In January 2020, we were told our son Lucas had few medical options left and that we had months not years left with him.. 2020 has become so closely associated with Covid-19 that it is now hard to recall that the first two or three months of the year were relatively worry-free for most Americans. It was never worry free for us. We didn’t begin our new year with a feeling of optimism for what lay ahead unless it was the delusional optimism of a bargainer as we asked, “When the urologist said months not years, he could mean 11 months right?” Lucas had Menkes Syndrome. It is a copper transport disorder so not only does insufficient copper reach the brain but too much collects in the kidneys. At this time, we had just come through a particularly rough December of kidney issues for Lucas. We were in and out of the hospital, Lucas endured sleep studies and we discovered he would now need supplemental oxygen at home. It was clear December was a decline for him and a new year did not offer new hope.
So by March when Covid-19 became something most of us could not ignore, we took it very seriously. Mindful of Lucas’ increased vulnerability and that our clock of months not years was ticking down, we determined to strictly isolate our family of four (five if you count our home care nurse). We pulled both boys out of school before the district made the call that schools should close. I was the only one to leave the house for grocery runs and our home nurse went heroically above and beyond her duty electing to isolate away from her own family, including her toddler granddaughter, rather than increase the risk to Lucas or leave us without care at home.
Lucas actually loved this period of time. Non-verbal, it’s always a guessing game to know what he’s thinking but I’d lay odds he wouldn’t know the difference between a Wednesday and a Saturday except that he definitely did know and appreciate the difference between a day when people went to work and school and a day we spent at home all of us together. Covid-19 meant so many more days of all of us together. We could see Lucas delight in that. Whenever he’d see us earlier than 4pm he’d light up or crack up laughing, as if to say “You’re not usually here with me at this time.”
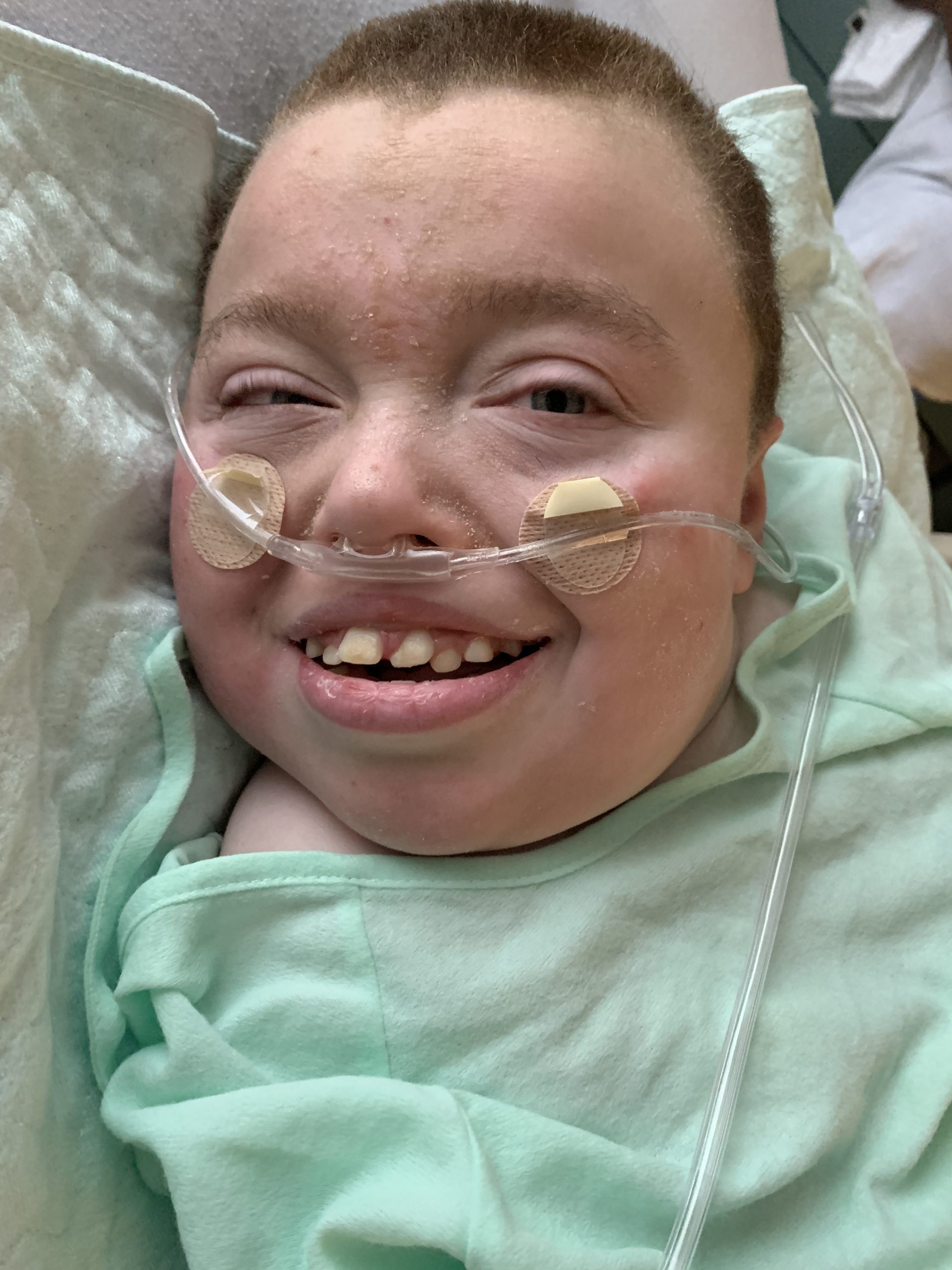 And I am actually able to be grateful to Covid for this time, if that’s possible. Many of us have thought through: “If you knew you were going to lose someone you love, what would you do differently?” Maybe for most it’s a theoretical exercise but the answer more often than not includes something about spending more time together. Well, it wasn’t theoretical for us. We did know and our lockdown lifestyle meant we got to spend a lot more time with Lucas than our typical days allowed.
