First published on Patient Worthy.
In medicine, baseline is a simple word. It’s a starting point; a reference used for comparison over time. Physicians document it carefully. Researchers rely on it. Clinical trials require it. But when your child is diagnosed with a terminal illness, baseline becomes something far more personal.
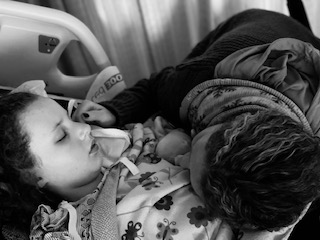
When my daughter Éabha was diagnosed with an aggressive brain tumor at age 10, I entered the world of pediatric oncology with a dual lens: I was both a registered nurse and her mother. I understood immediately why clinicians asked about baseline. Establishing a child’s baseline helps guide treatment decisions, detect complications, and evaluate disease progression. It is essential to good medicine. But living it is something entirely different.
 One day she was an energetic, creative, endlessly curious child. The next, we were standing in an intensive care unit being told to prepare for the worst. That day marked the end of the “baseline” we had always known. Before cancer, Éabha was vibrant in a way that filled every room. She was thoughtful beyond her years, fiercely loving, and completely devoted to her younger brother. Her laughter came easily. Her wit came quickly. Her energy felt limitless.
One day she was an energetic, creative, endlessly curious child. The next, we were standing in an intensive care unit being told to prepare for the worst. That day marked the end of the “baseline” we had always known. Before cancer, Éabha was vibrant in a way that filled every room. She was thoughtful beyond her years, fiercely loving, and completely devoted to her younger brother. Her laughter came easily. Her wit came quickly. Her energy felt limitless.
Then hydrocephalus, neurosurgery, biopsies, radiation, steroids, chemotherapy, complications, vision loss, weakness, and with each medical intervention came a subtle recalibration. A new version of our daughter emerged.
In pediatrics, baseline matters because children are still developing. Clinicians rely on parents to help distinguish what is normal growth from what signals concern. In pediatric cancer, especially brain tumors, that distinction can become lifesaving. A subtle change in coordination, increased fatigue, a shift in speech pattern, sleeping longer than usual, laughing a little less. These may be whispers of disease progression or treatment complications. But those whispers are rarely obvious. They live in nuance, and parents become fluent in that language.
Baseline isn’t static it is ever evolving. There was a baseline after surgery. A baseline after radiation. A baseline on high-dose steroids. A baseline during tapers. A baseline after shunt revisions. A baseline during stable scans. And every time we thought we understood it, it would shift again.
Monitoring her baseline became a constant, quiet vigilance. As a nurse, I had the clinical knowledge to recognize patterns. As her mother, I knew the cadence of her voice, the spark in her eyes, the rhythm of her walk, the subtle expressions that signaled something wasn’t right. Sometimes it was nothing, sometimes it was everything.
And yet, what makes baseline so difficult in pediatric cancer is not just the vigilance, it is the grief. When decline happens in children, what is often slipping away are pieces of identity. Children with neurologic cancers rarely decline dramatically overnight. The changes come gradually over time and to the outside world, these might appear insignificant. To us, they carried enormous weight. Because baseline is not only about physical ability, but it also encompasses personality, independence, humor, endurance, spirit. Each time Éabha’s baseline shifted, it was an acknowledgment that something had changed, perhaps permanently.
There is a particular exhaustion that comes from loving your child wholeheartedly while simultaneously assessing them clinically. I could understand the pathophysiology of increased intracranial pressure. I could interpret MRI reports. But nothing prepares you for realizing that the baseline you are now protecting would once have felt unimaginable.
Still, baseline was also how we held onto her. It was our early warning system. But it was also our sacred measure of who she was that day. It helped us know what kind of day it could be. Whether she had the strength for visitors. Whether she could sit outside and feel the sun. Whether we needed to advocate for medication adjustments or imaging sooner rather than later.
As her illness progressed, I came to understand that honoring a child’s baseline is honoring their dignity. When asked, “What is her baseline?” they were not simply collecting data. They were acknowledging her as a whole person, not just a diagnosis.
Éabha died at twelve years old.
And when I reflect on her life, I don’t think first about tumor markers or survival curves. I think about the steady courage she showed in a body that betrayed her. I think about the tenderness she extended to others even while suffering. I think about the quiet strength that carried her through days that would have broken most adults.
In the end, baseline was not just a clinical reference point. It was the story of who she was becoming, even as disease tried to define her.
For families navigating pediatric cancer, baseline is more than a word in a chart. It is the lens through which we recognize change. It is the language we use to communicate concern. It is often the first signal that something needs attention. When healthcare teams truly respect a parent’s understanding of baseline, they are doing more than practicing good medicine. They are entering into partnership with the people who know that child best. They are being invited into the most intimate understanding of that child’s life. That partnership can change everything.