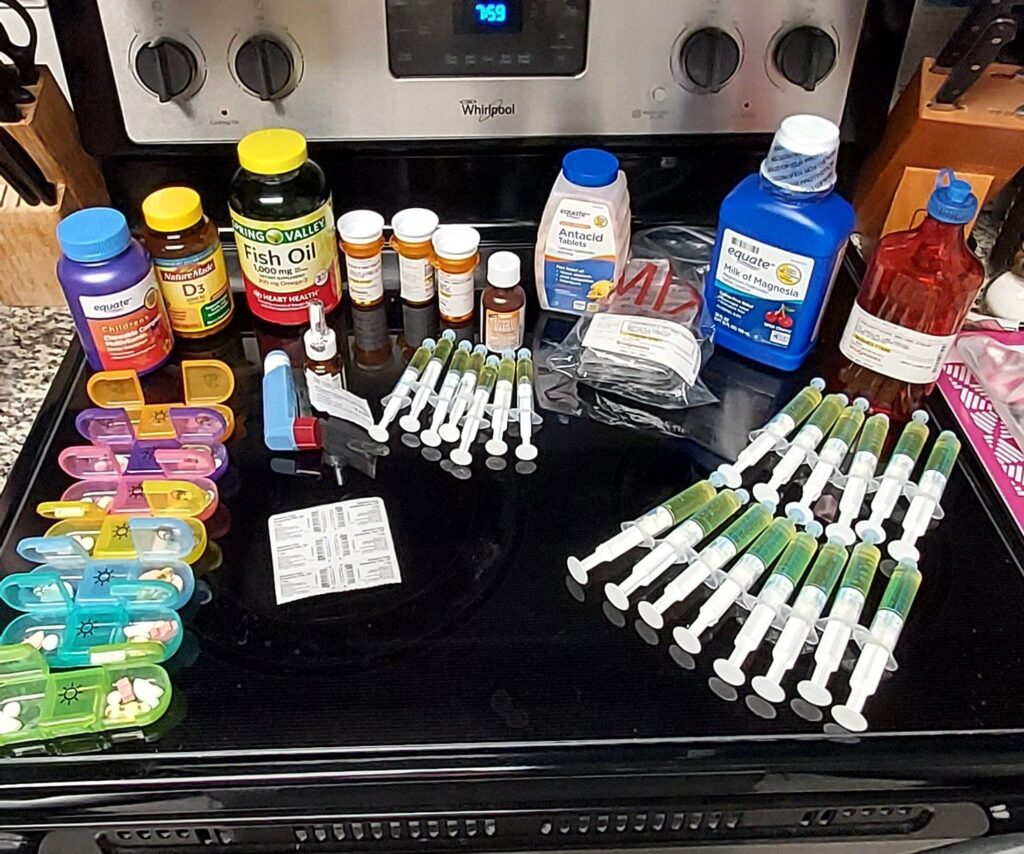
I wish they knew that the complexity of managing her condition – the continuous feedings, the special diets, the vomiting and pain, plus the weight of just not knowing, have pulled more from me than I thought I could give. I struggle with feeling like a failure because I couldn’t get her the nourishment she needed.
I wish they knew I have been required to do things to my little girl that were traumatic for her and that ripped my heart to shreds as she begged me not to do the things I must. I have held her down to place NG tubes, give terribly painful injections, and clean infected wounds all while she screamed and cried. Seeing the betrayal in her trusting eyes as the person who was supposed to protect her became the one that wounded her, made a piece of me die. It is devastatingly painful to be forced to damage your child’s soul in order to protect her body.
I wish they knew I hate having to be my child’s nurse because it steals all the time I wish I could just be her mother. I don’t even realize how vigilant I have become because I have forgotten how not to be. Waterproofing the central line for daily showers results in emotional meltdowns for her every time. Instead of splashing in bubble baths with playful laughter, it’s hurried showers with anxious fear. Fear that a leak in the carefully constructed waterproofed dressing will allow another life threatening infection to creep into her bloodstream. So as her nurse, I have to be vigilant.