And I am actually able to be grateful to Covid for this time, if that’s possible. Many of us have thought through: “If you knew you were going to lose someone you love, what would you do differently?” Maybe for most it’s a theoretical exercise but the answer more often than not includes something about spending more time together. Well, it wasn’t theoretical for us. We did know and our lockdown lifestyle meant we got to spend a lot more time with Lucas than our typical days allowed.
As we learned more about Covid-19, it seemed uniquely tailored to threaten our son. Boys with Menkes are susceptible to pneumonia, in fact that is often how they die. Boys with Menkes have twisted (compromised) blood vessels and as we learned Covid-19 might be a vascular infection as well as a respiratory one, we took it as a given that if Lucas got Covid he wouldn’t survive it.
During this time, I recall an odd moment of feeling a bit fortunate that we had been able to secure home oxygen supplies. Just three months earlier I was more likely to curse the addition of an oxygen machine to our home. (In fact I wrote about this at the time and you can read that here.) Now this gear seemed a scarce luxury. Even better, our oxygen setup could refill its own tanks so we were not subject to the shortages for tank refills we’d begun to hear were growing more frequent.
The risk of contracting Covid was weighing on us when Lucas’s kidney problems once again grew acute. We were reluctant to bring him to a doctor or worse a hospital. We knew his remaining treatment options were few and affording diminishing chances of good outcomes. We tried to balance that with the chance of him contracting Covid. In hindsight, I can second guess that we may have waited too long to get him care. We were forced to decide which risk was greater – Lucas’ general decline if left untreated or the threat of Covid infection.
In May, a trip to the ER started to seem unavoidable. Remember what May of 2020 was like – New York City was the epicenter for Covid infections. And while we live in upstate New York about three hours north of the city, it wasn’t unreasonable to imagine the pandemic’s spread had reached our area more so than most of the country. We were apprehensive to go.
Like many rare families, experience had taught us that there was no such thing as a short hospital stay for our boy. Seven day stays were routine. I had begun think of the hospital as a twist on the Hotel California: “you can check in any time you like, but you can never leave.” Only recently had we discovered the power of palliative care, particularly when it came to reducing unnecessary time in the hospital. In New York state the paperwork with DNR instructions is printed on bright pink paper and often called “the pink sheet”. Having this sheet with you can radically alter the dynamics of medical advice versus what is medically required. I’d wave the pink sheet in front of the attending doctor in the PICU and shout “we’re going home”. Okay, in truth that only happened in my imagination, but I’d like to think the attitude pervaded our actual exchanges.
When it became clear we might need to head into the hospital, my first call was to our urologist, who we had a long, trusted relationship with. My next call was to our palliative care doctor. I recapped our situation and our reluctance and asked her to prepare for the battle to get us discharged as quickly as possible. From her impressive and expansive well of patience and wisdom she replied “It sounds like you need to be here right away.” She allowed no trace of alarm, her tone was always placid, but it still struck my ears like claxon.
Fortunately our hospital had recently built a separate ER for kids. It tends to be less busy than the main ER. Even so, they seemed close to capacity. Do you know what it looks like when you bring in a kid with high temp, shallow breathing, low tone, swollen blue-ish feet? It looks like Covid-19. We were kept in isolation and staff followed glove and gown protocols that looked to me like the clean room suits of an integrated circuit fabrication lab. Lucas was tested for Covid which not surprisingly came back negative. I was only checked for a high temp and lacking one, I was mostly ignored.
Lucas was admitted and the first of several surgeries was scheduled. My wife Tina and I have a system for extended hospital stays. We alternate nights with Lucas and at home. Each of us gets a chance for the comfort of home and a day at work and then we swap. But with Covid we decided not to trade off. I would be the one to stay for the duration. I’ll admit I thought this was a manly protector type thing to do asTina and Alex would be spared any exposure to Covid (unless Luke or I brought it home with us.)
