Courageous Parents Network interviewed a couple about how their faith affected end of life decisions for their infant daughter following her sudden diagnosis with Leigh’s disease. This interview first appeared in the American Academy of Pediatrics’ Section on Hospice and Palliative Medicine’s quarterly newsletter, August 2018.
***
Sophia: We have three boys. They’re now 13, 10 and 6. Since we got married, we always dreamed of having a girl even before we had our first child. Maybe because we don’t have any girls in our family. We had her name picked out before we even got married. Miriam. It’s unbelievable that we already knew her name.
When I got pregnant with our fourth child, I would have been happy if it was a boy too, but when we found out that it’s a girl, and everything is normal, I was so happy, I couldn’t even talk. I just started screaming into the phone. I said, “oh, my God, I have to call my husband, I have three boys, I can’t believe it’s a girl!” It was just unbelievable how happy we were. I called Ross, I was screaming, I couldn’t talk from happiness.
My pregnancy was absolutely perfect. All the ultrasounds were amazing. I usually don’t buy things before the baby, but I bought a few outfits. I was just so excited that I can finally buy pink things. I got really cute things for breastfeeding, the cover-ups, with flowers. It was my last baby. I was 40 years old. It was like a gift for me. I thought I was making a major gift for myself.
When she was born and I saw her, she was absolutely beautiful. I couldn’t believe it. It was like I designed her myself. I remember calling my parents and saying, she’s so beautiful. And Ross called his parents and I remember him saying, she’s so beautiful. We felt so complete at that moment.
Ross: I wanted to give her name in a synagogue right away. It’s a whole religious naming ceremony. Everyone had come in. Someone said, oh, this is the first time Zilber boys can produce a girl. And everyone was laughing.
Sophia: It’s amazing that Ross insisted on doing naming in a synagogue for her so soon after birth. Looking back, it must have been a sign because if we waited longer, a month later she was already in the hospital and unconscious. She was here for such a short time, but at least we had a naming ceremony and a party for her.
From the beginning, something wasn’t quite right with Miriam because she wasn’t really breastfeeding. I always had a such a good experience breastfeeding my boys. I told nurses in the hospital when she was born that this is my fourth child and it was so different before. I didn’t think it was anything serious. I had no idea even that these diseases exist. I was so naive. They just kept saying that she’ll figure it out, sometimes it takes a little longer. And then she didn’t gain weight as much as she should have, even though she wasn’t losing weight either. So it tricked the doctors, I think because I was working very hard on feeding her. I literally was feeding her 24×7. I would go to the pediatrician almost every day to weigh her. Eventually I had to switch to a bottle. But she wouldn’t take the bottle either, which I showed to the pediatrician. She said, keep working really hard, keep working harder. And these doctors are so experienced, our practice is so experienced. Looking back, I just can’t believe that they didn’t think something was wrong.
The first few days she cried a lot, but then she went to the other extreme. She stopped crying. She was so lethargic and she would always sleep. I called my pediatrician and asked, are you sure it’s okay, she was crying so much and now she’s too calm, she’s not crying. And my pediatrician said, well, she’s just happy with everything.
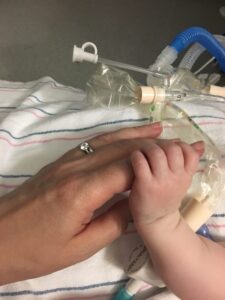
One Friday afternoon, I told the pediatrician, maybe I should take her to Children’s Hospital just for them to look at her. I felt very uncomfortable going into the weekend when I couldn’t feed her. The pediatrician looked at me and said, there is really nothing for them to check. So I went back home; I felt so helpless. On Sunday morning her skin felt very cold. I didn’t realize at the time but her body temperature was dropping. She was actually dying, which we didn’t know then. We gave her a bath, which was crazy, because I thought it’s going to warm her up. She slept through the bath. Water was pouring on her and she was sleeping. After the bath, I noticed that her hand was puffy, like there was some fluid or liquid in it. I had no idea what it meant, but I felt some intuition. I just thought I have to take her to the doctor now, something is going on. When we got to the doctor, she called the ambulance right away because Miriam’s vital signs were all horribly low.
Ross: When we got to the hospital, they were waiting for us and started running around, like on a show. They put her on life support for her breathing. They told us most likely it’s an infection.
Sophia: We have a friend who is a doctor and he was texting with us late at night. I remember texting him that doctors said if it’s not an infection, it’s a metabolic disease. And he texted back, well, that’s very rare, you shouldn’t think about it, that almost never happens.
Next day they did an MRI. They called us into a meeting with the doctors. They said they want to talk to us about the MRI. When we came in, we saw a very long table with many doctors there and social workers and nurses. They all stood up and didn’t sit down until we sat down. And when I saw that I thought, oh, my God, something is very wrong. And then the neurologist said, we want to talk about the MRI with you.