I wish they knew I have come to hate Sundays because that’s the day we do dressing changes. Too many times I have to ignore her cries of pain and pleading. I blink back my own tears so I can see to clean the blistered, broken, and bleeding skin from severe allergies that torture her if I don’t do everything exactly right. So as her nurse, I have to be perfect.
I wish they knew there are no dance classes because ballerinas can’t turn and leap when connected to IV poles and heavy medical backpacks just don’t go with pretty pink tutus. Too many doctor appointments mean there isn’t time for soccer practice. Medical needs have to be prioritized ahead of everything else in our lives. So as her nurse, I have to make hard choices.
I wish they knew that every fever and admission for IV antibiotics, cultures and blood work makes me relive the times she almost died. Just being in the hospital makes my anxiety unbearable. I’m so afraid of getting judged by providers as being difficult that I feel ill every time I advocate for her. I wish they knew that the repeated admissions, appointments, pumps, IV poles, medical backpacks, lack of sleep, and overwhelming supplies for infusions and line care, are all harsh reminders that I don’t get to be her mother as long as she needs me to be her nurse. So as her nurse, I have to be unbreakable, but as her mother, I weep.
________________________________________________________________________________________________________________
About Amanda
I live in Aurora, Colorado with my 12 year old daughter, Andalyn. I am divorced so I am navigating this journey as a single parent. We came from New Mexico in 2014 so that Andalyn could get the medical care she needed at Children’s Hospital Colorado. After spending 15 months in the Ronald McDonald house, we officially became Colorado residents when we moved into an apartment. Andalyn has complex medical needs and multiple challenging diagnoses. I have spent her life striving to make things for her as normal as possible because so little of her world is in our control. I have no idea how much longer she will get to be here but she has already lived far longer than many suspected she ever would. I survive most days on Diet Dr Pepper, sarcasm, and a little bit of dark humor sprinkled in for good measure. I am a very sensitive soul that feels all things deeply but I have found a way to thrive through the power of connection. That connection is what makes it possible for me to do impossible things for as long as they need to be done.
Initially, I was hesitant when Andalyn’s pediatrician suggested palliative care. I was scared by the implications. I didn’t understand the role of palliative care or how it would fit into Andalyn’s treatment team. Fortunately, her pediatrician sensed my discomfort and quickly offered clarification. I mistakenly thought, as most people do, that palliative care was the same thing as hospice. It is not. Palliative care is about maximizing quality of life and symptom management. It’s about shared decision-making, care coordination, and honoring your values. It’s about figuring out what’s important to you and where your boundaries are. Palliative care is about finding your voice and learning how to advocate for your child and for yourself.
I was already very good at advocating for Andalyn but I never dared consider the idea of advocating for myself until a palliative care doctor came into my world. Her medical team frequently anticipated problems offering solutions before I could even ask for help. Even so, there was a lot I never said either because I didn’t know exactly what I needed or because I was too scared I would be misunderstood. I have learned the hard way that in the medical world big feelings and too much honesty have a way of making boundaries and invisible walls appear where openness and comfortability once was. Palliative care became a valuable resource facilitating communication with her medical team, especially around difficult topics, so my needs could be better received.
One of the hardest things for me to convey was an unfamiliar kind of grief. I was drowning in a profound sense of loss that I couldn’t explain or talk about. I didn’t understand how I could be grieving so deeply when my daughter was still alive. This soul-sucking pain stretched from our past into our present, while somehow also projecting into our future. It is strange to mourn for what you have lost while simultaneously grieving what is happening right now and aching for what never will be.
Our palliative care provider and her pediatrician have become my guides on this journey back and forth across the bridge of borrowed time. A bridge that connects where Andalyn and I are now, to where I am afraid we will end up, long before I am ready. Not that you can ever truly be ready for something as awful as losing your child. They remind me that these things I struggle with are normal and in some ways, even expected. They provide me with much needed reassurance that my questions and fears are valid and don’t mean I am being dramatic. I am incredibly grateful that in especially difficult conversations the things I can’t quite figure out how to voice are somehow still understood and validated with sincere compassion and empathy.