Lucas, always stronger than we would credit him, pulled through one surgery and then another. Predictably our stay went from two days to three and then four. My wife argued she should relieve me but I thought it best for me to just stick it out. In hindsight, I see my position less as self-sacrificing and more as selfish. I was getting time with Lucas around the clock. I was seeing him smile for the first time in weeks. Tina and Alex were home worried and missing him. I could hear terror catch in her voice with each of my phone call updates. I knew her fear was not just that we’d lose Lucas but that she might not be there when we did.
Just as Menkes Syndrome had sometimes made our own home feel like a prison, now Covid was increasing that seclusion. There’s a reason we called it lockdown. And then to be in a hospital room during Covid, that only further constricts the physical and mental space we have left to us. It’s not the first time my stay in a NICU room has invited mental comparison to what a jail cell would be like. At night alarms and unannounced inspections interrupt my sleep. The room is perhaps 12 foot by 12 foot, the entry wall is glass and generally wide open. A limited moat of free space encircles Lucas’ bed and threads around the tray table I’ve commandeered for my laptop, his wheelchair, and all the hospital equipment. I pace that course until I’m dizzy, enough to shine the path on the floor if not carve a deeper channel in it.
Although I technically have the freedom to exit his room or the hospital, I’m loath to. In the best of times, we parents feel reluctant to leave our children’s rooms especially when our children cannot communicate on their own. Even a moment away for food or the bathroom rains guilt down –what if this is the critical moment? What if reaching me by phone is not fast enough? But Covid-19 has ensured these are far from the best of times and I am even more reticent to leave this room. I would risk not just my absence but the increased chances of contracting Coronavirus. Would that needed stretch of the legs or change of scenery bring the virus back with me to my son? The prison comparison grows more real. My tiny oasis is that recliner chair that almost converts to a bed.
Four days at the hospital turned into six, and one surgery expanded to four. But Lucas recovered from each and seemed ready to go home. The attending half-heartedly offered the option to stay one more night – “Nope, we’re going home.” I interrupted. Minutes later I heard him down the hall retelling that moment with a laugh “And the dad said Noooope, we’re going home.” That night home from the hospital was our last together as a family of four. He got our cuddles and we got his smile. The next morning Lucas awoke, struggled very briefly and left us before paramedics could arrive.
 For most of a year on our dry-erase board to-do list we had written “Lucas plan”. This was coded language for “plan Lucas’ funeral”. Since we were not active in any church, we knew we couldn’t rely on their structures and ceremonies. Like Lucas himself, his funeral would be one of kind. We intended to craft it ourselves. Despite these intentions, we never got very far beyond vague plans. Eventually we erased it from the to-do list still undone rather than let it grow ever more macabre. And then, as it turned out, Covid had one more cruel joke to play. Death during a pandemic will waylay even the best of funeral plans. The chance to gather loved ones and find comfort with them? Covid denied us most of that too. Friends and family did find other more socially distant ways to reach out. Dozens of small rocks were painted as Lucas memorials and placed on our porch. And thoughtfully prepared meals fed us for six straight weeks.
For most of a year on our dry-erase board to-do list we had written “Lucas plan”. This was coded language for “plan Lucas’ funeral”. Since we were not active in any church, we knew we couldn’t rely on their structures and ceremonies. Like Lucas himself, his funeral would be one of kind. We intended to craft it ourselves. Despite these intentions, we never got very far beyond vague plans. Eventually we erased it from the to-do list still undone rather than let it grow ever more macabre. And then, as it turned out, Covid had one more cruel joke to play. Death during a pandemic will waylay even the best of funeral plans. The chance to gather loved ones and find comfort with them? Covid denied us most of that too. Friends and family did find other more socially distant ways to reach out. Dozens of small rocks were painted as Lucas memorials and placed on our porch. And thoughtfully prepared meals fed us for six straight weeks.
 As we took stock of our new life without Lucas, we were honest enough to admit that some things were suddenly easier if in no way better. I mean on practical levels not emotional ones. Life with Lucas meant our ability to travel had been extremely limited for the past ten years (which was all of Alex’ life). It wasn’t too long before each of us voiced a silver lining that we could at last travel to those places we’d longed for, Italy, Prague, even Washington DC had seemed out of reach until now. But then Covid speaks up and says “No, not even this. Not while I’m around.
As we took stock of our new life without Lucas, we were honest enough to admit that some things were suddenly easier if in no way better. I mean on practical levels not emotional ones. Life with Lucas meant our ability to travel had been extremely limited for the past ten years (which was all of Alex’ life). It wasn’t too long before each of us voiced a silver lining that we could at last travel to those places we’d longed for, Italy, Prague, even Washington DC had seemed out of reach until now. But then Covid speaks up and says “No, not even this. Not while I’m around.
So yes, Covid made a bad time worse, but really we already had more than ten years experience with a disease rewriting our plans for us.