That meeting plays in my mind still — forever. Every word of that meeting — it’s still playing in my mind. The doctors told us that that it’s mitochondrial disease. They were very pessimistic. They told us that it has no cure or treatments. But it was good that they told us the truth. We wouldn’t want to be given false hopes.
Ross: They are able to see high lactic acid in her blood and they were able to see high lactic acid on the MRI in her brain. They didn’t know yet which exactly disease it was. Later we knew it was Leigh’s Disease.
Sophia: They told us that if Miriam starts breathing she would come back home, but her life would be very short. At that point I was thinking about my boys and what it would do to them to have her back at home, knowing it was only a matter of time.
We went home and told the kids that Miriam is very sick. We told them that she might not get better. It was truly the worst thing I had to tell my kids. I broke their hearts completely. They wouldn’t stop crying for most of the night. It was killing me that I had to hurt my children this much. But I had to tell them the truth because I had to prepare them. And they started praying for her. They prayed for her so much, really. Especially my older son, who was 12. He would just pray for her for hours.
Our friend is a neurologist. She told us right away that Miriam most likely has Leigh’s Disease. She also told us if Miriam starts breathing and comes back home it’ll be a “different Miriam”. She told us that Miriam’s hand was likely puffy because she was retaining fluid.
Sophia: In a few days they did another MRI on her and it had gotten so much worse. The neurologist was crying and told us that Miriam is dying.
The doctors said that we could remove the breathing tube.
We talked to our Rabbi. First, we asked what are we supposed to pray for now that they told us she’s definitely dying. Can we really still pray for recovery? What do I tell the kids because they are praying so much and it’s helping them to pray? He recommended telling the kids that God already made his decision for Miriam, but they could pray for strength, they could pray for God to do his will. That was very helpful for us because it helped us accept what was happening, but still pray.
Next, about the life support — our Rabbi told us that by the Jewish law, we really can’t take out an intervention that’s already there. He also consulted with another senior Rabbi and they really took it very seriously. If she had never received life support, we wouldn’t have to give her breathing tube, but now that she had it, it should not be removed.
Ross: Actually, they would have recommended not to intubate her in the first place, if they knew her diagnosis.
Sophia: One nurse asked us, Does your Rabbi think that she’ll recover? And I said, No, he understands, we know that she’ll die, but we’ll just let God take her away and not do it ourselves because if we are the ones that pull out the breathing tube then we are technically taking the action to end her life. Our Rabbi recommended we shouldn’t take active actions to shorten her life, but we also shouldn’t take active actions to prolong her life. For example, once her blood pressure starts falling, we don’t have to give her medication. We signed the DNR.
Ross: Rabbi was there every day and all the time he was consulting with the senior Rabbi in New York.
Sophia: It took a month, a little over a month. That was absolutely the hardest month ever. We knew that we could always technically stop.
Ross: We could do whatever we wanted to do, it was still our decision as parents.
Sophia: Our Rabbi was in the hospital almost every day for hours. If I texted him that I’m really upset, he would just drive there. 15 minutes later I would just see him in the room.
Ross: I think the doctors and nurses didn’t completely understand why we wouldn’t just stop her life support. They could see it that it was very difficult. They would talk to us at different times. One time they said we just want to talk to you without your wife. When I met with them, I told them that, in this type of matter, my wife and I make decisions together, and are on the same page, so there is absolutely no point for you to meet with me separately or schedule a meeting when she’s not there.
Sophia: It took a lot longer, way longer than anyone could have expected. And I think they did see that it was difficult, and I think they were respectful and trying to understand our perspective.
Ross: They could see that it was very hard for us to be there and they cared a lot about us. The Rabbi was helping the whole time. He said whatever decision you make, you are the parents. You don’t have to follow my advice. But this is my advice — he did say that right now it’s difficult, but later you’ll look at it and you’d feel better about it that you had time to say goodbye, you had time to make peace with it.
Sophia: I don’t feel upset at the doctors. They had the best in their heart.
Ross: It was important for us to do what we thought is the right thing to do. These are extremely difficult painful decisions, at some point less medical and more moral decisions. We wanted to make sure we can live with these decisions for the rest of our lives. At the end of the day we feel we did the right thing, and having that time helped us transition in the grieving process as well.
Sophia: I remember a nurse at some point said that if it drags out too long, we’ll have to have a hospital ethics committee talk about it. But honestly, I didn’t get upset with her because I knew she cared.
Sophia: There was one doctor that was more insistent on taking out the breathing tube, especially towards the end. She actually had two siblings who died from Leigh’s Disease, so she was very affected by the fact that she now was taking care of a baby with it. She really cared, but it was also upsetting for her. But after Miriam died, we got a card from her and she wrote that, “your courage and conviction as a couple and your faith were so evident”. She wrote, “You touched my heart.”
Sophia can be reached at sophiazilber@gmail.com