Palliative care also provides crucial support as I work through the painful process of trying to accept unimaginable things. One of the hardest being the reality that we have pretty much exhausted every intervention available in our hopes to “cure” Andalyn. Palliative care is helping me to make the very painful shift from cure to comfort; from hoping someday she will have a normal life, to trying to make the life she has as normal as possible.
In making this shift, I need to voice my fears without being told things like, “don’t think like that” or “we will cross that bridge when we come to it”- well meaning but useless sentiments. I need someone willing to sit with me in the uncomfortable moments; someone who can help me process my fears around the potential death of my child. I need to ask the questions my mouth refuses to utter but my heart screams anyway. I need someone that knows how to guide me through the places that no parent should ever have to go.
Despite all my pain, grief, and shifting expectations, I know palliative care is not about giving up or losing hope; even though hope looks very different for me now. I no longer hope for what I have come to accept as unrealistic expectations. Hope has changed into trying to have as many good days as possible with the fewest regrets. Hope is now centered in trusting her providers to work with me as I advocate for Andalyn in all the ways that matter, for as long as she needs me to.
I now understand how palliative care helps me see things from a different perspective and empowers me to make purposeful decisions. Decisions that feel right in the very deepest parts of my soul even if someone standing on the outside could never understand how I could make such choices. Palliative care is about having help to evaluate which interventions no longer make sense and which risks are worth taking in order to create moments of joy for Andalyn that she otherwise wouldn’t have. Palliative care is helping us find the balance between living for interventions and doing interventions so she can live.
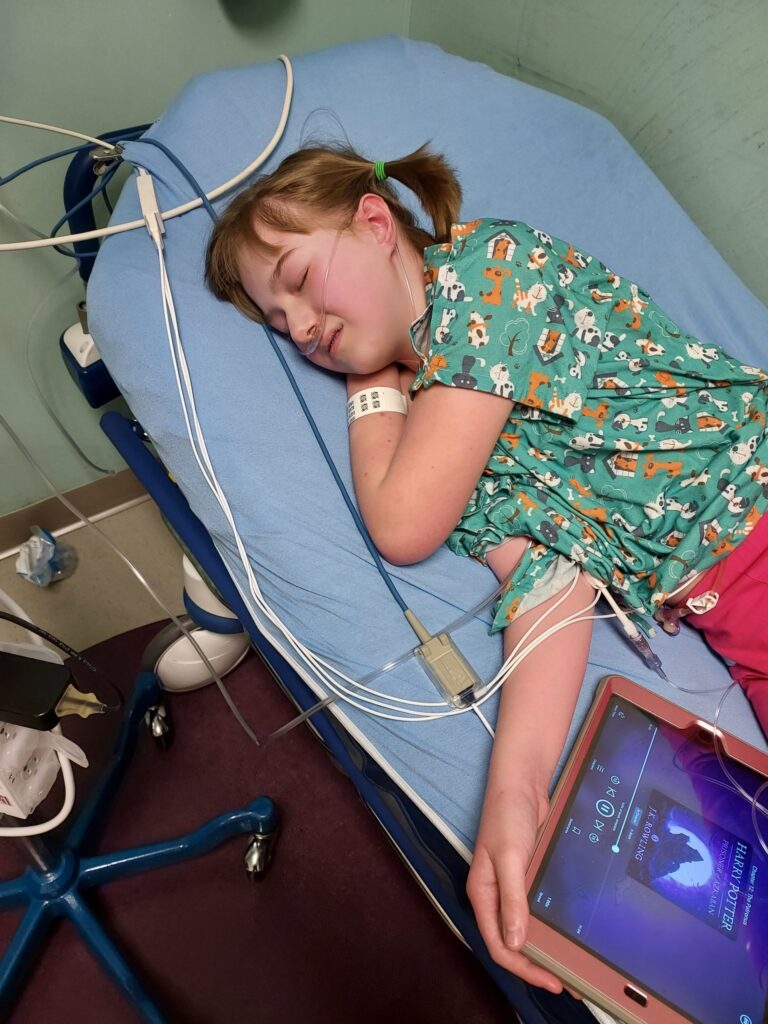
Recently, for example, I asked if Andalyn could be allowed to go swimming. She has loved being in pools, baths, or any other water play as long as I can remember. It devastated her when she was told at just 4 years old that she could not do those things again until she no longer had a central line. The reality is she will likely always need a central line. So I did some soul searching.
I sobbed my way through the entire conversation with her pediatrician as I asked for his recommendations to mitigate the risks of swimming with a central line as much as possible. I told him how important shared decision making is to me. I cried so hard I am not even sure how he understood anything I said but he listened patiently and without judgment.
I left that appointment with a promise that he would get back to me with his recommendations around swimming and a sense of peace knowing he understood my need to create joy for Andalyn. If something terrible happens as a result, I will cling to that peace and remind myself that I had support from her team. Most importantly, I will remind myself that I gave her a voice in how she got to live.
For me, palliative care has been about finding validation and a safe place to talk through the things I’m not supposed to say out loud and to process the inevitable shifts in my child’s baseline. Most of all, palliative care is lending me the courage to keep fighting, especially when fighting looks a lot like letting go.
________________________________________________________________________________________________________________
About Amanda
I live in Aurora, Colorado with my 12 year old daughter, Andalyn. I am divorced so I am navigating this journey as a single parent. We came from New Mexico in 2014 so that Andalyn could get the medical care she needed at Children’s Hospital Colorado. After spending 15 months in the Ronald McDonald house, we officially became Colorado residents when we moved into an apartment. Andalyn has complex medical needs and multiple challenging diagnoses. I have spent her life striving to make things for her as normal as possible because so little of her world is in our control. I have no idea how much longer she will get to be here but she has already lived far longer than many suspected she ever would. I survive most days on Diet Dr Pepper, sarcasm, and a little bit of dark humor sprinkled in for good measure. I am a very sensitive soul that feels all things deeply but I have found a way to thrive through the power of connection. That connection is what makes it possible for me to do impossible things for as long as they need to be done.
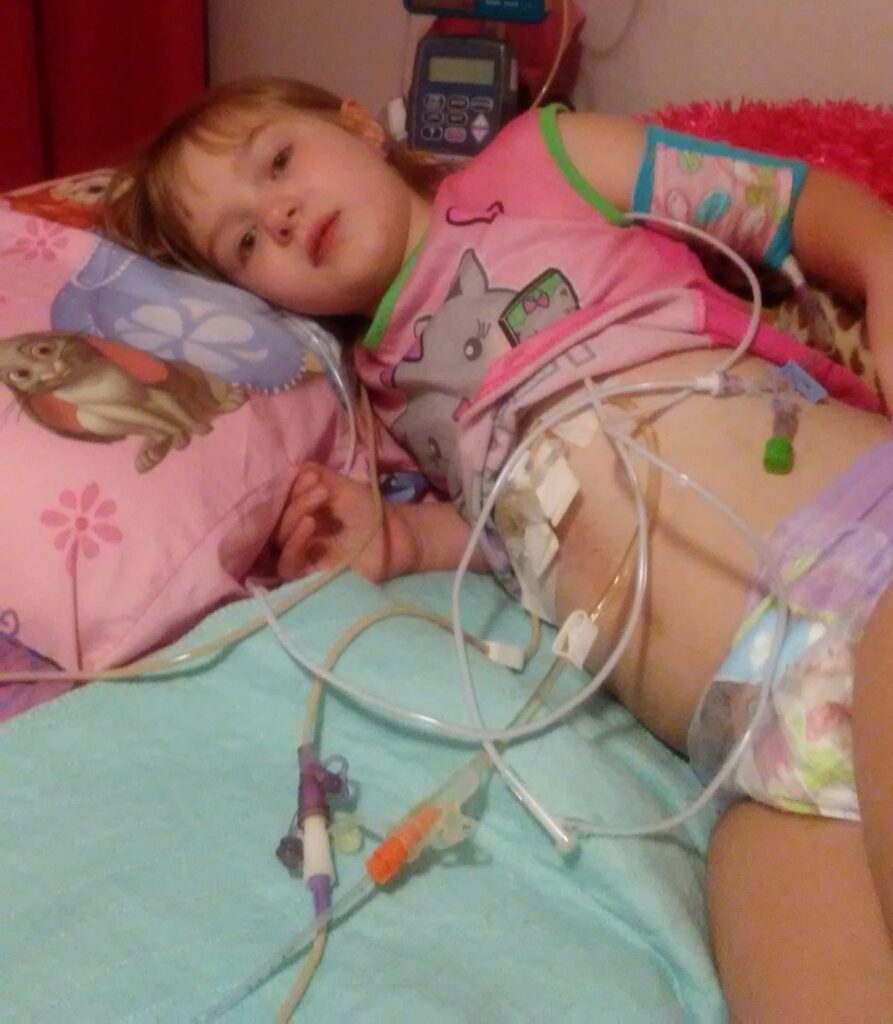 People often tease me about being a pessimist. They aren’t wrong about that. They are just wrong about why. They don’t understand that I became a pessimist because constantly hoping for the best became too painful to be sustainable at some point. For me, preparing for the worst softens the blow just a bit. It allows me to protect myself ever so slightly from the devastation that comes with inevitable shifts in Andalyn’s baseline. Hope is still part of my journey just not in the way it used to be.
People often tease me about being a pessimist. They aren’t wrong about that. They are just wrong about why. They don’t understand that I became a pessimist because constantly hoping for the best became too painful to be sustainable at some point. For me, preparing for the worst softens the blow just a bit. It allows me to protect myself ever so slightly from the devastation that comes with inevitable shifts in Andalyn’s baseline. Hope is still part of my journey just not in the way it used to be.
It is hard having to navigate all the things that caring for a chronically ill child involves. Finding emotional support can be surprisingly difficult. I have been misjudged and invalidated enough that now I am careful how and where I seek support. Sometimes people say I’m a negative person and if I had a more positive outlook things would get better. But that is not how intestinal failure works. I wish they could see that my nature is not actually negative. The truest, deepest parts of my soul are full of enthusiasm. Those parts have just been weighed down and buried under a lifetime of pain and trauma. They hide as a matter of self preservation, but they are still in there.
Other times people say I don’t focus enough on the positive aspects of my life and if I did things would get better. But that is not how trauma works. I wish they could see through the chaos to recognize that the only way I survive is by feeding my soul tiny crumbs of joy. I can only move forward when I have something to move toward so I have mastered finding ways to focus on the positive, but it will never be enough to overshadow the pain. Focusing on the positive pulls me through pain, it doesn’t eliminate it.
The hardest times for me are when people say I am just not a happy person and suggest I could choose to be happy if I really wanted to. But that is not how grieving works. This assumption is misguided but understandable coming from those who have never walked this path. I wish they could see that for me, happiness gets mixed up and diluted in all the trauma and pain. I visit happiness every chance I get, I just don’t get to live there anymore. My child’s illness moved me out of the land of happiness and into the land of anticipatory grief the day that I realized that she could die.
Anticipatory grief is a land of shifting baselines and a place you live while a loss is still unfolding. It is a place where pain gets peeled back and all the different layers of your loss are exposed. It is filled with missed milestones and unmet expectations and no one can truly join you except for those who already live there. In the land of anticipatory grief the price you pay for hope is paid with pieces of your soul.
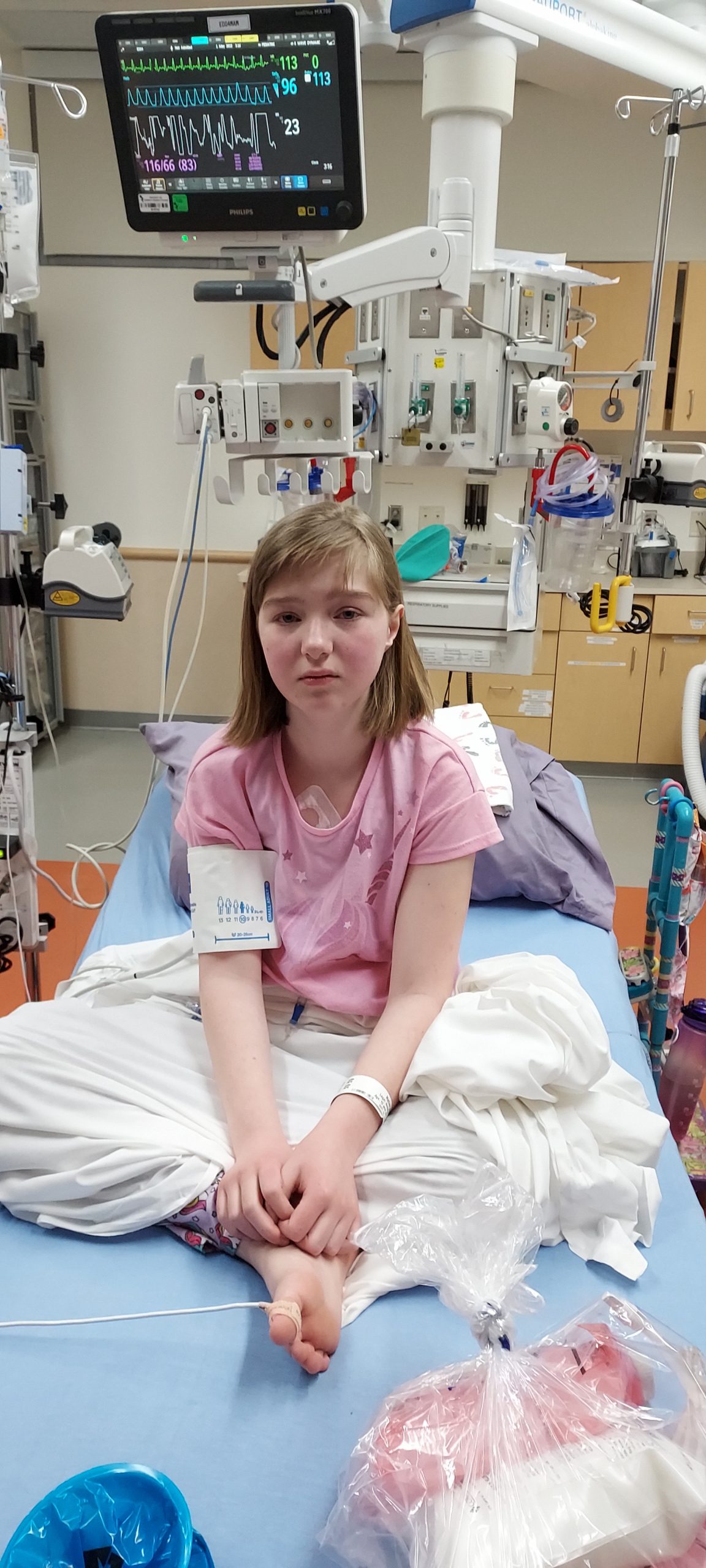 In the land of anticipatory grief, I find myself feeling torn between the heartbreak of letting go of what I wish could be, and trying to accept what is. For me, it is a place I have been coming to terms with all Andalyn and I have lost and that never will be, while also trying my best to live in the moment. Anticipatory grief is a place where I learn how to absorb unimaginable things and yet somehow find the strength to keep moving forward for my child.
In the land of anticipatory grief, I find myself feeling torn between the heartbreak of letting go of what I wish could be, and trying to accept what is. For me, it is a place I have been coming to terms with all Andalyn and I have lost and that never will be, while also trying my best to live in the moment. Anticipatory grief is a place where I learn how to absorb unimaginable things and yet somehow find the strength to keep moving forward for my child.
For a long time after we came to Colorado it felt like an endless stream of procedures, tests, and surgeries. We tried everything to understand the nuance and complexity of Andalyn’s intestinal failure. As my relationship with her team of providers grew stronger, so did my trust and willingness to step outside my comfort zone and allow myself to be led when the path forward was unclear. And it seemed to be unclear a lot. Every time we got a routine that I could almost remember without alarms and written schedules, something would shift and we had to start over from scratch. Each thing we learned or discovered, sometimes by accident, revealed another small part in a nightmarish puzzle with shape shifting pieces. I hoped if we could discover the ‘what’ and the ‘why’, surely the ‘how’ to fix it would follow but it was an endless pursuit for answers that never materialized.
With each new treatment, surgery, or intervention, I would desperately cling to the hope that this would be the magic thing that would turn our world into something normal but the truth has a way of unwinding dreams without regard for vulnerability. The twisted mess of vacillating between hope and devastation broke my heart again and again and I grew weary under the suffocating weight of repeated disappointments. The reality that Andalyn might not survive her intestinal failure sank deep into my soul and is never far from my awareness. Living with a central line and TPN dependence requires hypervigilance, sacrifice, and the willingness to accept deadly risk. It is tragically inconvenient to have to embrace the intervention she needs to live, knowing most likely that it will be the thing that kills her. Letting hope weave its way through your soul takes intentional bravery, but hope is a slippery thing to hold on to when it gets tangled in reality.
________________________________________________________________________________________________________________
About Amanda
I live in Aurora, Colorado with my 12 year old daughter, Andalyn. I am divorced so I am navigating this journey as a single parent. We came from New Mexico in 2014 so that Andalyn could get the medical care she needed at Children’s Hospital Colorado. After spending 15 months in the Ronald McDonald house, we officially became Colorado residents when we moved into an apartment. Andalyn has complex medical needs and multiple challenging diagnoses. I have spent her life striving to make things for her as normal as possible because so little of her world is in our control. I have no idea how much longer she will get to be here but she has already lived far longer than many suspected she ever would. I survive most days on Diet Dr Pepper, sarcasm, and a little bit of dark humor sprinkled in for good measure. I am a very sensitive soul that feels all things deeply but I have found a way to thrive through the power of connection. That connection is what makes it possible for me to do impossible things for as long as they need to be done.
Having a child with a rare progressive disease is like a lifelong train ride…
Every family affected gets their own train car. You see, all of the cars are connected. Like all of the families with the rare disease. At first, you don’t know where the train is going. But you get on it because, let’s face it, you don’t have a choice.
You make friends with the other people in their cars and all try to learn from each other…not about the destination, but about the ride. You become close, because you share a journey that few others in the world understand. And the more you learn, the faster the train picks up speed. And you don’t know when the train ride will end, but you know that eventually it will be your stop.
But you don’t want the train to stop. Because this ride doesn’t have a happy ending. So the train ride you never wanted to be on now has a hint of terror every time you hear the brakes squeal. Maybe these are just bumps in the track. But you’re optimistic because hey, what choice do you have? This bump was just a surgical procedure or a short hospital stay. This wasn’t your stop. The train picks up speed again. Then all of the sudden BAM.
The train car behind you gets hit by a bus and the one in front of you is flooding. The whole train feels the shock. You’re okay this time, but it’s your friends in those cars. You have a friend in every car. You know the cars well, because they are just like yours. You can’t help them anymore because this was their stop, so you try to help the other passengers. The pain of this crash belongs to every person on the train.
And the train keeps going. Bumps and squeals and all. You keep trying to find a way off, but no one has figured out how to stop this train yet. Meanwhile, you get closer and closer to the others on the train. And somehow, you’re still grateful for this terrible ride and the time you get with all the people on it.
Yeah…having a child with a rare progressive disease is lifelong train ride.
________________________________________________________________________________________________________________
Lydia Anderson is mom to Warrick (age 8) and Raistlin (age 2 1/2). Raistlin was diagnosed shortly after birth with Multisystemic Smooth Muscle Dysfunction Syndrome (MSMDS), an ultra-rare disorder affecting less than 50 people in the entire world and was hospitalized for the first 26 months of his life. Since Raistlin’s birth, Lydia and her husband Warren have worked to cofound a non-profit organization to raise awareness of the disease (www.acta2alliance.org), and helped to organize the first meeting ever to bring together diagnosed families from across the world. Lydia and Warren now strive to help the affected families connect with medical professionals to help with the very rare and unique medical concerns of the MSMDS community.


